CASE REPORT
Pekka Pohjanpelto1,4, Aki Kangasmäki2, Kalevi Kairemo2,3,*
1Päijät-Häme Central Hospital, Lahti, Finland
2Docrates Cancer Center, Helsinki, Finland ‘b’
3The University of Texas MD Anderson Cancer Center, Houston, USA
4retired
Abstract
The examination with lacrimal scintigraphy showed that the supine side-down eye position of the test subject inhibited the transfer of the tracer into the lacrimal sac. The result means that utilizing gravitation offers the patient a convenient alternative to prolong the ocular contact time of each eye drop.
Keywords: lacrimal scintigraphy; eye drop; head position; lacrimal drainage; topical administration
Introduction
The purpose of this study was to examine with lacrimal scintigraphy [1–3] whether using a supine side-down eye position inhibits the flow of an eye drop to the nasolacrimal passage in lacrimal scintigraphy (Figure 1).
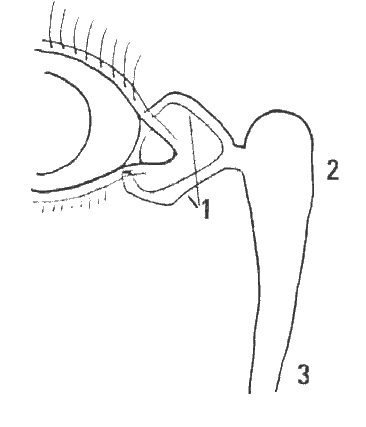
Figure 1. Lacrimal drainage system: 1) lacrimal canaliculi, 2) lacrimal sac, and 3) nasolacrimal duct.
Materials and methods
The test subject (author P.P) had no known lacrimal drainage problems. The examination was made with dynamic imaging using a Siemens Symbia T2 gamma camera (Erlangen, Germany). The gamma camera was equipped with a low energy collimator, utilizing a 15% gamma energy window and a zoom factor of 2.7-3.2. The test subject lay on his back with two pillows underneath his head. A drop of (approximately 150 kBq in 20 µL) of technetium-99m pertechnetate was placed into the middle of the inferior fornix of both eyes. Subsequently, the test subject turned over onto his right side and positioned his face directly to the right hand side for ten minutes. The eyes were open, blinking spontaneously. The first imaging was completed at 5-10 minutes post administration (Figure 2). However, after re-positioning the test subject into an upright position for a period of 5 minutes, the imaging was repeated in supine face-up position at intervals of 15-20 minutes and again at 25-30 minutes post administration (Figure 2).
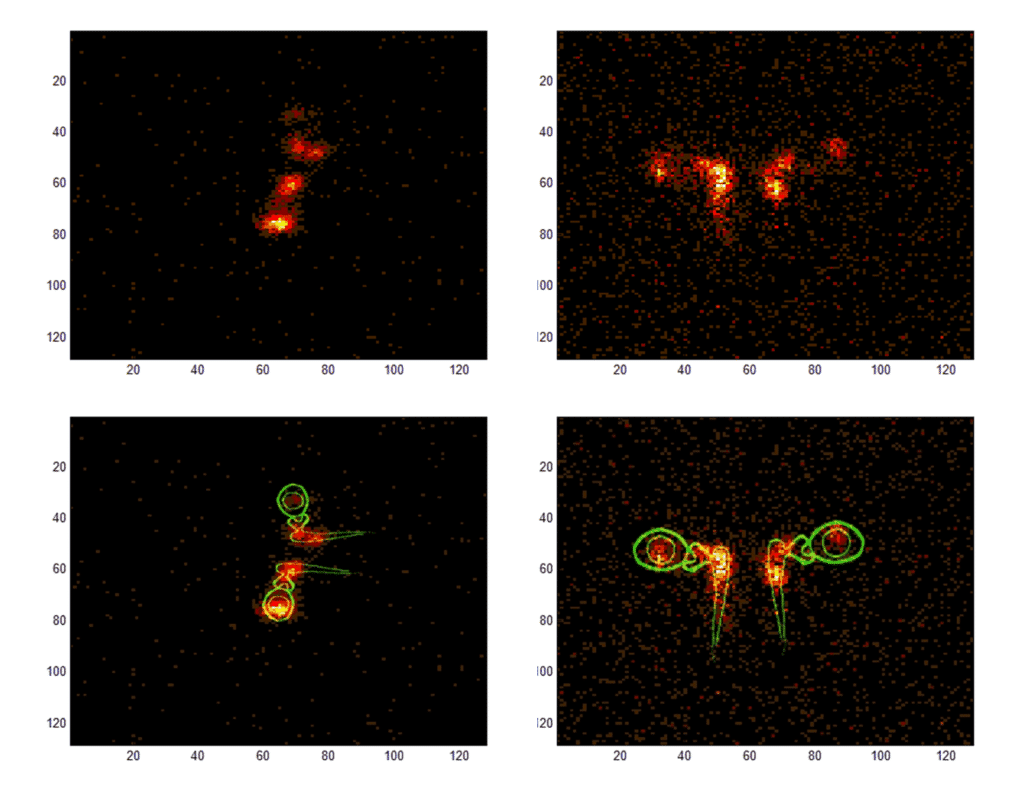
Figure 2. Lacrimal scintigraphy, the supine side position of the face, 5-10 minutes p.adm. right side down (left upper panel, actual image; left lower panel, actual image fused with lacrimal system scheme). In the right eye, the major activity is located laterally in the palpebral aperture, whereas the minor activity is soaked into the lacrimal canaliculi. In the left eye the majority of the tracer has transferred to the nasolacrimal passage. Lacrimal scintigraphy, supine face-up, 25-30 minutes p.adm. (right upper panel, actual image; right lower panel, actual image fused with lacrimal system scheme). The tracer has advanced towards the lower nasolacrimal passage symmetrically on both sides.
Results and discussion
During the side-down position of the eye, the majority of the tracer moved laterally, but did not exceed the temporal canthus. Some of the amount was soaked into the lacrimal canaliculi, presumably immediately after administration. The transfer further to the nasolacrimal passage occurred only after the down position was finished (Figure 3). It appeared that lacrimal scintigraphy can be performed in the supine position. The side-down position of the eye apparently prolongs the ocular contact time of a topical drop. The current recommendation to reduce the transfer of an eye drop into the lacrimal drainage system is to press the lacrimal sac with a finger or alternatively close the eye for 5 minutes after administering the drug. This improves the intraocular penetration of topically applied glaucoma medications and discourages systemic absorption [4]. Subsequently, the usage of gravitation combined with medication, offers an effective and convenient method alternative, compared to the current practice.
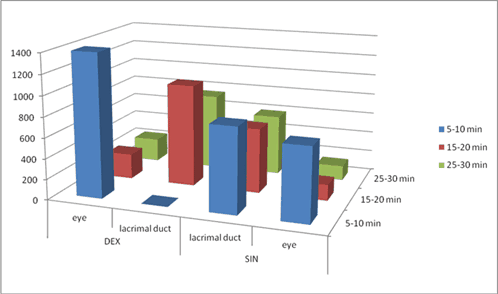
Figure 3. Quantitative results in the eyes and lacrimal ducts at different imaging intervals. At 5-10 min (face right) when there is no activity in the right lacrimal duct, although there is a lot of activity in the left lacrimal duct. At 15-20 min after 5 min of an upright position, in the face-up imaging position, the activity has disappeared from the right eye to the lacrimal duct; on the left the change is smaller. At 25-30 min, the situation is almost symmetrical in both eyes.
Conclusion
The supine side-down eye position inhibits the flow of an eye drop to the nasolacrimal passage. This may have an effect on pharmacodynamics and bioavailability of topically administered ophthalmic drugs.
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest (such as honoraria; educational grants; participation in speakers’ bureaus; membership, employment, consultancies, stock ownership, or other equity interest and expert testimony or patent-licensing arrangements), or non-financial interest (such as personal or professional relationships, affiliations, knowledge or beliefs) in the subject matter or materials discussed in this manuscript.
References
- Pohjanpelto P, Vorne M, Vähätalo S, Unto E. Gamma imaging of the lacrimal apparatus. Duodecim. 1980; 96: 1015-1020.PubMed
- MacDonald A, Burrell S. Infrequently performed studies in nuclear medicine. Part 1. J Nucl Med Technol. 2008; 36: 132-143.CrossRef PubMed
- Detorakis ET, Zissimopoulos A, Ionnakis K, Kozobolis VP. Lacrimal outflow mechanisms and the role of scintigraphy; current trends. World J Nucl Med. 2014; 13: 16-21.CrossRef PubMed
- Flach AJ. The importance of eyelid closure and nasolacrimal occlusion following the ocular instillation of topical glaucoma medications, and the need for the universal inclusion of one of these techniques in all patient treatments and clinical studies. Trans Am Ophthalmol Soc. 2008; 106: 138-148.PubMed
Article information
Corresponding Author: Kalevi Kairemo.
Copyright: © 2016 Pohjanpelto P et al.
How to cite: Pohjanpelto P, Kangasmäki A, Kairemo K. Lacrimal scintigraphy in the supine lateral head position. J. Diagn. Imaging Ther. 2016; 3(1): 52-54 (https://dx.doi.org/10.17229/jdit.2016-0905-023).
Article history: Received 01 September 2016; Revised 02 September 2016; Accepted 03 September 2016; Published online 05 September 2016.
Archive link: JDIT-2016-0903-023
home »
