Blemishes are among the most common skin concerns presenting in both clinical and consumer settings. Yet despite their prevalence, the standard treatment approach remains largely unchanged: target the bacteria, strip the excess oil, dry out the visible lesion. For many people, this works in the short term. For just as many, it does not work at all, or creates new problems as fast as it clears the old ones.
Understanding why requires examining what blemishes actually are at the biological level and why effective treatment demands more than a single mechanism of action.
What Blemishes Are and How They Form
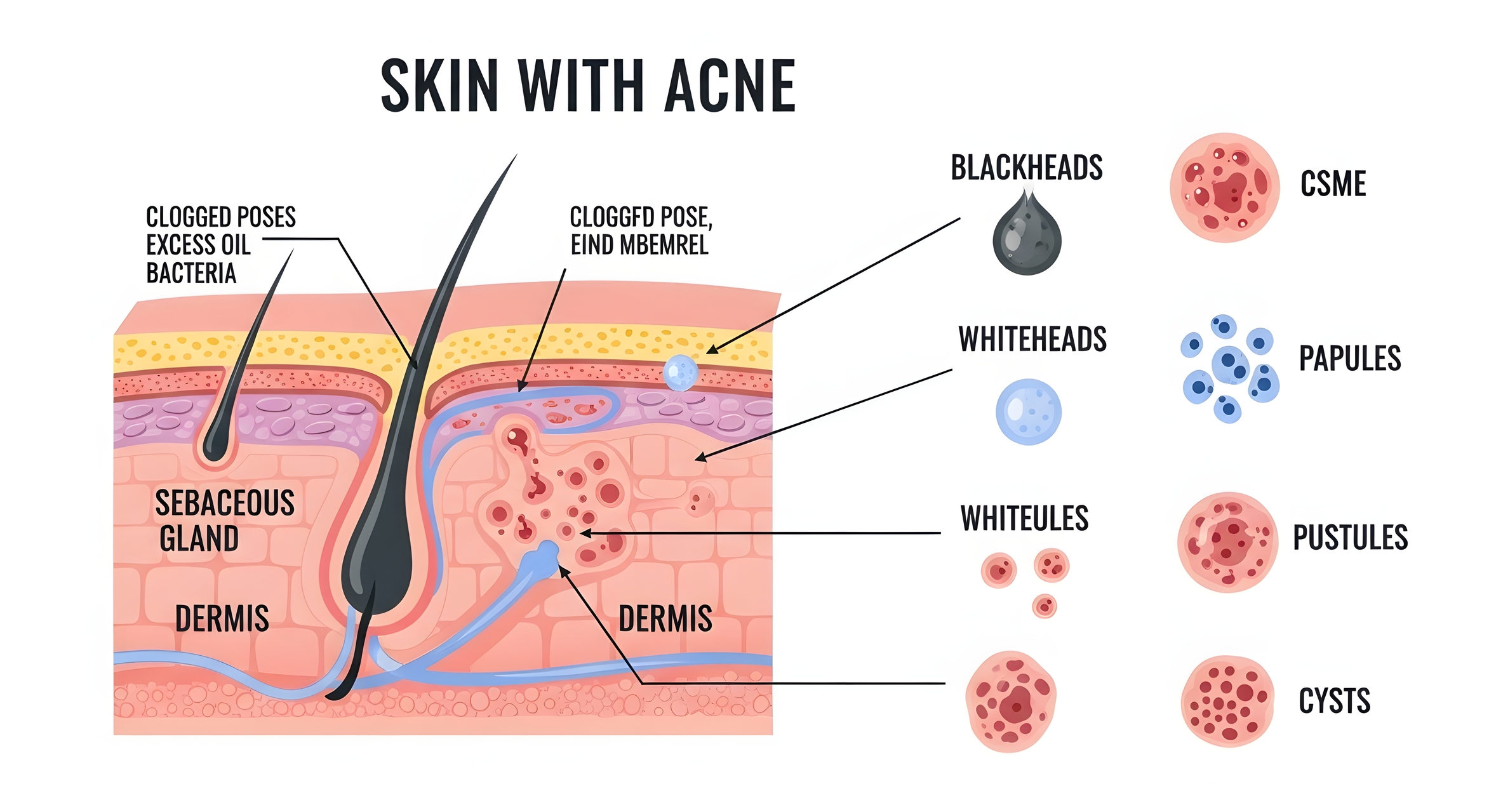
A blemish is a broad term for any visible skin imperfection, including comedonal lesions (whiteheads and blackheads), inflammatory lesions (papules and pustules), severe nodular or cystic lesions, and the post-inflammatory discolouration and scarring that follows. from mild surface-level congestion to deep, scar-forming cysts that require clinical intervention.
What they share is a common origin. Blemishes form when the pilosebaceous unit becomes dysfunctional. Dead skin cells accumulate at the follicle opening rather than shedding normally. Sebum produced by the sebaceous gland becomes trapped behind that blockage.
Cutibacterium acnes (formerly Propionibacterium acnes), a bacterium that colonises the hair follicle, proliferates in the anaerobic environment created by the plug. The immune system responds with inflammation. The result, depending on depth and severity, is everything from a surface whitehead to a painful cystic nodule.
The key point is that all four of these events occur simultaneously. Blocking, bacteria, sebum excess, and inflammation are not sequential steps. They are concurrent processes that reinforce each other, which is precisely why treating only one of them tends to produce incomplete results.
The Limitation of Single-Target Approaches
The dominant model for blemish treatment has been to identify the most visible driver and apply a chemical agent to suppress it. Benzoyl peroxide targets bacteria. Salicylic acid dissolves the keratin plug in the follicle opening. Retinoids accelerate cell turnover to prevent accumulation. Each has clinical evidence behind it. Each also has a well-documented limitation.
Benzoyl peroxide is bactericidal and effective against Cutibacterium acnes, but it is also a strong oxidising agent. At the concentrations used in most over-the-counter products (2.5-10%), it commonly causes dryness, peeling, and disruption of the skin barrier. When the skin barrier is compromised, transepidermal water loss increases, the skin becomes more reactive to environmental irritants, and the sebaceous glands frequently upregulate sebum production. The net result can be a cycle where treating one driver of blemishes exacerbates another.
Salicylic acid’s mechanism is better suited to comedonal blemishes than to inflamed lesions, as it works by dissolving the lipid plug rather than directly targeting bacteria or inflammation. It is a useful maintenance ingredient, but not a comprehensive treatment on its own.
Retinoids are effective at preventing follicular hyperkeratinisation but carry a well-known adjustment period of 4 to 8 weeks during which blemishes often worsen before improving. Research on sebum composition in acne patients has also highlighted that the quality of sebum matters as much as the quantity. In acne-prone skin, linoleic acid is consistently deficient, altering sebum consistency and promoting comedone formation. No current retinoid or salicylic acid treatment directly addresses this deficiency.
The pattern across conventional approaches is the same: they are well-engineered for one mechanism but leave the others unaddressed. That gap is where most people experience recurring or treatment-resistant blemishes.
What a Multi-Target Formulation Looks Like
A formulation that addresses all four drivers simultaneously needs antibacterial activity, anti-inflammatory compounds, barrier-supporting lipids, and exfoliating or pore-clearing agents. The challenge in conventional chemistry is that the most effective antibacterials tend to be the most damaging to the barrier. This is the tradeoff that makes single-formulation conventional blemish treatment difficult.
Botanical formulations offer a different chemistry. Many plant-derived compounds have overlapping activities. They can suppress bacterial growth and reduce inflammation with a single molecule, without the barrier-stripping properties of synthetic oxidising agents. This makes them particularly relevant for skin already damaged by years of conventional treatment.
Botanical Ingredients With Documented Skin Activity
Several botanical actives have now accumulated sufficient peer-reviewed evidence to be considered clinically relevant rather than merely traditional. The following represent the most studied in the context of inflammatory and comedonal blemishes.
Calendula officinalis (Marigold)
An updated review on the multifaceted therapeutic potential of Calendula officinalis confirms its anti-inflammatory, antibacterial, antioxidant, and wound-healing activities. The relevant mechanisms for blemish treatment include inhibition of pro-inflammatory cytokine production and direct antibacterial activity against Gram-positive bacteria. Norse Organics reports acne reduction of up to 78% over 90 days in formulations that use calendula as the primary active, based on their ingredient-level study data. Calendula is also notably well tolerated on reactive and sensitive skin, a significant advantage over synthetic antibacterials.
Sea buckthorn (Hippophae rhamnoides)
Sea buckthorn oil is unusual in containing over 190 bioactive compounds, including the rare omega-7 fatty acid, palmitoleic acid. This fatty acid is a natural component of human skin lipids and supports skin barrier function and wound healing. Sea buckthorn also contains beta-carotene, tocopherols (vitamin E), and phytosterols that collectively reduce oxidative stress and suppress inflammatory mediators. For blemish-prone skin, its primary value is barrier rebuilding and anti-inflammatory support, addressing two of the four drivers that conventional treatments typically ignore.
Thistle oil (Carthamus tinctorius)
Thistle oil is high in linoleic acid, the fatty acid consistently shown to be deficient in the sebum of acne-prone individuals. Topical application of linoleic acid-rich oils has been shown to reduce microcomedone size and improve sebum composition. In clinical testing, 92% of participants reported significantly more moisturised skin after two weeks of using thistle oil, without increased oiliness. This addresses the sebum quality problem directly rather than simply suppressing sebum quantity.
Borage oil (Borago officinalis)
Borage oil is the richest plant source of gamma-linolenic acid (GLA), an omega-6 fatty acid with established anti-inflammatory properties. GLA is a precursor to anti-inflammatory prostaglandins and suppresses the production of pro-inflammatory leukotrienes. In blemish-prone skin, topical borage oil supports barrier function, reduces inflammatory response, and penetrates more deeply than most surface-level treatments, making it particularly relevant for deep inflammatory and cystic blemishes where surface-only treatments have limited effect.
Rosehip (Rosa canina)
Rosehip oil’s relevance to blemish treatment extends beyond active breakouts to post-blemish recovery. It contains trans-retinoic acid precursors, linoleic acid, and a range of antioxidants that support cellular repair. Clinical evidence supports its role in reducing scar depth and post-inflammatory hyperpigmentation, meaning it addresses the marks that persist after a blemish heals. For people dealing with both active blemishes and residual discolouration, rosehip works on both the active and residual phases of the problem.
These ingredients work on different parts of the blemish cycle without creating the tradeoffs inherent in single-agent synthetic approaches. Brands that have built formulations around concentrated combinations of these actives are now accumulating substantial real-world evidence.
One example is Norse Organics, whose blemish treatment approach combines cold-pressed calendula, sea buckthorn, thistle, borage, and rosehip in a waterless formulation that delivers concentrated botanical actives without synthetic fillers or preservatives. Their customer data show 97% satisfaction among more than 500,000 users, with some individuals reporting a visible reduction in redness within the first 8 to 12 hours of use.
Practical Considerations for Blemish Treatment Selection
Whether evaluating a botanical or conventional approach, several principles apply when assessing likely efficacy.
- Mechanism coverage. Does the formulation address bacteria, sebum quality, pore congestion, and inflammation? Products targeting only one or two of these will produce incomplete results for most people.
- Barrier impact. Does the treatment support or compromise the skin barrier? Barrier damage drives rebound sebum production and increases vulnerability to bacterial colonisation, which perpetuates the blemish cycle.
- Ingredient concentration. Botanical actives must be present at therapeutically relevant concentrations. A trace quantity of calendula in an otherwise water-based formula will not produce the same outcomes as a concentrated, waterless botanical formulation.
- Post-blemish recovery. Effective treatment addresses the marks and discolouration that follow breakouts, not just the active lesions. A complete blemish treatment strategy includes ingredients that support scar fading and cellular renewal.
- Time commitment. Blemish treatment requires at least one complete skin cell turnover cycle (approximately 28 days) to produce meaningful results. Any evaluation period shorter than this does not give a treatment a genuine trial.
Summary
Blemishes are multi-factorial. They develop when bacteria, excess sebum, follicular congestion, and inflammation interact simultaneously. Treatments that address only one of these drivers can produce visible results in the short term but often leave the other drivers intact, which is why recurrence is so common.
The evidence increasingly supports formulations that target all four mechanisms concurrently. Whether that is through carefully designed botanical combinations or through a combination of conventional therapies, the principle is the same: blemish treatment that works over the long term needs to address the full biology of why blemishes form, not just the most visible symptom at any given moment.
For readers managing persistent blemishes, the most productive question to ask of any treatment is not whether it works on bacteria, but whether it addresses the entire cycle. The answer to that question narrows the field considerably.
Disclaimer
This content is for general informational purposes only and is not medical advice. It is not intended to replace consultation with a qualified healthcare professional. References to specific ingredients, products, brands, or reported results do not amount to endorsement or guarantee, and individual outcomes will vary. Readers should seek professional advice for persistent or severe skin concerns and use skincare products with care, including patch testing where appropriate.