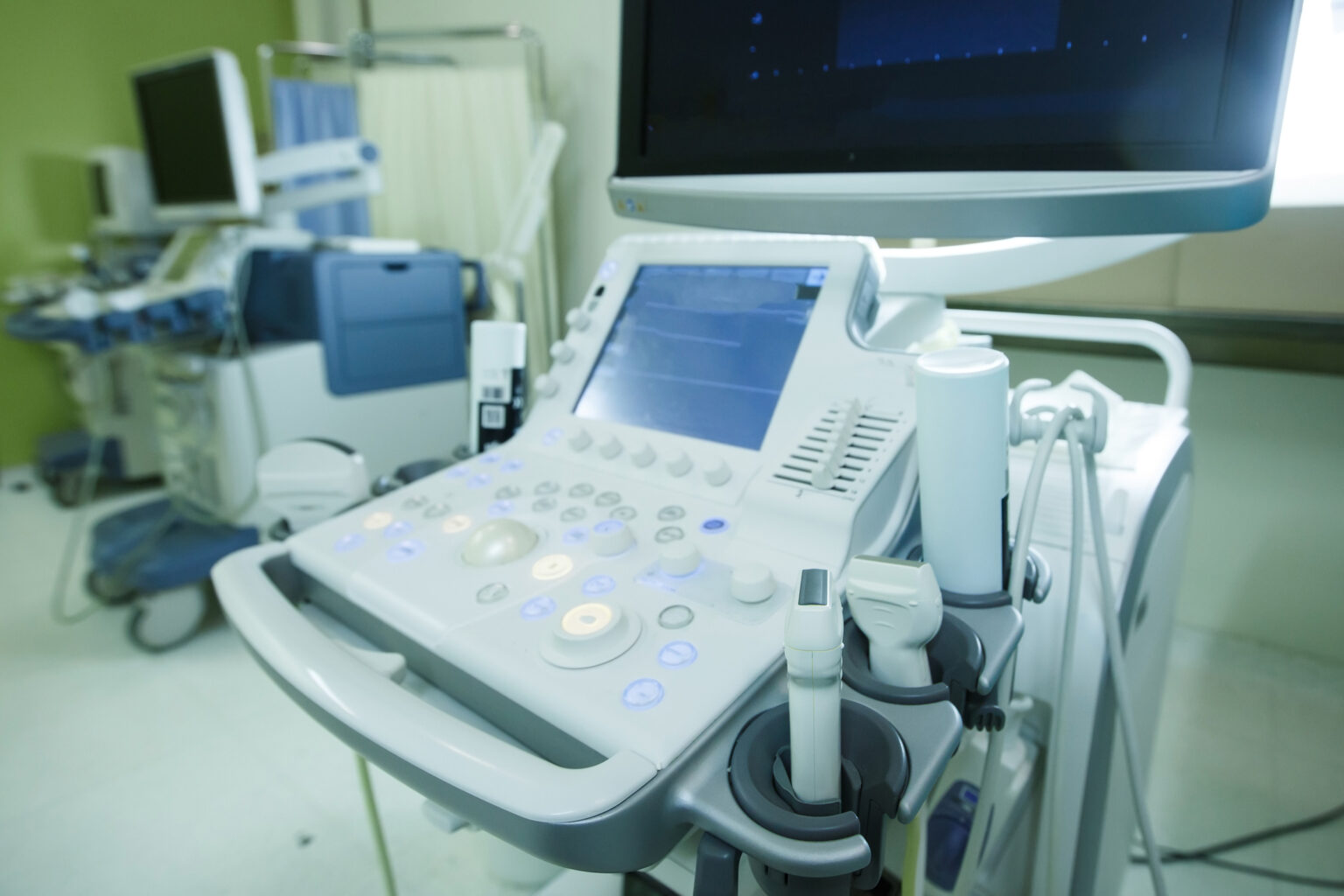
Ultrasound imaging has undergone remarkable progress in recent years. Once confined to static 2D scans and specialist radiology departments, it now spans emergency care, oncology, neurology, and even therapeutic interventions. The combination of artificial intelligence, hardware innovation, and miniaturised technology is reshaping what ultrasound can achieve in both clinical and research settings.
The latest advancements indicate a shift towards greater automation, portability, and diagnostic precision—changes that promise to transform the way clinicians, researchers and healthcare systems approach imaging.
Artificial Intelligence and Automation
The integration of artificial intelligence (AI) is one of the most significant developments in ultrasound imaging. Traditional ultrasound has always relied heavily on operator expertise. Image quality and diagnostic accuracy could vary depending on who performed the scan. Today, AI systems are reducing that variability by automating image capture, segmentation, and interpretation.
AI-assisted ultrasound platforms, such as Philips’s latest software for the EPIQ Elite and Affiniti systems, provide automated measurements and diagnostic guidance during examinations. These tools analyse the data in real time, flagging areas of concern and suggesting measurements based on pattern recognition and deep learning algorithms. The result is faster workflow, reduced cognitive load for clinicians, and more consistent imaging outcomes.
In breast ultrasound, deep learning algorithms are being trained to detect tumours and differentiate between benign and malignant lesions with high accuracy. Similarly, in obstetric imaging, AI models such as U-Net++ with attention mechanisms automatically segment the foetal anatomy, reducing the need for manual contouring.
These systems are particularly valuable in resource-limited environments where access to experienced sonographers is scarce. AI allows non-specialists to obtain clinically useful scans under guidance from real-time algorithms, broadening access to ultrasound diagnostics across diverse healthcare settings.
However, there are still challenges. AI models must be validated across different populations and equipment types to prevent bias. Clinical oversight remains essential, as the accuracy of AI interpretation can still depend on the quality of image acquisition. Nevertheless, as regulatory frameworks evolve, the integration of AI will continue to enhance ultrasound’s role as a rapid, intelligent, and accessible imaging tool.
Point-of-Care and Portable Ultrasound
The miniaturisation of ultrasound technology has arguably been as transformative as the introduction of AI. Portable and handheld devices are now capable of producing diagnostic-quality images and can connect wirelessly to tablets or smartphones. These systems—commonly referred to as point-of-care ultrasound (POCUS)—are expanding the reach of imaging beyond hospitals and radiology departments.
POCUS is being adopted in emergency medicine, intensive care, sports medicine, and even pre-hospital environments. Paramedics can now assess trauma or cardiac activity on scene, guiding treatment before hospital arrival. This capability not only saves time but also supports earlier decision-making in critical care.
Manufacturers such as Philips and GE Healthcare have developed advanced portable systems, including the Flash 5100 POC, designed specifically for high-acuity settings. These handheld scanners are battery-powered, durable, and capable of high-resolution imaging for cardiac, abdominal, and musculoskeletal assessment.
The potential impact of POCUS in low- and middle-income countries is particularly noteworthy. Portable ultrasound devices are relatively affordable, do not require radiation shielding, and can operate in remote settings with minimal infrastructure. Combined with AI-assisted scanning, they could help democratise access to medical imaging worldwide.
Yet, as with any decentralised technology, training remains a significant factor. While POCUS devices make ultrasound more accessible, they also highlight the need for consistent education and quality assurance frameworks to ensure reliable results across different operators and settings.
Beyond 2D: 3D, 4D and Fusion Imaging
Ultrasound has traditionally provided two-dimensional cross-sectional images, but recent developments in 3D and 4D ultrasound are changing that. Using tomographic reconstruction techniques, clinicians can now visualise organs and tissues in three dimensions, enhancing understanding of spatial relationships and improving diagnostic confidence.
The approval of PIUR Imaging’s tomographic ultrasound system for use with GE scanners represents a major step forward. It enables automated 3D reconstructions that can be manipulated in real time, allowing detailed evaluation of vascular and soft-tissue structures without ionising radiation.
Fusion imaging—a technique that overlays ultrasound data with MRI or CT images—is another growing trend. It combines the real-time capability of ultrasound with the anatomical detail of other modalities, creating a comprehensive view that aids navigation during biopsies or interventional procedures.
Quantitative imaging methods are also advancing. Elastography, for instance, measures tissue stiffness and provides valuable information for assessing fibrosis, tumours, or vascular compliance. Microvascular imaging and contrast-enhanced ultrasound (CEUS) can now visualise blood flow at the capillary level, revealing perfusion patterns previously only seen with advanced MRI.
These developments reflect a broader goal within imaging: to obtain not just structural information, but functional and quantitative data that can inform early diagnosis and personalised treatment planning.
Therapeutic and Interventional Ultrasound
While ultrasound is best known as a diagnostic tool, its therapeutic applications are expanding rapidly. High-intensity focused ultrasound (HIFU) and histotripsy are two of the most exciting examples.
Histotripsy, now under clinical trial within the NHS, uses focused ultrasound pulses to disrupt tumour tissue without heat or incisions mechanically. Early results suggest it can precisely destroy targeted cells while sparing surrounding tissue—a potential alternative to surgery or radiation for certain cancers.
Similarly, HIFU is already approved for conditions such as uterine fibroids and prostate disease. It delivers concentrated ultrasound energy to induce thermal coagulation, effectively treating tissue without invasive procedures.
Ultrasound is also being explored for drug delivery and neuromodulation. Focused ultrasound can transiently open the blood–brain barrier, allowing targeted delivery of therapeutic agents. This has significant implications for neurological disorders and oncology, where localised drug access has long been a challenge.
In hepatology, the emergence of ultrasound-derived fat fraction (UDFF) techniques allows quantitative assessment of liver steatosis. These measurements correlate closely with MRI-based methods, providing a non-invasive, cost-effective approach for monitoring metabolic and liver diseases.
The convergence of diagnostic and therapeutic ultrasound signals a broader shift towards image-guided, non-invasive medicine, where treatment can be visualised and adjusted in real time.
Hardware and Transducer Innovation
Modern ultrasound performance relies heavily on transducer technology, and this area is experiencing rapid innovation. High-frequency probes (above 20 MHz) are improving resolution for dermatological, ophthalmic, and vascular imaging, enabling visualisation of fine anatomical detail.
At the same time, research into flexible and wearable ultrasound transducers is advancing. Thin, lightweight patches using piezoelectric or polymer materials can adhere to the skin and continuously monitor organs such as the heart or bladder. These devices could transform patient monitoring in hospital wards or even at home.
Micro-electromechanical system (MEMS)-based arrays are another promising development. They allow smaller, cheaper, and more energy-efficient probes, making high-quality ultrasound feasible in portable formats.
On the software side, adaptive beamforming and advanced noise-reduction techniques are improving image clarity, while machine learning is optimising signal processing automatically during scanning.
Together, these hardware and software improvements are expanding the boundaries of ultrasound, making it more accurate, accessible, and adaptable to a wide range of clinical tasks.
Expanding Clinical Applications
The diversity of ultrasound’s applications continues to grow. Beyond obstetrics and cardiology, it now plays a central role in neuromuscular, vascular, hepatic, and oncological imaging.
In vascular medicine, quantitative ultrasound parameters are being used to assess arterial stiffness and vascular ageing, providing early indicators of cardiovascular risk. In neurology, deep learning models are helping automate the evaluation of muscle pathology in neuromuscular diseases, improving diagnostic consistency and speed.
In oncology, multiparametric ultrasound—combining elastography, CEUS, and 3D imaging—offers detailed tissue characterisation that may reduce the need for more invasive procedures.
Even in metabolic and public health contexts, ultrasound is gaining ground. Non-invasive liver screening using UDFF is emerging as a viable population-level tool for identifying fatty liver disease and tracking the effects of lifestyle or pharmacological interventions.
As clinical adoption broadens, the challenge will be to maintain standards for image quality, data management, and training across disciplines that historically have relied less on imaging.
The Role of Ultrasound in a Connected Healthcare Ecosystem
Another trend shaping the future of ultrasound is its integration within digital healthcare systems. Cloud-based image sharing and tele-ultrasound allow scans to be acquired in one location and interpreted in another, connecting rural clinics to urban hospitals.
Artificial intelligence and automation enhance this model by ensuring that remotely acquired images are of sufficient quality for accurate interpretation. This is particularly important in emergency response, battlefield medicine, and developing regions.
Combined with wearable technology and portable devices, ultrasound is becoming part of a broader ecosystem of connected diagnostics. This aligns with healthcare’s movement towards patient-centred care, continuous monitoring, and early intervention.
Challenges and Considerations
As with any rapidly evolving technology, ultrasound’s progress brings practical and ethical questions. The proliferation of devices outside traditional imaging departments raises issues of quality control and regulatory compliance. There is also the question of data security, particularly as AI systems process and store increasing volumes of image data in cloud environments.
Moreover, while automation reduces operator dependence, it must not lead to over-reliance on algorithms. Clinical interpretation and patient context remain irreplaceable components of diagnosis.
Cost and infrastructure are additional considerations. Advanced 3D and fusion imaging systems, while powerful, remain expensive. Achieving equitable access will depend on balancing innovation with affordability and sustainable deployment.
Conclusion
Ultrasound imaging stands at the forefront of a technological transformation. The integration of artificial intelligence, portable systems, and advanced imaging techniques is pushing it far beyond its traditional boundaries. What was once a static 2D tool has evolved into a dynamic, intelligent, and increasingly therapeutic modality.
From point-of-care diagnosis to non-invasive tumour ablation, ultrasound is redefining its role in modern medicine. Its combination of safety, versatility, and real-time capability ensures it will remain one of the most important imaging modalities in clinical practice.
As healthcare moves towards greater accessibility and personalisation, ultrasound embodies the principles of the next generation of medical imaging—fast, portable, intelligent, and patient-centred.
Disclaimer
The information presented in The Future of Ultrasound Imaging: Key Developments Shaping 2025 and Beyond is provided for general educational and informational purposes only. It does not constitute medical advice, diagnosis, or treatment, and should not be relied upon as a substitute for consultation with qualified healthcare professionals.
While every effort has been made to ensure the accuracy and reliability of the information at the time of publication, Open MedScience makes no representations or warranties of any kind, express or implied, regarding the completeness, accuracy, or currency of the content. Developments in medical technology and clinical practice may evolve rapidly, and readers are encouraged to verify information and consult relevant professional or regulatory sources before applying it in practice.
Any mention of specific companies, products, or technologies is for illustrative purposes only and does not imply endorsement or recommendation by Open MedScience. The views expressed are those of the author and do not necessarily reflect those of affiliated organisations or contributors.
Open MedScience accepts no responsibility for any loss, injury, or damage arising from the use of, or reliance on, the material presented in this article.
home » blog » medical imaging modalities »