Key Takeaways
- Teething marks the emergence of primary teeth in infants and lasts until about three years of age.
- Modern paediatric dentistry uses digital technologies and AI to monitor tooth eruption and diagnose abnormalities accurately.
- AI systems can analyse dental images to predict eruption patterns and identify potential orthodontic problems early.
- Intraoral scanning provides detailed digital models, improving comfort and monitoring for young patients.
- Emerging advancements aim to personalise treatment plans and enhance telemedicine in paediatric dental care.
Teething is one of the earliest biological processes in oral development, marking the emergence of primary teeth through the gums during infancy and early childhood. Although this process has long been recognised as a normal stage of development, modern paediatric dentistry has begun to examine tooth eruption in much greater detail using digital technologies, artificial intelligence (AI), and advanced imaging systems. These developments are transforming how dentists monitor teething, diagnose abnormalities in eruption patterns, and plan early interventions that support long-term oral health.
Historically, the clinical management of teething relied primarily on visual examination and parental reports of symptoms such as gum irritation, drooling, or mild discomfort. While these observations remain useful, contemporary dental research now emphasises the importance of understanding the biological mechanisms that regulate tooth eruption and identifying abnormalities before they cause complications. Medical imaging and digital diagnostic tools have therefore become central components of modern paediatric dental practice.
This article examines recent developments in the scientific understanding of teething in children and explores how medical imaging technologies are helping clinicians monitor tooth development more accurately and intervene earlier when problems occur.
Understanding the Biology of Tooth Eruption
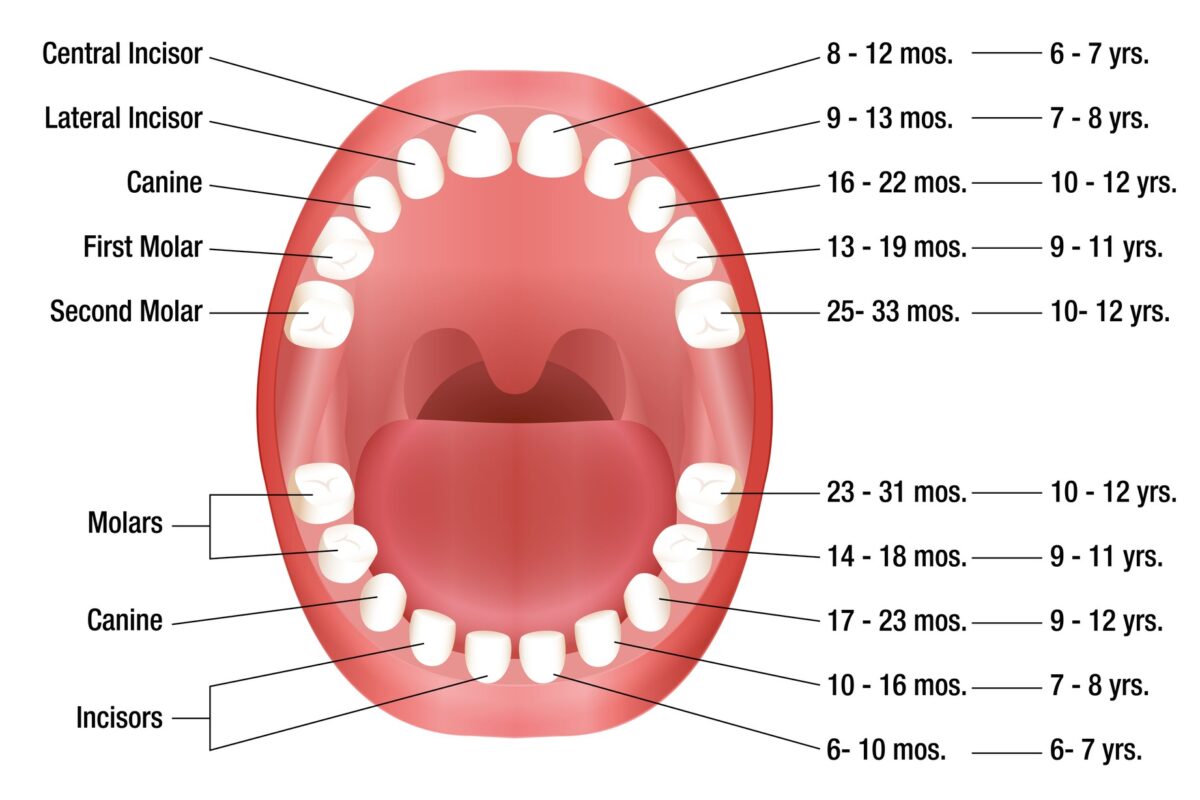
Teething refers to the eruption of primary teeth from the jawbone through the gum tissue into the oral cavity. This process typically begins at around six months of age and continues until approximately three years, when most children have a full set of twenty primary teeth. The eruption sequence usually follows a predictable pattern, starting with the lower central incisors and progressing towards the molars.
Although the process is natural, variations in eruption timing and sequence are common. Genetic factors, nutritional status, systemic diseases, and environmental influences may all affect tooth development. In some children, teeth may erupt earlier or later than expected, while others may develop conditions such as delayed eruption, ectopic eruption (when a tooth emerges in an abnormal position), or impacted teeth that remain trapped in the jawbone.
Understanding these variations is important because abnormalities in early tooth development can influence jaw growth, bite alignment, and the positioning of permanent teeth. Researchers, therefore, increasingly focus on monitoring tooth development from infancy through childhood to detect deviations from normal patterns.
Advances in paediatric dental research have also clarified that many symptoms traditionally attributed to teething, such as fever or severe illness, are not directly caused by the eruption process. Instead, teething is usually associated with localised gum discomfort, increased drooling, and mild irritability. This improved understanding has helped clinicians guide parents more accurately while emphasising the importance of dental monitoring during early childhood.
The Shift Towards Digital Dentistry
One of the most significant developments in modern dentistry is the transition from analogue diagnostic methods to digital technologies. Digital dentistry integrates computer-based imaging, three-dimensional modelling, and artificial intelligence to improve the detection and management of oral diseases.
In paediatric dentistry, these technologies provide valuable insights into the complex process of tooth eruption. Digital imaging allows clinicians to visualise developing teeth within the jawbone, enabling them to identify problems long before they become clinically visible.
A key advantage of digital systems is their ability to store and analyse large amounts of data. Radiographs, intraoral photographs, and three-dimensional scans can be compared over time, enabling dentists to track developmental changes with greater precision. This longitudinal monitoring is particularly useful during the mixed dentition period, when both primary and permanent teeth are present.
Artificial intelligence is also becoming an increasingly important component of digital dentistry. Machine learning algorithms can analyse dental images, identify anatomical structures, and automatically detect potential abnormalities. In paediatric dentistry, AI models have shown strong potential to improve diagnostic accuracy and support clinical decision-making.
These systems can analyse radiographic images, clinical photographs, and patient data simultaneously, enabling clinicians to detect dental conditions earlier and develop more personalised treatment strategies.
Artificial Intelligence and Tooth Eruption Analysis
Recent research has demonstrated how AI can analyse dental images to identify abnormalities associated with tooth eruption. Deep learning models trained on large datasets of panoramic radiographs can automatically detect individual teeth, classify them as primary or permanent, and determine their stage of development.
One study developed an AI-based system capable of detecting and segmenting teeth in paediatric panoramic radiographs with near-expert accuracy. The model achieved very high precision in identifying permanent and deciduous teeth during the mixed dentition stage, demonstrating its potential for clinical application.
Another line of research focuses specifically on predicting abnormal eruption patterns. Deep-learning systems have been developed to analyse radiographic images and detect ectopic eruption of permanent teeth, a condition that can disrupt normal dental alignment. These models can evaluate tooth position and development and classify eruption patterns with accuracy comparable to that of experienced dentists.
AI is also used to forecast tooth eruption sequences and identify children who may develop future orthodontic problems. By analysing large datasets of dental images, predictive algorithms can estimate the probability of malocclusion, crowding, or delayed eruption. This information allows clinicians to initiate preventive or interceptive treatments at an earlier stage.
Although these technologies are still undergoing validation in clinical environments, they represent an important step towards predictive dentistry, where potential problems are identified before they cause functional or structural damage.
Intraoral Scanning and Digital Models
Another recent innovation in paediatric dentistry is the use of intraoral scanners to create highly detailed digital models of the teeth and oral tissues. These devices capture thousands of images within seconds and combine them to produce a three-dimensional representation of the mouth.
Recent research has demonstrated how handheld intraoral scanners combined with AI-assisted software can generate comprehensive digital models of children’s teeth, enabling dentists to detect early signs of dental decay and developmental defects.
Intraoral scanning offers several advantages for paediatric patients. The process is quick, non-invasive, and comfortable, which is particularly important for young children who may find traditional dental impressions uncomfortable. Digital models can also be stored electronically and compared over time, allowing dentists to monitor changes in tooth position and eruption patterns.
These digital records are especially useful for orthodontic assessment. By analysing the spatial relationships between teeth and jaws, clinicians can determine whether early orthodontic intervention is necessary. In many cases, early detection of alignment problems allows for simpler treatments that guide the natural development of the dentition.
In addition, digital models can be shared remotely with specialists, making teledentistry and collaborative diagnosis more accessible.
Conventional Dental Radiography
Although newer technologies are emerging, conventional dental radiography remains one of the most widely used imaging techniques in paediatric dentistry. Digital radiographs allow clinicians to visualise the internal structures of teeth and jaws with relatively low radiation exposure.
Panoramic radiographs are particularly valuable for monitoring tooth eruption. These images capture the entire dental arch in a single view, revealing the position and developmental stage of both primary and permanent teeth. Sequential radiographs taken over time enable dentists to observe the progression of eruption and identify abnormalities such as impacted or supernumerary teeth.
Radiographic imaging is also useful for detecting dental caries, cysts, infections, and bone abnormalities that may interfere with tooth development. By identifying these conditions early, dentists can implement preventive treatments that minimise the need for more complex procedures later in life.
Digital radiography has further improved patient safety by reducing radiation doses and enabling electronic image enhancement for improved diagnostic clarity.
Cone Beam Computed Tomography in Paediatric Dentistry
Cone Beam Computed Tomography (CBCT) represents one of the most important advances in dental imaging. Unlike traditional radiographs, which produce two-dimensional images, CBCT generates three-dimensional representations of the teeth, jaws, and surrounding anatomical structures.
This technology provides a highly detailed visualisation of tooth roots, bone structures, and developing teeth within the jaw. CBCT is particularly useful for evaluating complex dental conditions, such as impacted teeth, cysts, and developmental anomalies, that cannot be fully assessed with conventional radiography.
Clinical studies have shown that CBCT can provide more accurate information about periodontal defects and bone structures than conventional intraoral imaging techniques.
In paediatric dentistry, CBCT is typically reserved for cases requiring detailed anatomical information for diagnosis or treatment planning. Examples include assessing impacted canines, evaluating jaw growth abnormalities, or planning surgical procedures.
Although CBCT involves higher radiation exposure than standard dental radiographs, modern systems employ low-dose protocols designed specifically for paediatric patients. These protocols ensure that the diagnostic benefits of three-dimensional imaging outweigh potential risks.
Multimodal Imaging and Data Integration
One of the most promising areas of research in dental imaging involves combining multiple imaging modalities to create more comprehensive diagnostic models. For example, CBCT data can be integrated with intraoral scans to produce detailed digital representations that include both internal anatomical structures and external tooth surfaces.
Advanced machine learning systems can analyse these combined datasets to identify subtle changes in tooth development and jaw growth. By integrating radiographic data with clinical records and imaging scans, these systems provide clinicians with a more complete understanding of each patient’s oral development.
Such multimodal approaches are also enabling researchers to build large datasets of paediatric dental images. These datasets are essential for training AI systems to detect abnormalities in tooth eruption and predict future dental problems.
Early Detection and Preventive Dentistry
The integration of imaging technologies and artificial intelligence is transforming paediatric dentistry from a reactive to a preventive discipline. Instead of waiting until symptoms appear, clinicians can now detect potential problems much earlier.
Early identification of eruption disturbances allows dentists to intervene before permanent teeth become misaligned. For example, interceptive orthodontics can guide the eruption path of developing teeth and prevent crowding or bite abnormalities.
Imaging also helps dentists monitor jaw growth and facial development. Because tooth alignment is closely related to skeletal development, early detection of growth abnormalities can inform treatment strategies that support normal development.
These advances ultimately contribute to improved long-term oral health outcomes for children.
Future Directions in Dental Imaging for Teething
The next decade is likely to see continued integration of digital technologies in paediatric dentistry. Several emerging developments are particularly promising.
First, artificial intelligence systems will become more accurate as larger datasets of paediatric dental images become available. Improved algorithms may eventually provide real-time diagnostic support during dental examinations.
Second, advances in imaging technology may further reduce radiation exposure. Researchers are exploring alternative imaging methods such as optical coherence tomography and ultrasound, which may provide detailed images of dental tissues without ionising radiation.
Third, digital dentistry will increasingly incorporate personalised treatment planning. By combining genetic information, imaging data, and predictive modelling, clinicians may be able to forecast dental development and tailor interventions to individual patients.
Finally, telemedicine and remote diagnostics are expected to play a larger role in paediatric dental care. Digital scans and imaging data can be shared with specialists across different locations, expanding access to expert consultation.
Conclusion
Recent advances in paediatric dentistry have significantly improved the understanding of teething and tooth eruption in children. While teething is a natural stage of development, modern research has revealed that variations in eruption patterns can influence long-term oral health.
Medical imaging technologies, including digital radiography, cone beam computed tomography, and intraoral scanning, allow dentists to visualise teeth and jaw structures with unprecedented detail. When combined with artificial intelligence and digital data analysis, these tools enable clinicians to detect abnormalities earlier, monitor dental development more accurately, and plan preventive treatments that support healthy oral growth.
As digital technologies continue to evolve, the integration of advanced imaging and predictive analytics will likely further transform paediatric dentistry. Early diagnosis, personalised treatment planning, and minimally invasive interventions will become increasingly central to the management of teething and tooth development in children.
Ultimately, these developments represent an important step towards a more proactive and technologically advanced approach to oral healthcare for young patients.
Disclaimer
The information presented in this article is intended for general educational and informational purposes only. It does not constitute professional medical or dental advice, diagnosis, or treatment. The content reflects current research and developments in paediatric dentistry and medical imaging, but should not be used as a substitute for consultation with qualified healthcare professionals.
Parents, caregivers, and readers should always seek advice from a licensed dentist, paediatric dentist, or healthcare provider regarding any questions or concerns about a child’s oral health, teething symptoms, or dental development. Individual cases may vary, and appropriate diagnosis and treatment require clinical evaluation by trained professionals.
Open MedScience makes no representations or warranties regarding the completeness, accuracy, or reliability of the information provided. The publication of this article does not imply endorsement of any specific medical procedure, technology, or treatment discussed.
home » blog » dentistry »