Bone imaging is an essential diagnostic tool for detecting bone diseases, injuries, and disorders. With the ongoing advancements in imaging technology and the development of new imaging agents, the future of bone imaging looks promising, offering greater accuracy and precision in diagnosis and treatment.
Bone Imaging in Paget’s Disease: From Diagnosis to Monitoring Treatment Response
Bone scans use a radioactive tracer to create images of the bones. The tracer is injected into the bloodstream, accumulating in areas of the bone undergoing active growth or repair. Bone scans can detect bone fractures, infections, tumours, and conditions such as osteoporosis and Paget’s disease.
Bone imaging is a valuable tool for diagnosing and monitoring Paget’s disease. Paget’s disease is a bone disorder characterized by abnormal bone remodelling, leading to weakened bones, deformities, and pain. The following imaging modalities help to diagnose and monitor Paget’s disease:
- X-rays can detect the characteristic changes in bone structure in Paget’s disease. These changes include areas of increased bone density, called sclerotic lesions, and areas of bone thinning or osteoporosis circumscripta. X-rays can also detect deformities and fractures associated with Paget’s disease.
- Using radiopharmaceuticals, such as technetium-99m or fluorine-18, can provide a more comprehensive view of bone involvement in Paget’s disease. These scans can detect areas of increased bone turnover and activity and areas of decreased blood flow or avascular necrosis that can occur in advanced cases.
- CT scans can provide more detailed images of the bones affected by Paget’s disease, including bone deformity, thinning, or thickening. CT scans are beneficial for evaluating the spine and other areas where X-rays may not provide a complete picture.
- MRI can provide detailed images of soft tissue, which can help detect nerve or spinal cord compression associated with advanced Paget’s disease. MRI is also useful for detecting areas of bone marrow oedema, indicating areas of increased bone activity or inflammation.
Bone Imaging with Technetium-99m
Technetium-99m (Tc-99m) is a radioisotope commonly used in bone imaging. A medical cyclotron or generator produces it from its parent isotope, molybdenum-99 (Mo-99). Tc-99m has a short half-life of about 6 hours, making it ideal for medical imaging because it allows imaging studies to be completed within a reasonable time.
In bone imaging, Tc-99m is typically injected intravenously, accumulating in areas of the bone undergoing active growth or repair. This makes it useful for detecting various bone conditions, including fractures, infections, tumours, and degenerative bone diseases.
Tc-99m bone imaging can be achieved in several ways, including planar imaging, SPECT (single-photon emission computed tomography), and hybrid imaging (such as SPECT/CT or SPECT/MRI). Planar imaging involves taking two-dimensional images of the bone, while SPECT imaging involves three-dimensional images that can provide more detailed information about the bone structure and function.
Strontium-89 for the Palliative Treatment of Bone Pain in Metastatic Cancer
Strontium-89 (Sr-89) is not used in bone imaging but rather as a treatment for metastatic bone cancer to relieve bone pain. Sr-89 is a radioactive isotope similar in structure to calcium, especially taken up by bone tissue. Once injected into the bloodstream, it accumulates in areas of the bone undergoing active growth or repair, such as those affected by bone metastases.
The radioactive decay of Sr-89 emits beta particles, which can penetrate the bone tissue and destroy the cancer cells within the bone. This can lead to pain relief and improved quality of life for patients with metastatic bone cancer.
While Sr-89 is not used for diagnostic bone imaging, it can be imaged using nuclear medicine techniques such as gamma camera imaging, confirming the radioactive isotope uptake in the bone tissue.
Furthermore, Sr-89 is a valuable treatment option for patients with metastatic bone cancer who are experiencing bone pain, and it can provide significant pain relief and improved quality of life.
Samarium-153 for the Treatment of Bone Pain in Metastatic Cancer
Samarium-153 (Sm-153) is not typically used in bone imaging but rather as a treatment for bone pain associated with metastatic bone cancer. Sm-153 is a radioactive isotope similar in structure to calcium, preferentially taken up by bone tissue. Once injected into the bloodstream, it accumulates in areas of the bone undergoing active growth or repair, such as those affected by bone metastases.
The radioactive decay of Sm-153 emits beta particles, which can penetrate the bone tissue and destroy the cancer cells within the bone. This can lead to pain relief and improved quality of life for patients with metastatic bone cancer.
Consequently, Sm-153 is not used for diagnostic bone imaging. It can be imaged using nuclear medicine techniques such as gamma camera imaging, confirming the radioactive isotope uptake in the bone tissue.
However, Sm-153 is a valuable treatment option for patients with metastatic bone cancer who are experiencing bone pain, and it can provide significant pain relief and improved quality of life.
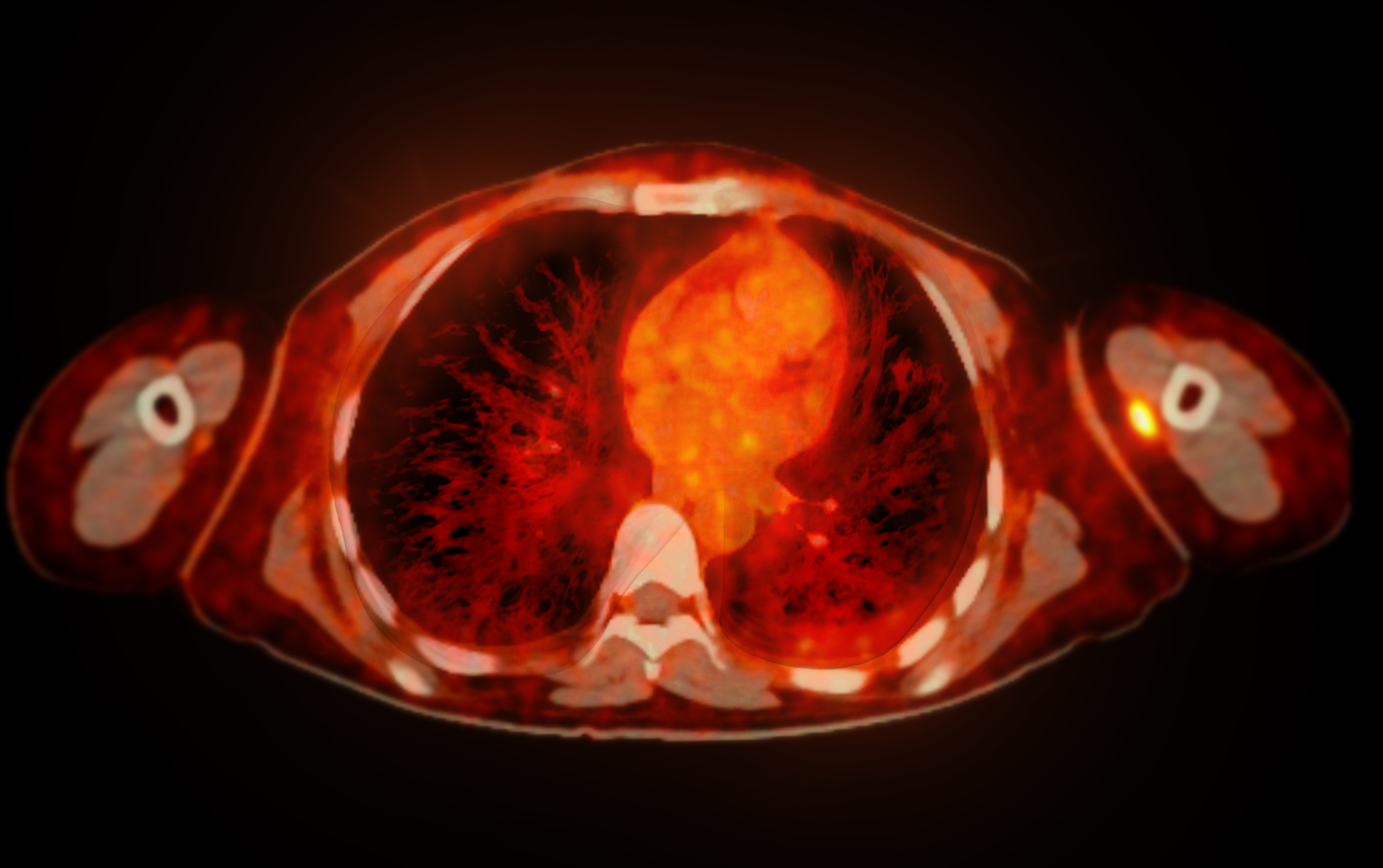
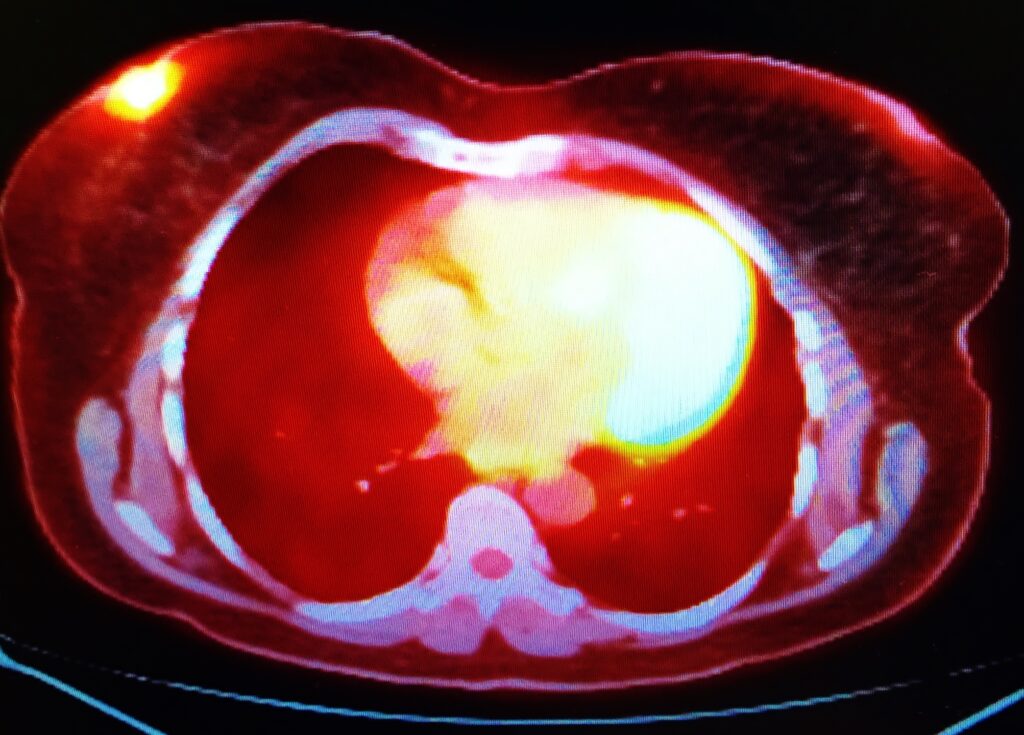
Fluorine-18 as a Tracer in PET Bone Imaging
Fluorine-18 (F-18) is not typically used as the primary imaging agent in bone imaging but as a tracer in PET (positron emission tomography) bone imaging. F-18 is a radioisotope commonly used in PET imaging due to its short half-life of about 110 minutes, which allows imaging studies to be completed relatively quickly.
In PET bone imaging, F-18 is typically administered intravenously, and the bone tissue takes it up in a manner similar to Tc-99m. However, F-18 detects bone metastases in cancer patients and evaluates treatment effectiveness.
PET imaging using F-18 can provide valuable information about the structure and function of the bone tissue, and it can help to detect bone abnormalities at an earlier stage than other imaging modalities.
F-18 PET bone imaging can be combined with other imaging modalities, such as CT (computed tomography) or MRI (magnetic resonance imaging), to provide more detailed information about the bone tissue and surrounding structures.
Overall, F-18 PET bone imaging is a valuable tool for detecting bone metastases and other bone abnormalities, and it can provide vital information to guide treatment decisions and monitor disease progression.
Radiopharmaceuticals used in Bone Imaging
Several new imaging agents in bone imaging have shown promise in preclinical and clinical studies. These agents can provide more accurate and specific information about bone structure and function, improving the diagnosis and treatment of bone disorders, for example:
- Sodium fluoride (NaF) PET is a promising imaging agent to detect increased bone activity and remodelling areas. This makes it particularly useful for the detection of bone metastases in cancer patients, as well as for the evaluation of bone mineral density and turnover in osteoporosis and other metabolic bone disorders.
- Radium-223 (Ra-223) dichloride is a radiopharmaceutical that can selectively target areas of bone affected by metastatic prostate cancer. It emits alpha particles that can penetrate bone tissue and kill cancer cells while sparing surrounding healthy tissue. Ra-223 has been shown to improve survival in patients with metastatic prostate cancer and has been approved by the FDA for this indication.
- Gadolinium-based contrast agents (GBCAs) for MRI are commonly used in MRI to enhance the contrast between tissues and improve the accuracy of diagnosis. Newer GBCAs that target specific molecular markers associated with bone diseases, such as integrins and osteoclasts, are being developed and tested in preclinical and clinical studies.
- Osteocalcin-targeted imaging agents: Osteocalcin is a protein produced by bone-forming cells called osteoblasts. Targeted imaging agents that bind specifically to osteocalcin, such as radiolabeled antibodies and peptides, are being developed and tested to detect bone metastases and other bone disorders.
The Future of Bone Imaging: An Overview of Emerging Technologies and Applications
The future of bone imaging is promising, with ongoing advancements in imaging technology and the development of new imaging agents. The key trends and developments in the field include:
- There is growing interest in using molecular imaging techniques to detect bone disease at an earlier stage and monitor treatment response more accurately. This includes using targeted imaging agents that can bind specifically to molecules associated with bone diseases, such as cancer cells or inflammatory markers.
- Artificial intelligence (AI) and machine learning algorithms are being developed to analyze large amounts of imaging data and extract meaningful information about bone structure and function. This could help to improve the accuracy and speed of diagnosis and treatment planning.
- Combining multiple imaging modalities, such as PET/CT or MRI/SPECT, is becoming increasingly popular for bone imaging. These hybrid scanners provide more comprehensive and accurate information about bone tissue and surrounding structures.
- Advances in 3D printing technology are being used to create anatomically accurate models of bone tissue for surgical planning and educational purposes. These models can be customized to each patient’s specific anatomy and can help improve surgical procedures’ accuracy and safety.
- Portable bone imaging devices are being developed to be used at the point of care, such as in emergency departments or remote locations. This could help to improve access to bone imaging for patients who may not have easy access to traditional imaging facilities.
The future of bone imaging is exciting, with technological advancements and the development of new imaging agents that can improve the accuracy and speed of diagnosis and treatment planning for a wide range of bone conditions and injuries. For example, radioisotopes are a valuable tool in bone imaging because they allow for the detection of bone abnormalities at a molecular level, which can lead to earlier detection and treatment of bone conditions.
Disclaimer
The content provided in this article, “Nuclear Medicine Techniques for Bone Imaging and Cancer Diagnosis”, is intended for informational and educational purposes only. It does not constitute professional medical advice, diagnosis, or treatment, and should not be relied upon as such. Readers are encouraged to consult qualified healthcare professionals for medical concerns or questions related to bone imaging or cancer diagnosis and treatment.
The information reflects the knowledge and understanding available at the time of publication (18 March 2023) and may not represent the most current developments in nuclear medicine or imaging technologies. Open Medscience makes every effort to ensure the accuracy of the information provided but does not guarantee its completeness or reliability.
Mentions of specific radiopharmaceuticals, imaging agents, or techniques are included to inform and illustrate current practices and emerging options; they do not imply endorsement or recommendation by Open Medscience or its contributors. Use of any diagnostic or therapeutic method should be based on individual clinical evaluation and local regulatory guidelines.
Open Medscience and its authors accept no liability for any loss, injury, or damage resulting from the use of information contained in this article.
home » blog » nuclear medicine imaging »