Orthodontic treatment has advanced more in the past decade than in the preceding fifty years. Digital imaging, improved materials, and AI-assisted planning tools have changed how practitioners diagnose conditions and deliver clinical results. These changes affect every phase of care, from the initial diagnostic workup through the final retention stage. Patients today begin treatment with more clinical information available than previous generations ever had.
The shift reaches across practice types and geographic markets, affecting both how care is delivered and what clinical outcomes are realistically achievable. Sun Orthodontist, a multi-location practice based in Miami, Florida, represents the kind of provider that has incorporated several of these technologies into routine clinical workflow. Examining the science behind these tools and the evidence supporting their use gives a clearer basis for evaluating what they actually offer patients.
Three-Dimensional Imaging and Its Role in Diagnosis
Cone-beam computed tomography (CBCT) provides orthodontists with a full three-dimensional view of teeth, roots, jaw structure, and surrounding bone before treatment begins. Conventional radiographs show teeth in two dimensions and leave room for estimation that CBCT largely removes from the diagnostic process. A clinician can identify impacted teeth, measure bone density, and assess root positions before a single bracket is placed or an aligner ordered. That precision makes treatment planning more reproducible across a broader range of case complexity.
Research published through the National Library of Medicine has confirmed the diagnostic value of CBCT for complex orthodontic cases, including impacted canines, skeletal discrepancies, and root resorption assessment. These findings have contributed to broader adoption across specialty dental practices. That said, routine use of CBCT for straightforward cases remains a point of active discussion within the field. Current radiation dose considerations in dental cone beam imaging emphasise a selective approach, reserving higher dose modalities for cases where the additional diagnostic information genuinely changes the treatment plan.
Intraoral scanners have replaced physical alginate impressions at many practices. Patients receive a digital scan in place of impression trays, and the resulting 3D models transfer directly to labs or aligner fabrication software. Dimensional accuracy across intraoral scanners varies by device and operator, and full-arch scans can still introduce measurable deviations in the posterior segments, an area where research continues to refine protocols.
How Clear Aligner Materials Have Improved
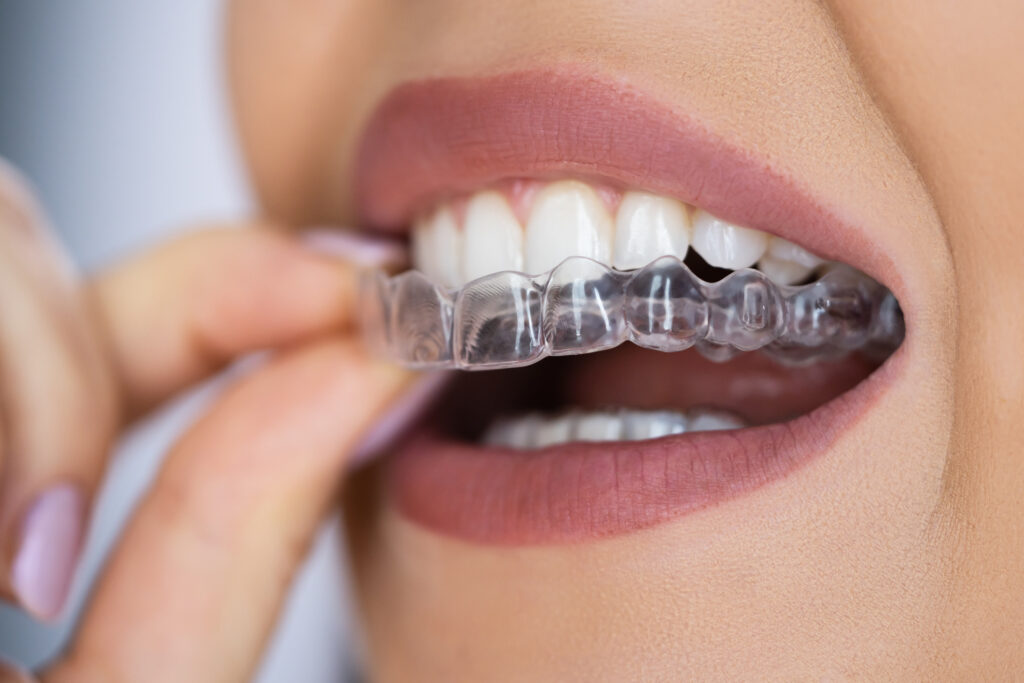
Clear aligners have been available since the late 1990s, but the materials and planning methods behind them have developed considerably over that period. Early systems had documented limits around tooth rotations, vertical movements, and bite correction. Current thermoplastic formulations maintain their shape more consistently under occlusal load and deliver steadier force levels over a full day of wear. Peer-reviewed literature has confirmed the expanded applicability of cases, though moderate to severe skeletal discrepancies generally still require fixed appliance support or adjunctive procedures.
Attachment protocols have extended what aligners can accomplish mechanically. Small composite bumps bonded to individual teeth allow aligners to apply forces at more controlled angles, enabling rotations and extrusions that flat plastic cannot produce without a direct physical contact point. Treatment simulation software lets clinicians visualise projected tooth movement before fabrication begins. Patients can review anticipated staging before committing to a plan, though it remains important to clearly communicate that digital simulations are projections, not guarantees of outcome.
The evidence base for aligner treatment has grown, but study quality varies. Many published trials have short follow-up periods or small sample sizes, and long-term retention data for aligner-treated cases continues to accumulate.
AI Assisted Planning and Cephalometric Analysis
Machine learning models trained on large radiographic and CBCT datasets can now complete cephalometric landmark identification in seconds. That process previously required careful manual tracing and introduced measurable inter-examiner variation. Automated analysis reduces that inconsistency and delivers a baseline within the timeframe of a single clinical appointment. For practices managing high patient volumes, this represents a practical change in diagnostic workflow.
Studies comparing AI-generated cephalometric analyses against those produced by experienced clinicians have found that automated systems perform within clinically acceptable tolerances on standardised datasets. Accuracy can decrease with lower-quality images or atypical anatomical presentations, precisely the cases where precise measurement matters most. The technology does not replace clinical judgment; it provides a faster starting point for a trained practitioner to refine the plan.
The crossover between automated landmark detection in medical imaging and orthodontic software has become increasingly direct. Methods developed in radiology research have been adapted for dental planning platforms, and the clinical validation of those adaptations is ongoing. Practitioners using AI-assisted tools should understand both what has been validated and where the training data may not reflect the full range of patient presentations they encounter.
Remote Monitoring Between Appointments
Remote monitoring has become a component of aligner-based treatment at many practices. Patients photograph their teeth using a smartphone app at set intervals, and a clinician reviews those images before approving advancement to the next tray. This approach maintains a degree of clinical oversight without requiring an office visit at every stage. Practices adopting remote monitoring have reported the ability to manage larger patient cohorts without proportional increases in chair time.
The clinical evidence supporting remote monitoring is still developing. Current studies suggest it is effective for detecting gross deviations from planned tooth movement, but photographic assessment has inherent limits compared to in-person clinical examination. Inter-arch relationships, gingival health, and certain attachment issues are difficult to evaluate reliably through consumer smartphone images. The American Association of Orthodontists has noted that remote monitoring should complement, rather than replace, scheduled clinical evaluations at appropriate intervals.
For patients with demanding schedules, periodic remote check-ins offer practical value in maintaining treatment continuity. The data generated through regular submissions also helps practices identify patterns in how specific case types respond over time, which has incremental value for refining future planning.
Bracket and Wire Technology in Fixed Appliances
Self-ligating brackets use a built-in clip rather than elastic ties to hold the archwire in the bracket slot. Reduced friction between the wire and bracket allows lighter forces to move teeth, and some clinical studies associate this with faster initial alignment and fewer discomfort episodes in early treatment. The evidence on whether self-ligation produces meaningfully faster overall treatment times remains mixed. Several controlled trials have found no statistically significant difference in total treatment duration compared to conventional bracket systems when other variables are held constant.
Archwire materials have developed in parallel. Nickel-titanium wires with shape-memory properties exert a continuous force as they return to their preset arch form throughout the wear cycle. Copper-nickel-titanium variants activate at body temperature and deliver more consistent force output across the day. These properties are most relevant during the levelling and alignment phase, where sustained light force tends to produce a more predictable cellular response than periodic heavy loading. Research in orthodontic biomechanics continues to examine optimal force levels for different tooth types and bone densities.
What the Evidence Suggests for Patients
No single technology determines whether orthodontic treatment succeeds. Clinical skill, diagnostic accuracy, and patient compliance all contribute in ways that the available tools cannot override. Practices that have adopted current methods have generally kept pace with the clinical literature behind them, but the presence of equipment alone does not confirm appropriate clinical application.
Patients evaluating a provider can ask a few direct questions to gauge the clinical approach:
- Is CBCT imaging reserved for cases with a genuine diagnostic need, with a clear explanation of why it is indicated?
- Are the limits of digital simulation explained before a treatment plan is finalised?
- Does remote monitoring supplement in-person visits rather than replace them entirely?
- Can the practice point to board certification and continuing education in the methods they use?
Orthodontic care has reached a point where better imaging data, improved materials, and communication tools together improve the predictability of many treatment types. Understanding where the evidence is strong, and where it is still accumulating, helps patients and practitioners make decisions grounded in what the science currently supports.
Disclaimer
This article is provided for general informational and educational purposes only and does not constitute medical, dental, or orthodontic advice, diagnosis, or treatment. The content reflects the understanding of the subject at the time of publication and should not be relied upon as a substitute for professional consultation with a qualified dentist, orthodontist, or other healthcare provider. Mention of specific practices, technologies, products, or providers does not imply endorsement by Open MedScience. Treatment suitability, risks, and outcomes will vary according to individual circumstances, and readers should seek personalised clinical advice before making decisions about orthodontic care.