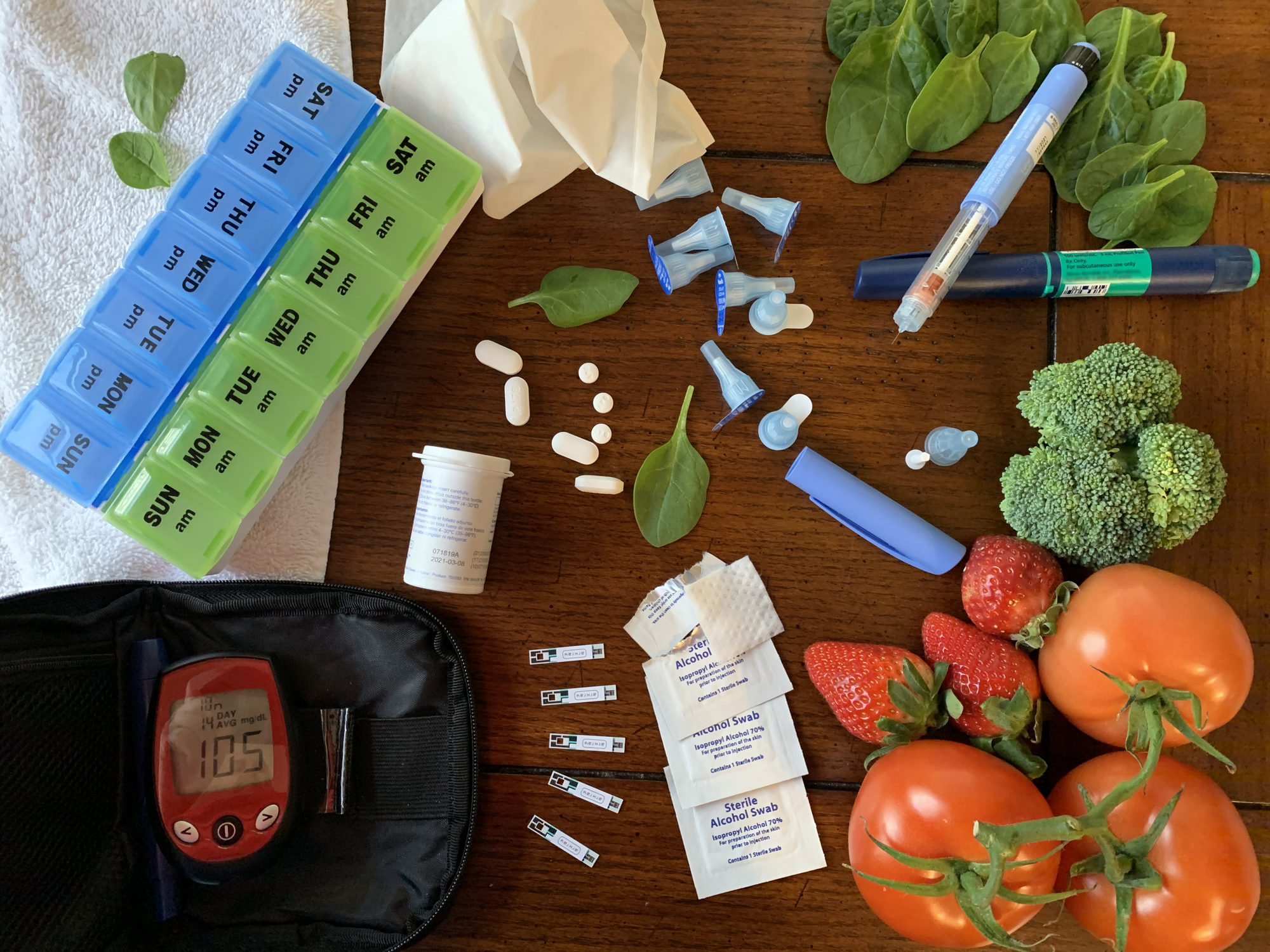
Summary: Managing type 2 diabetes involves balanced eating, regular exercise, correct use of medication, and looking after mental wellbeing. People can maintain steady blood sugar levels and reduce the risk of complications by making thoughtful lifestyle adjustments and staying informed about treatment options.
Keywords: Diabetes; Blood sugar; Nutrition; Exercise; Monitoring; Support.
Introduction to Type 2 diabetes
Type 2 diabetes is a long-term condition that affects how the body regulates blood sugar. When someone develops type 2 diabetes, their body either resists the effects of insulin—an essential hormone produced by the pancreas—or does not produce enough insulin to keep blood sugar levels within a healthy range. As a result, glucose can build up in the bloodstream and lead to a variety of potential complications, including cardiovascular problems, nerve damage, and vision issues.
Although a diagnosis of type 2 diabetes can feel overwhelming, a proactive and informed approach makes a significant difference in managing the condition day to day. Through consistent meal planning, regular physical activity, and thoughtful monitoring of blood sugar levels, many individuals can continue pursuing the activities they enjoy while preserving good health. For those seeking extra guidance on how to simplify this process, resources like FeelGreatAgain provide wellness guidance and lifestyle insights that make healthy changes feel achievable rather than daunting.
The path to living well with type 2 diabetes also entails understanding what triggers changes in blood sugar, recognising symptoms of high or low blood sugar, and learning how to work with healthcare professionals to optimise treatment.
Self-management is key. Whether an individual is newly diagnosed or has been living with type 2 diabetes for many years, maintaining a realistic outlook, educating oneself, and adapting habits to address changing needs are all critical. As technology advances, tools for continuous blood sugar monitoring and new medication options are becoming more widely available, which further helps individuals keep diabetes under control.
The following sections examine essential factors that contribute to a sustainable lifestyle for those with type 2 diabetes. These include dietary considerations, strategies for staying physically active, key information on medication use, methods for blood sugar tracking, and ways to look after one’s emotional health. By focusing on these aspects, people with type 2 diabetes can aim for a balanced, productive, and enjoyable life.
Understanding Type 2 Diabetes
Type 2 diabetes is characterised by insulin resistance, which means the body does not respond to insulin as effectively as it should. Insulin is responsible for helping glucose enter cells, where it can be used as energy. When cells do not respond well to insulin, blood glucose levels increase. Over time, this can lead to a higher risk of complications, such as cardiovascular disease, kidney problems, and nerve damage.
A number of factors contribute to the development of type 2 diabetes. Genetics can play a role; those with close relatives who have diabetes may be more susceptible to it themselves. Lifestyle factors, such as inactivity and a diet high in refined carbohydrates, processed foods, and sugary drinks, also significantly impact the risk of developing the condition. Additionally, being overweight and obese increases the likelihood of developing insulin resistance.
The hallmark symptoms of type 2 diabetes include frequent urination, heightened thirst, increased hunger, fatigue, blurred vision, and slow wound healing. However, some individuals have only mild symptoms or none at all, especially in the early stages. This makes regular check-ups and blood sugar testing particularly important for early detection.
Diagnosing type 2 diabetes typically involves measuring blood glucose levels through tests such as fasting plasma glucose, oral glucose tolerance, or HbA1c tests, which indicate average blood sugar levels over approximately three months. Once a diagnosis is confirmed, doctors often recommend lifestyle interventions as the first line of management. These interventions aim to help individuals reach a stable weight, adopt healthier eating habits, and incorporate more physical activity. In some instances, medication becomes necessary if lifestyle changes alone are not enough to keep blood sugar levels within an acceptable range.
Understanding the core aspects of type 2 diabetes helps demystify the condition. Individuals can start making targeted decisions that promote better long-term health by acknowledging how and why it develops. This foundational knowledge also fosters more productive communication with healthcare teams, enabling people to ask informed questions and take an active role in their care plan.
The Importance of Balanced Nutrition
One of the most powerful tools for managing type 2 diabetes is a well-planned diet. Paying attention to portion sizes and nutrient composition can help keep blood sugar stable throughout the day. Although there is no single “perfect” meal plan for everyone with type 2 diabetes, many find success by focusing on whole foods that are nutrient-dense and lower in refined sugars.
Carbohydrate Awareness
Carbohydrates have the most significant direct impact on blood sugar levels. When carbohydrates are broken down, they turn into glucose, which enters the bloodstream. This means choosing carbohydrates that are absorbed more gradually, such as whole grains, legumes, and vegetables. These options often contain more fibre, which helps with digestion and slows the release of glucose into the bloodstream. In contrast, refined carbohydrates like white bread, sugary cereals, and pastries can cause sudden spikes in blood sugar.
Protein and Healthy Fats
Protein sources such as lean meats, fish, eggs, beans, and lentils offer essential building blocks for muscle repair and other bodily functions. They also tend to have a minimal effect on blood sugar levels when consumed in moderation. Likewise, healthy fats—found in foods such as avocados, nuts, seeds, and olive oil—support heart health and help individuals feel full.
Meal Timing and Portion Control
It matters not only what one eats but also when one eats. Eating smaller, balanced meals spaced evenly throughout the day can help regulate blood sugar more effectively than having a few large meals. For instance, consuming a small breakfast, a medium-sized lunch, and a balanced dinner with small snacks in between (if needed) helps keep energy levels steadier. Portion sizes also play a major role. Even foods that are considered healthy can lead to higher blood sugar if eaten in large quantities.
Mindful Eating Habits
Mindful eating involves paying attention to hunger and fullness cues, eating slowly, and truly savouring each bite. This approach can reduce overeating and help people make more deliberate food choices. Minimising distractions during meals—like watching television or scrolling through a phone—allows individuals to focus more on how they feel as they eat, which often leads to better portion control.
Working with Nutrition Professionals
For people who require more personalised guidance, consulting a registered dietitian or diabetes educator can be beneficial. These professionals can help tailor a meal plan that aligns with individual health goals, cultural preferences, and any other medical considerations. By learning to read food labels, track carbohydrate intake, and balance meals, individuals become better equipped to make long-term dietary changes that support stable blood sugar levels.
Physical Activity: Key to Blood Sugar Control
Exercise is another mainstay in the management of type 2 diabetes. Regular physical activity helps the body use insulin more efficiently and can lower blood sugar levels. It also supports weight management, cardiovascular health, and mental wellbeing.
Types of Exercise
A blend of aerobic and strength-training activities often provides the best results for people with type 2 diabetes. Aerobic exercises, such as brisk walking, cycling, or swimming, increase the heart rate and burn calories. Strength-training exercises like weightlifting, resistance band workouts, or bodyweight exercises help build and maintain muscle mass, increasing the number of calories burned at rest and improving insulin sensitivity.
Incorporating Exercise into Daily Life
For some, dedicating time exclusively to the gym might be difficult. However, many activities throughout the day can contribute to better fitness. Going for short walks after meals, using the stairs instead of a lift, or even doing household chores that involve active movement can all add up. The key is consistency. Small bursts of activity throughout the day can positively affect blood sugar and overall health.
Precautions and Planning
Before beginning a new exercise routine, it is wise for individuals with type 2 diabetes to speak with a healthcare provider, especially if they have other conditions like high blood pressure or complications related to diabetes. Monitoring blood sugar levels before and after exercise is also advisable to understand how physical activity affects them. People at risk of hypoglycaemia may need to have a small snack before exercising or carry glucose tablets.
Staying Motivated
Consistency is more likely when an individual genuinely enjoys the activities they choose. That might mean dancing, playing a sport, or simply going for a scenic walk. Setting realistic goals and tracking progress—whether through a fitness app, a journal, or a supportive group—can also help maintain motivation. Celebrating small achievements, such as walking longer without feeling tired, can inspire individuals to continue working on their fitness.
Medication and Blood Sugar Monitoring
While lifestyle modifications form a cornerstone of type 2 diabetes management, medication also plays a key role for many people. Medications help lower blood sugar in different ways, from increasing insulin sensitivity to slowing carbohydrate absorption. Understanding how these medications work and adhering to proper monitoring practices ensures the best possible outcomes.
Common Medications for Type 2 Diabetes
- Metformin: Often prescribed as a first-line treatment, metformin works by lowering glucose production in the liver and improving insulin sensitivity.
- Sulfonylureas (e.g., gliclazide): Stimulate the pancreas to produce more insulin.
- DPP-4 Inhibitors (e.g., sitagliptin): Help boost levels of hormones that encourage the pancreas to release insulin when blood sugar levels are high.
- GLP-1 Receptor Agonists (e.g., liraglutide): Slow digestion and help the pancreas release insulin more effectively. These may also assist with weight management.
- SGLT2 Inhibitors (e.g., canagliflozin): Promote the elimination of glucose through urine, lowering blood sugar levels.
- Insulin: Some individuals need insulin injections to compensate for their body’s insufficient insulin production or high resistance.
The Role of Blood Sugar Monitoring
Regularly tracking blood sugar levels allows individuals to see how their body responds to various factors, including meals, exercise, stress, and medications. Monitoring can be done with a blood glucose meter by pricking the finger for a drop of blood. Alternatively, continuous glucose monitors (CGMs) provide real-time readings throughout the day and night. These devices often help people fine-tune their daily choices with fewer interruptions for manual testing.
Effective Use of Medication
Taking medication at the right time and in the right dose is crucial for achieving stable blood sugar control. Skipping doses or taking medication inconsistently can result in large fluctuations in blood sugar and increase the risk of complications. Healthcare providers may adjust dosages or switch medications if someone experiences side effects or if a medication becomes less effective over time.
Communication with Healthcare Teams
Staying in regular contact with doctors, diabetes educators, or nurses supports better medication management. Appointments provide opportunities to discuss any side effects, challenges with adherence, or issues with blood sugar levels. Over time, treatment plans may need to be adjusted to reflect changes in weight, activity level, or the progression of diabetes itself.
Emotional Wellbeing and Support
Living with type 2 diabetes requires ongoing attention to daily routines and can bring challenges that affect emotional health. Feelings of stress, anxiety, or frustration are not uncommon, and these emotions can sometimes impact blood sugar control. By seeking the right kind of support and employing strategies to manage stress, individuals can protect their emotional wellbeing alongside their physical health.
Recognising Emotional Stress
Stress can elevate blood sugar levels because of hormonal changes in the body. Identifying the sources of stress—be it job-related concerns, family responsibilities, or financial worries—allows individuals to create coping strategies. Some might benefit from setting realistic goals rather than aiming for perfection, as high standards can lead to disappointment if blood sugar fluctuates.
Strategies for Stress Management
Techniques like deep breathing exercises, progressive muscle relaxation, and gentle forms of yoga can help lower stress hormone levels and improve focus. Engaging in hobbies or creative pursuits, such as painting or gardening, offers a welcome distraction and fosters a sense of achievement. Setting aside time for relaxation, whether it is reading a good book or enjoying time with loved ones, can restore a sense of balance.
Professional Support
Mental health professionals, such as counsellors or psychologists, can offer valuable techniques for coping with the emotional pressures of diabetes. Cognitive behavioural therapy (CBT) helps individuals identify negative thought patterns and replace them with more positive, constructive ones. Group therapy sessions or support groups connect people who share similar experiences, enabling them to learn from each other’s challenges and successes.
Family and Social Support
In many cases, family and friends can provide invaluable support. Educating loved ones about type 2 diabetes encourages them to offer understanding and assistance, whether it is reminding someone to check their blood sugar or planning shared meals that align with healthy eating guidelines. Participating in community programmes, whether online or in person, can also foster a sense of belonging. Being part of a supportive environment helps reduce feelings of isolation and encourages lasting changes in lifestyle.
Long-Term Strategies and Conclusion
Managing type 2 diabetes is an ongoing process that evolves over time. What works well at one stage in life may require adjustments later due to ageing, changes in activity level, or shifts in personal preferences. Maintaining a flexible mindset and remaining open to trying new approaches can pave the way for sustained success.
Regular Check-ups and Screenings
Routine medical appointments are essential for the early detection of any complications that may arise. These include annual eye exams to look for changes in the retina, foot checks to spot nerve damage or circulation problems, and regular blood tests to monitor kidney function. Staying on top of these check-ups allows for early intervention and helps prevent problems from worsening.
Adapting as Needed
Life events such as changes in job schedules, family responsibilities, or unexpected health issues can disrupt routines. During these times, it may help to revisit dietary plans, exercise regimens, and medication schedules. In some cases, new therapies or tools might be introduced, such as insulin pumps or advanced glucose monitoring systems. Seeking guidance from healthcare providers during transitions helps keep diabetes management on track.
Personal Accountability and Self-Monitoring
Taking ownership of one’s health fosters better outcomes. This could involve setting reminders to take medication, using a smartphone app to record blood sugar readings, or scheduling regular consultations with a dietitian. When individuals track their daily choices—what they eat, how they exercise, and how they feel—it becomes easier to spot patterns and make informed adjustments.
Building a Support Network
A solid support network encompasses healthcare professionals, family members, and peers who understand the demands of living with type 2 diabetes. Beyond medical care, emotional encouragement is equally important. Sharing challenges, celebrating progress, and exchanging practical tips can reinforce healthy habits and reduce feelings of isolation.
Looking Ahead
Ongoing research in diabetes management continues to introduce novel treatments and cutting-edge technology, increasing the range of options available. While adjustments and monitoring remain necessary, these advancements can potentially simplify daily routines and offer greater flexibility. Staying informed about new developments, whether through reputable health websites, diabetes magazines, or support groups, can help individuals discover tools that enhance their quality of life.
Conclusion
Living with type 2 diabetes is an active, daily commitment, but it does not have to diminish one’s enjoyment of life. Through balanced nutrition, regular physical activity, responsible use of medication, and mindful monitoring of blood sugar, individuals can greatly reduce risks associated with the condition. Emotional wellbeing is equally important, and having access to social and professional support can ease the challenges that arise. By combining these elements into a cohesive approach and remaining adaptable to changing circumstances, people with type 2 diabetes can maintain good health and continue engaging in the activities they treasure.
Disclaimer
The content of this article is intended for general informational purposes only and should not be considered medical advice, diagnosis, or treatment. Individuals living with type 2 diabetes should consult with qualified healthcare professionals before making any changes to their diet, medication, physical activity, or self-management routines. While every effort has been made to ensure the accuracy of the information presented, Open Medscience does not accept any liability for any loss, injury, or damage incurred as a result of reliance on this content. Always seek personalised advice from your GP, diabetes nurse, or specialist care team.