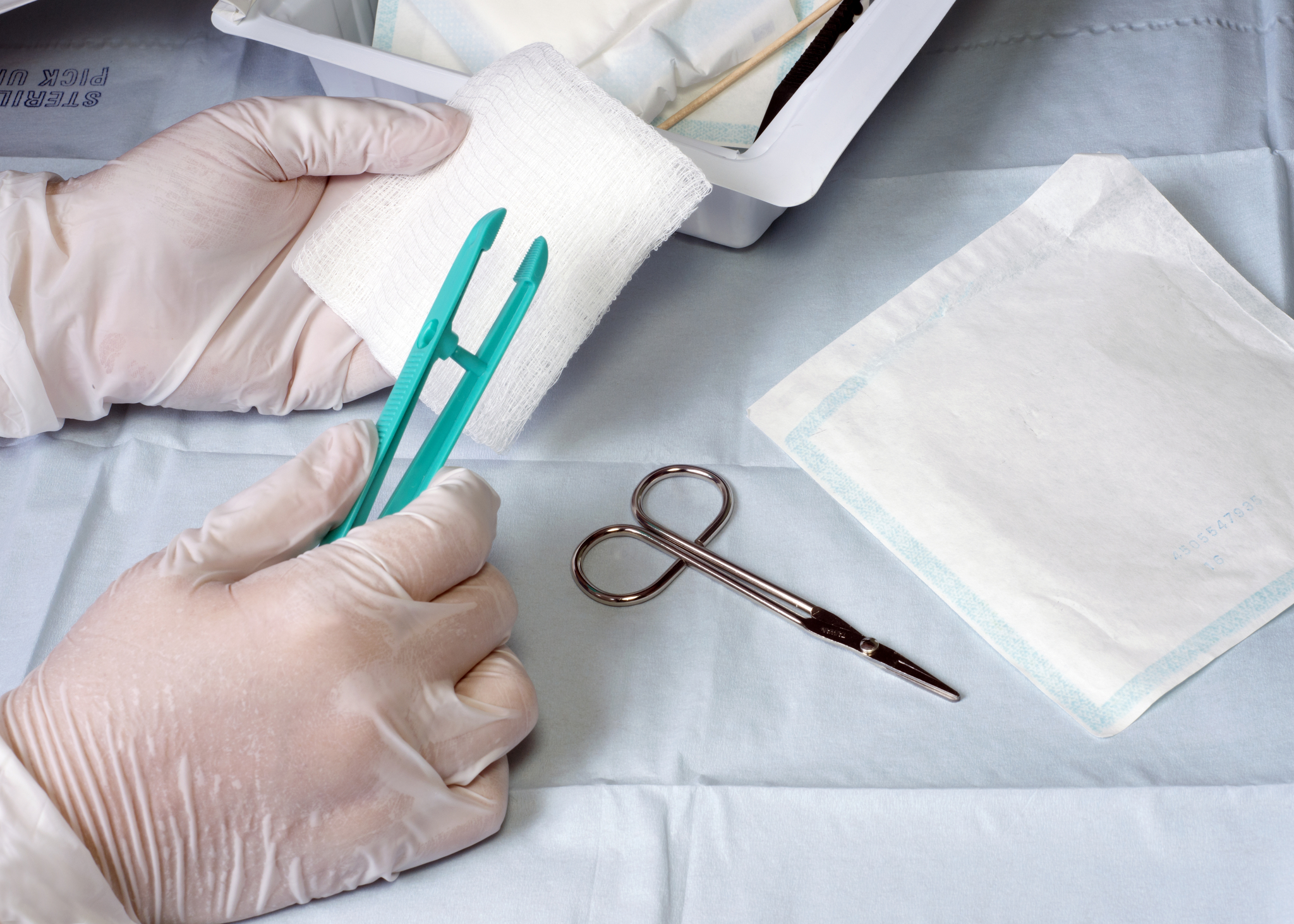
If you care for patients with diabetic foot ulcers, pressure injuries, or slow-healing surgical sites, you’ve likely wondered, “I know the basics, but am I using the most current approach?” That’s a fair question. Wound care now spans infection control, pain management, and long-term quality of life, not just dressings and bandages.
Modern wound care certification programs help you turn daily experience into structured skills. You learn assessment, debridement decisions, dressing selection, and documentation. Hospitals, home health agencies, and long-term care settings are seeing more complex wounds as patients age and acuity rises. Employers want proof that you can handle those cases safely and with confidence. Formal wound care training offers that proof.
This guide shows you exactly what these programs teach. By the end, you’ll know whether certification will give you the clarity, confidence, and clinical skill set you’re looking for.
Why Structured Wound Care Education Matters Now
Across hospitals, long-term care, and home health, clinicians are seeing more complex wounds as diabetes, chronic vascular disease, and population ageing all rise together. These patients often have multiple comorbidities, limited mobility, and fragile skin, which makes them far more vulnerable to pressure injuries, surgical site complications, and slow-healing ulcers.
Structured wound education replaces that variability with a shared language, a stepwise approach to assessment, and protocols that link daily practice to measurable outcomes. International pressure injury guidelines developed with the National Pressure Injury Advisory Panel (NPIAP) show that consistent risk scoring, repositioning, and moisture management can reduce both the incidence and severity of pressure injuries when teams follow a common protocol.
CDC infection-prevention guidance likewise highlights core practices such as hand hygiene, aseptic technique, and appropriate device management as baseline standards to reduce healthcare-associated infections across settings.
Core Skills Covered in Modern Courses
Modern wound care courses focus on practical skills that translate directly to the bedside. Instead of memorising staging labels or product names in isolation, learners work through short cases that show how each decision affects healing, comfort, infection risk, and length of stay. When you compare programs, look for a wound care certification that explains not only what to do, but also why specific choices matter in different care settings. A strong curriculum usually covers competencies such as:
- Accurate wound assessment and staging: using consistent measurement techniques, describing tissue types clearly, and spotting early infection or biofilm so treatment can be escalated before deterioration. International pressure injury guidance stresses standardised tools to support consistent decision-making across the team.
- Dressing selection and moisture balance: matching dressings and advanced options such as negative pressure therapy, contact layers, and compression to the wound’s depth, drainage, and aetiology. WOCN-linked guidelines highlight how appropriate dressings and change frequency support moist healing while protecting periwound skin.
- Safe debridement principles: clarifying which methods fall within the learner’s scope of practice, how to check perfusion and pain control, and when to refer promptly for surgical or specialist intervention.
- Infection-prevention and antimicrobial stewardship: reinforcing aseptic technique, appropriate specimen collection, and collaboration with infection-prevention and pharmacy teams to avoid unnecessary antimicrobial use. CDC core infection-prevention practices frame these behaviours as baseline expectations in all healthcare settings.
- Pain management, education, and communication: using non-pharmacologic strategies alongside timed analgesia, explaining dressing plans in plain language, and coordinating goals of care with nurses, therapists, dietitians, and prescribers so that patients understand and can follow the plan between visits.
How Modern Wound Care Training Fits Busy Clinical Schedules
For most clinicians, the barrier to further study is not motivation but time. Modern courses address this by offering modular, self-paced content that can be completed between shifts or during protected learning time. Typically, learners move through short video lessons, case discussions, quizzes, and skills checklists that reinforce concepts while tracking progress through structured wound care training.
Fully online courses have become the primary route for many clinicians because they combine flexibility with structure. In-person or blended programs, including workshops and simulation labs, remain useful for hands-on practice but are often limited by travel, tuition costs, and staffing constraints.
Building Confidence in Wound Care Practice
Structured wound education gives clinicians a clearer roadmap for assessing risk, staging wounds accurately, choosing appropriate dressings, and recognising when to escalate care. Over time, that shared knowledge base strengthens decision-making, supports safer documentation and infection-prevention practices, and makes it easier for teams to speak a common clinical language about complex wounds.
As you compare programs, take a close look at course syllabi, faculty experience, clinical guideline alignment, and accreditation status, and then get certified by reputed organisations that can demonstrate transparent standards and outcomes.
Disclaimer: This article is for informational and educational purposes only and does not constitute medical advice or professional guidance. Clinicians should follow local policies, professional standards, and consult qualified healthcare providers or specialists when making clinical decisions.
home » blog » education »