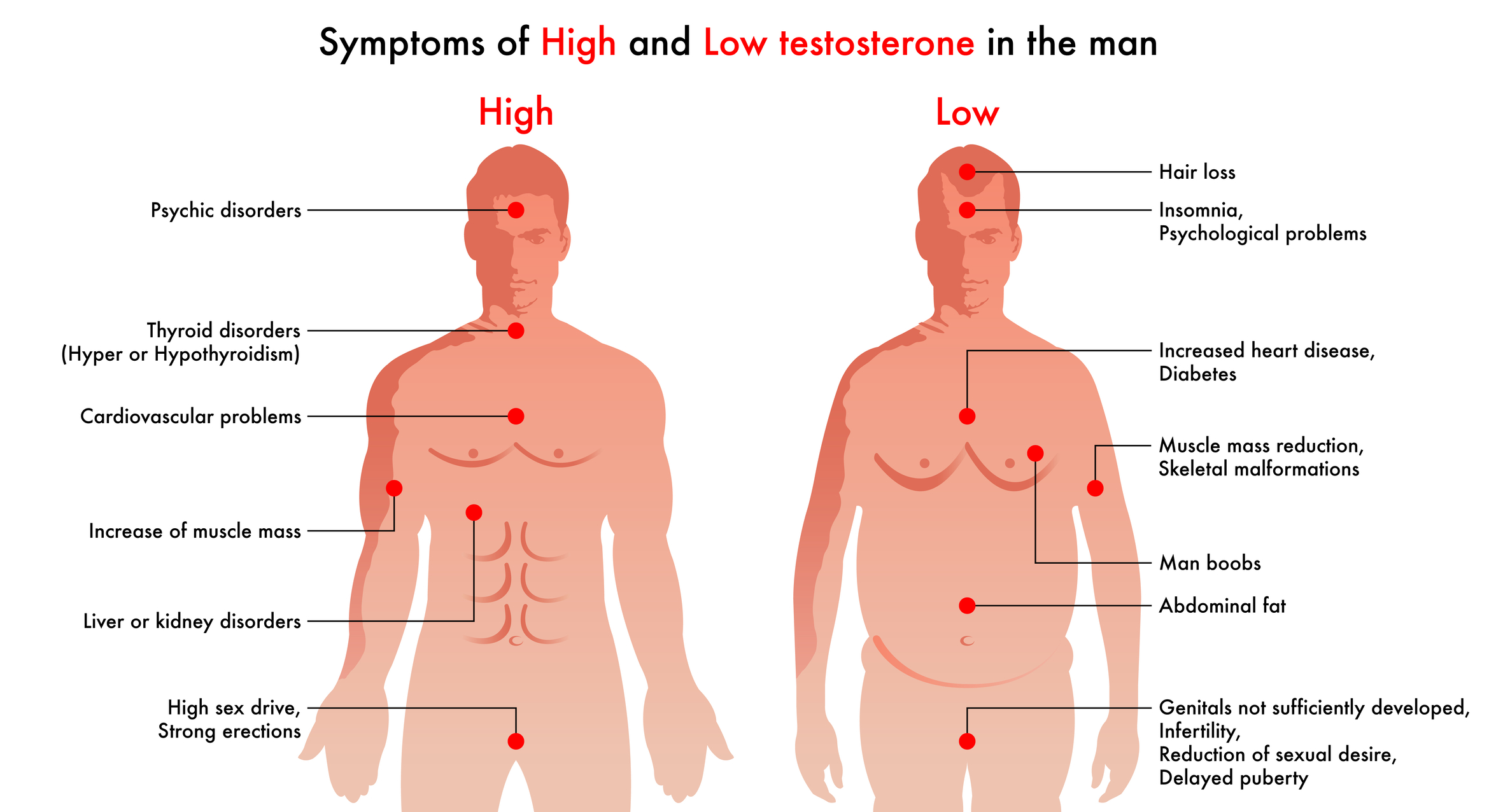
Testosterone deficiency is a clinically recognised condition affecting men that extends far beyond reduced libido. Testosterone plays a central role in metabolic function, muscle maintenance, cognitive performance, and cardiovascular health. While a decline in testosterone levels is expected with age, a subset of men experiences a more significant drop that leads to measurable symptoms and health risks.
From a medical standpoint, testosterone deficiency, often referred to as hypogonadism, can arise from primary testicular dysfunction or secondary causes involving the hypothalamic-pituitary axis. The distinction matters because it influences both testosterone deficiency diagnosis and its treatment strategy. Importantly, not all cases are age-related.
Lifestyle factors, chronic stress, obesity, and systemic disease contribute to hormonal imbalances in men, making this a multifactorial issue rather than a simple consequence of ageing.
Diagnostic Criteria and Clinical Evaluation
A proper testosterone deficiency diagnosis requires both biochemical evidence and clinical symptoms. Relying on lab values alone can lead to underdiagnosis, especially when individuals fall within the lower end of “normal” reference ranges but still experience dysfunction.
Biochemical Assessment
Standard diagnostic protocols include:
- Morning total testosterone measurements, ideally repeated on separate days
- Free testosterone evaluation for cases with altered SHBG levels
- Supporting labs such as LH, FSH, and prolactin
Clinicians must interpret these results in context. A man with borderline levels and clear symptoms of low testosterone may still warrant further evaluation. This is particularly relevant in cases of testosterone decline with age, where reference ranges may not reflect optimal physiological function.
Symptom Correlation
The clinical picture is equally important. Fatigue, reduced strength, and cognitive changes are often early indicators. Effective management of low testosterone levels begins with recognising these patterns rather than dismissing them as normal ageing.
A comprehensive approach also considers broader endocrine health. Thyroid dysfunction, insulin resistance, and adrenal imbalances frequently coexist, contributing to a wider hormonal imbalance in men.
Symptom Burden and Systemic Impact
Symptoms of low testosterone in men are diverse and affect multiple systems. Understanding this symptom burden is critical for both patients and clinicians.
Physical Manifestations
Common physical symptoms include:
- Decreased muscle mass and strength
- Increased visceral fat
- Persistent fatigue
These changes are often gradual but can significantly impact the quality of life.
Sexual and Reproductive Health
Sexual health is one of the most noticeable areas affected by testosterone deficiency in men. Symptoms include:
- Reduced libido
- Erectile dysfunction
- Decreased sexual performance
These issues are not purely psychological and often reflect underlying endocrine dysfunction.
Cognitive and Emotional Effects
Testosterone also influences brain function. Men may experience:
- Brain fog and reduced focus
- Mood instability
- Decreased motivation
These cognitive symptoms are frequently misattributed to stress or burnout, delaying accurate diagnosis.
Incorporating integrative health approaches that address sleep, nutrition, and stress management can help identify and mitigate contributing factors before symptoms worsen.
Why Testosterone Deficiency Is Often Missed
Despite its prevalence, testosterone deficiency in men is frequently overlooked. Several factors contribute to this gap in care.
Limitations of Standard Lab Ranges
Laboratory reference ranges are based on population averages, not optimal health markers. As a result, men with clinically significant symptoms may still fall within “normal” values.
Symptom Overlap with Other Conditions
Symptoms of low testosterone often overlap with:
- Depression
- Chronic fatigue
- Metabolic syndrome
This overlap leads to misdiagnosis and fragmented care, particularly when the underlying hormonal imbalance is not addressed.
Incomplete Evaluations
Many initial assessments do not include a full hormonal panel. Without a comprehensive view, clinicians may miss the broader endocrine context necessary for accurate testosterone deficiency diagnosis.
The Role of Testosterone Replacement Therapy
Testosterone replacement therapy (TRT) is a clinically validated treatment for men with confirmed deficiency. Its goal is to restore testosterone levels to a physiological range and alleviate symptoms.
Mechanism and Delivery Methods
TRT works by supplementing endogenous testosterone through:
- Intramuscular injections
- Transdermal gels or patches
- Subcutaneous pellets
The choice of method depends on patient preference, absorption variability, and clinical considerations.
Clinical Benefits
When appropriately prescribed, TRT can lead to:
- Improved energy and physical performance
- Increased lean muscle mass
- Enhanced libido and sexual function
- Better cognitive clarity
These benefits address both the physical and psychological aspects of testosterone deficiency in men.
Monitoring and Safety
TRT is not a one-time intervention. Ongoing monitoring is essential to ensure safety and effectiveness. This includes:
- Regular bloodwork
- Hematocrit and lipid monitoring
- Hormonal balance adjustments
Lifestyle factors remain important. For example, adequate recovery is critical, as regular rest improves productivity and supports hormonal regulation.
Identifying Appropriate Candidates for TRT
Not all individuals with low-normal testosterone levels require treatment. Candidates for TRT typically meet the following criteria:
- Persistent symptoms of low testosterone
- Consistently low biochemical levels
- No contraindications, such as untreated prostate conditions
In cases of testosterone decline due to age, treatment decisions should be individualised. The presence of functional impairment is often a more meaningful indicator than age alone.
Addressing contributing factors such as obesity, poor sleep, and chronic stress is equally important. These elements play a significant role in hormonal imbalance and may influence treatment outcomes.
A Broader Perspective on Hormone Optimisation
Modern approaches to diagnosing testosterone deficiency increasingly emphasise personalisation. Rather than focusing solely on testosterone levels, clinicians evaluate the entire hormonal network.
This includes:
- Thyroid function
- Cortisol patterns
- Insulin sensitivity
Such a comprehensive strategy helps identify root causes and supports long-term outcomes. In many cases, optimising overall health can enhance the effectiveness of TRT or reduce the need for higher doses.
When to Seek Medical Evaluation
Men experiencing persistent fatigue, reduced performance, or sexual health changes should consider checking their testosterone levels. Early assessment allows for timely intervention and reduces the risk of long-term complications.
A structured evaluation ensures that both biochemical data and clinical symptoms are considered, leading to a more accurate diagnosis.
Reframing Men’s Health Through Hormonal Insight
Testosterone deficiency should not be viewed as an inevitable part of men’s ageing. While testosterone decline with age is common, the associated symptoms and health risks are not something individuals need to accept without question.
A precise testosterone deficiency diagnosis, combined with appropriate use of TRT and lifestyle optimisation, can significantly improve quality of life. Recognising the broader context of hormonal imbalance in men allows for more effective, individualised care that addresses both symptoms and underlying causes.
Disclaimer: This article is for general information only and does not constitute medical advice, diagnosis, or treatment. Testosterone deficiency and TRT should be assessed and managed by a qualified healthcare professional. Do not start, stop, or change any treatment without seeking medical advice.
home » blog » health and wellbeing »