Quick Answer
An expert Canadian compounding pharmacy maintains compliance and quality in customised medications by adhering to NAPRA model standards, provincial regulations, and Health Canada requirements. This model involves multi-step verification processes, pharmaceutical-grade ingredients, accredited facilities for sterile and non-sterile preparations, rigorous pharmacist checks, and ongoing quality assurance programs that prioritise patient safety and precise formulation outcomes for their healthcare partners.
Introduction
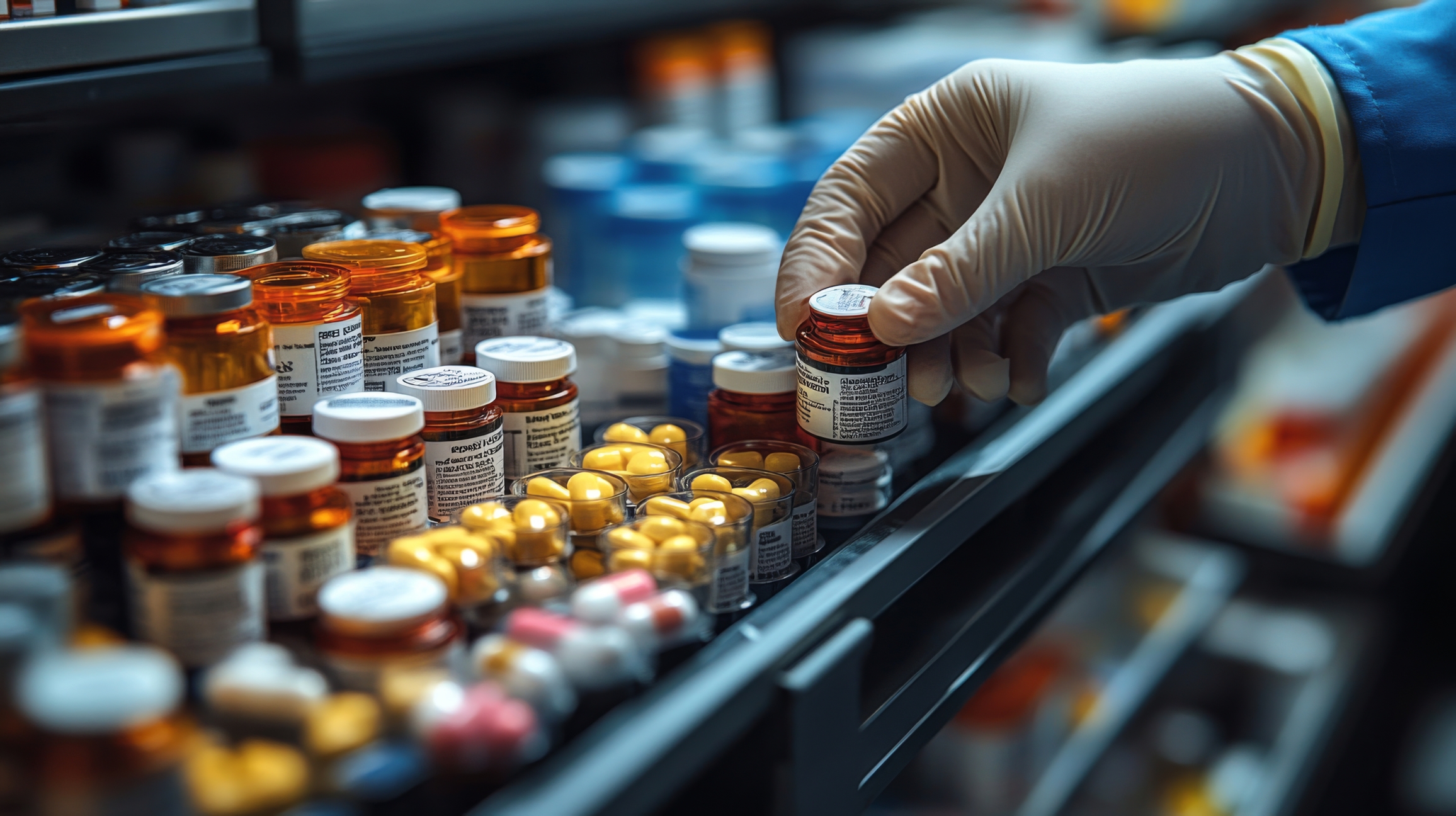
Healthcare providers often face challenges when standard commercial medications fail to meet specific patient needs, whether due to dosage adjustments, allergen concerns, or unique delivery methods. In these situations, turning to a compounding pharmacy becomes essential for creating tailored solutions that align with individual requirements while upholding the highest safety and efficacy standards.
Create Compounding exemplifies this commitment through structured processes, including multi-step pharmacist verifications, use of validated procedures, and sourcing from pharmacopeial-grade suppliers. Such practices build partners’ confidence by consistently delivering reliable, high-quality, customised medications that support effective patient care across diverse clinical scenarios.
Regulatory Frameworks for Compounding Pharmacy
National guidelines establish the foundation for all professional activities in this specialised field. These layered requirements combine federal direction with provincial enforcement to deliver consistent protections for every customised preparation.
Alignment with NAPRA Model Standards
NAPRA model standards define precise expectations for compounding environments, process validation, and risk management approaches. Compounding pharmacies integrate these expectations through structured policies that govern facility design, equipment maintenance, and staff qualifications. In practice, regular internal audits confirm ongoing adherence and identify opportunities for refinement before external reviews occur.
Provincial Licensing and Operational Mandates
Provincial colleges of pharmacists issue licenses and perform periodic audits focused on personnel credentials, documentation accuracy, and safety protocols. The result is a unified national system where only fully qualified operations handle specialised formulations.
- Verification of each prescription for clinical appropriateness and regulatory fit
- Sourcing exclusively from suppliers meeting pharmaceutical grade specifications
- Implementation of batch-specific testing for potency and sterility, where required
- Retention of full records to support traceability during any regulatory inquiry
Integration of Health Canada Directives
Health Canada supplements these frameworks with directives on ingredient traceability and product stability evaluation. Such requirements ensure that all materials and finished items meet stringent safety thresholds. This structured oversight directly supports reliable outcomes when standard commercial options fall short.
Implementing Quality Assurance in Customised Medications
Quality assurance forms the practical backbone of every preparation in a compounding pharmacy. This structured approach transforms regulatory requirements into daily operational realities through repeated checks, validated techniques, and controlled environments that minimise variability and maximise precision.
Core Elements of Multi-Step Verification
Every prescription undergoes a thorough review before compounding begins. Pharmacists assess clinical appropriateness, dosage calculations, potential interactions, and alignment with the original prescriber’s intent. Once formulation proceeds, preparation takes place in designated areas to maintain cleanliness and containment standards.
In accredited facilities, both sterile and non-sterile processes follow validated protocols. Ingredients arrive from suppliers adhering to pharmacopeial specifications, undergo identity confirmation upon receipt, and enter production only after clearance. During compounding, weights and measures are subject to double verification to prevent transcription errors.
Rigorous Quality Controls and Testing Protocols
Beyond initial checks, finished preparations face additional scrutiny. Labelling undergoes independent review for accuracy of instructions, strength, and beyond-use dating. For certain high-risk formulations, stability considerations or potency testing apply according to established guidelines.
A typical quality assurance sequence includes these key steps:
- Initial prescription evaluation by a licensed pharmacist
- Ingredient identity and quality confirmation
- Precise measurement and mixing using calibrated equipment
- Four separate pharmacist verifications covering formulation, preparation, labelling, and documentation
- Final release authorisation only after all checkpoints are clear
Comparison of Sterile vs Non-Sterile Quality Requirements
These layered controls create confidence that each customised medication meets exact specifications while protecting patient safety.
Sustaining Long-Term Compliance and Partner Confidence
Ongoing adherence to evolving standards separates reliable operations from those facing repeated corrective actions. In practice, pharmacies maintain momentum through proactive systems that anticipate regulatory shifts, preserve documentation integrity, and foster transparent communication with prescribers and healthcare teams.
Continuous Training and Competency Maintenance
Personnel involved in compounding receive regular education on updated NAPRA guidance, provincial bylaws, and emerging best practices in formulation science. Annual competency evaluations, combined with scenario-based simulations, confirm that staff retain technical proficiency across both routine and complex preparations.
The result is a workforce equipped to handle variations in prescription complexity while consistently applying current protocols. This sustained focus reduces the risk of deviation and reinforces trust when partners review audit trails or request process details.
Documentation and Traceability Systems
Full traceability remains non-negotiable for long-term viability. Every step, from ingredient receipt through final dispensing, is documented with timestamps in secure electronic systems. Batch records include supplier certificates, equipment calibration data, environmental monitoring logs, and all verification signatures. When questions arise months later, these records provide clear, defensible evidence of compliance.
Key traceability components include:
- Ingredient lot numbers cross-referenced with certificates of analysis
- Preparation logs capturing exact weights, mixing sequences, and environmental conditions
- Pharmacist verification timestamps at multiple production stages
- Beyond-use date rationale supported by stability references or published data
- Adverse event reporting mechanisms integrated into the workflow
Regular quality summaries shared upon request, combined with open channels for feedback, strengthen these professional bonds without the pressure to promote. Over time, this reliability translates into sustained collaboration even as regulatory landscapes continue to evolve.
Maintaining Excellence in Compounding Pharmacy Partnerships
The combination of robust regulatory alignment, meticulous quality assurance processes, and sustained operational discipline creates the foundation for consistent performance in this specialised field. Pharmacies that prioritise ongoing training, comprehensive documentation, and transparent communication position themselves to adapt effectively as guidelines evolve and partner expectations grow.
In the end, healthcare providers benefit most when they collaborate with operations that demonstrate unwavering commitment to these principles. So, a Canadian compounding pharmacy focused on precision and accountability delivers customised medications that reliably meet clinical needs while upholding the highest standards of safety and quality over the long term.
Disclaimer
This article is intended for informational and educational purposes only and does not constitute medical, pharmaceutical, or regulatory advice. Readers should consult qualified healthcare professionals or relevant regulatory authorities for guidance on specific compounding pharmacy practices, compliance requirements, or patient care decisions. References to organisations, standards, or services are provided for general context and do not represent endorsements.