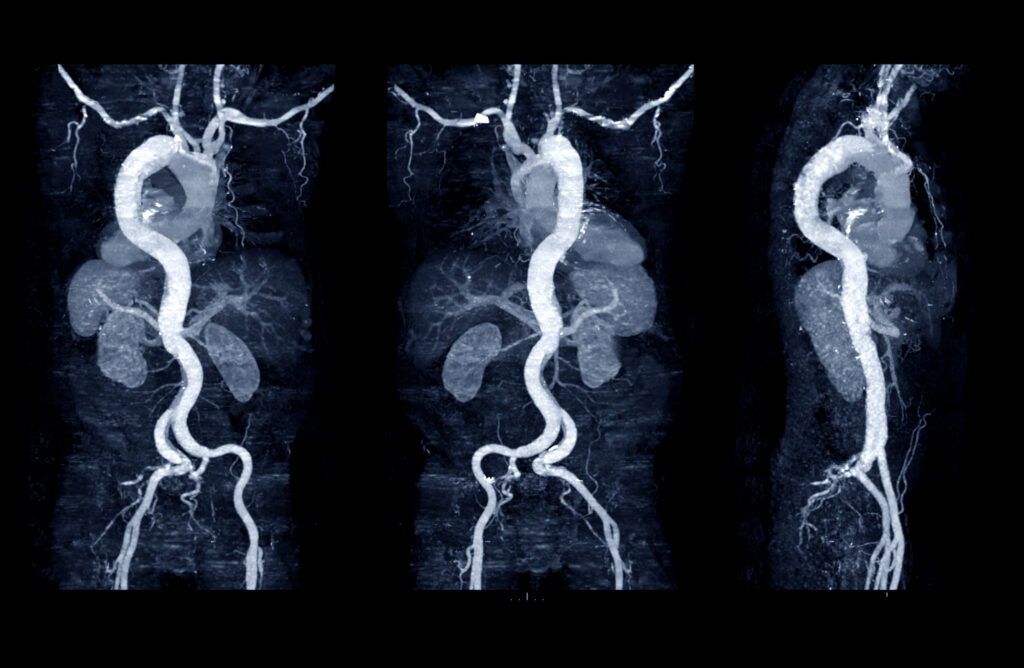
Keynote: Perivascular fat density measured on CTA is independently associated with abdominal aortic aneurysm progression and may serve as a practical imaging biomarker for risk stratification and monitoring.
Keywords: Perivascular fat density, abdominal aortic aneurysm, CTA aneurysm progression, fat density CTA, aneurysm imaging biomarker, aortic aneurysm growth.
Recent research has highlighted the potential of perivascular fat density (PFD) as a non-invasive imaging marker for predicting the progression of abdominal aortic aneurysms (AAAs). A retrospective analysis involving 144 patients with known AAAs demonstrated that higher PFD values on computed tomography angiography (CTA) were significantly associated with more rapid aneurysm growth.
The study compared baseline PFD values between patients with fast-growing and slow-growing aneurysms. Those in the fast-expanding group showed notably higher fat density measurements (–72.6 Hounsfield Units [HU]) compared to the slower-growth group (–81.2 HU), with a highly significant p-value of <0.001. These findings suggest that the characteristics of perivascular tissue, particularly inflammation as reflected by fat density, may play a crucial role in aneurysm dynamics.
PFD was also found to correlate positively with baseline AAA diameter, aneurysm volume, and the rate of annual expansion. Importantly, even after adjusting for various clinical factors and imaging characteristics, PFD remained independently associated with aneurysm progression. The reported odds ratio was 1.18 (95% confidence interval: 1.08–1.28; p<0.001), indicating a strong and consistent relationship.
This study supports the concept that CTA fat biomarkers, such as PFD, could be valuable in routine AAA follow-up. Given the widespread availability of CTA in clinical practice, this approach offers a practical advantage over other imaging modalities, such as PET or MRI, which are less accessible and more costly.
The implications are significant: identifying patients with elevated PFD could help stratify risk and tailor surveillance strategies more effectively. Furthermore, it opens avenues for monitoring the response to therapies targeting perivascular inflammation, which may influence aneurysm stability.
The research, published in BMC Medical Imaging by Zhang et al. (2025), contributes to the growing evidence that the perivascular environment is not merely a passive bystander in vascular disease, but may actively influence the biological processes driving aneurysm development and expansion.
As efforts continue to improve the prediction and management of AAA progression, perivascular fat density, measured via standard CTA, represents a promising and accessible imaging biomarker for risk stratification and longitudinal monitoring.
Reference: Zhang, S., Chang, N., Yu, X. et al. Association between perivascular fat density on CT angiography and abdominal aortic aneurysm progression. BMC Med Imaging 25, 357 (2025). https://doi.org/10.1186/s12880-025-01895-8
Disclaimer
This note summarises findings from a published research article for informational and educational purposes only. It is not intended to replace clinical judgement, diagnostic procedures, or professional medical advice. The content is based on the study by Zhang et al., published in BMC Medical Imaging (2025), and does not necessarily reflect the views of the original authors, journal, or affiliated institutions. Clinicians and researchers should refer to the full article for detailed methodology and interpretation before applying the findings in clinical practice or further research.