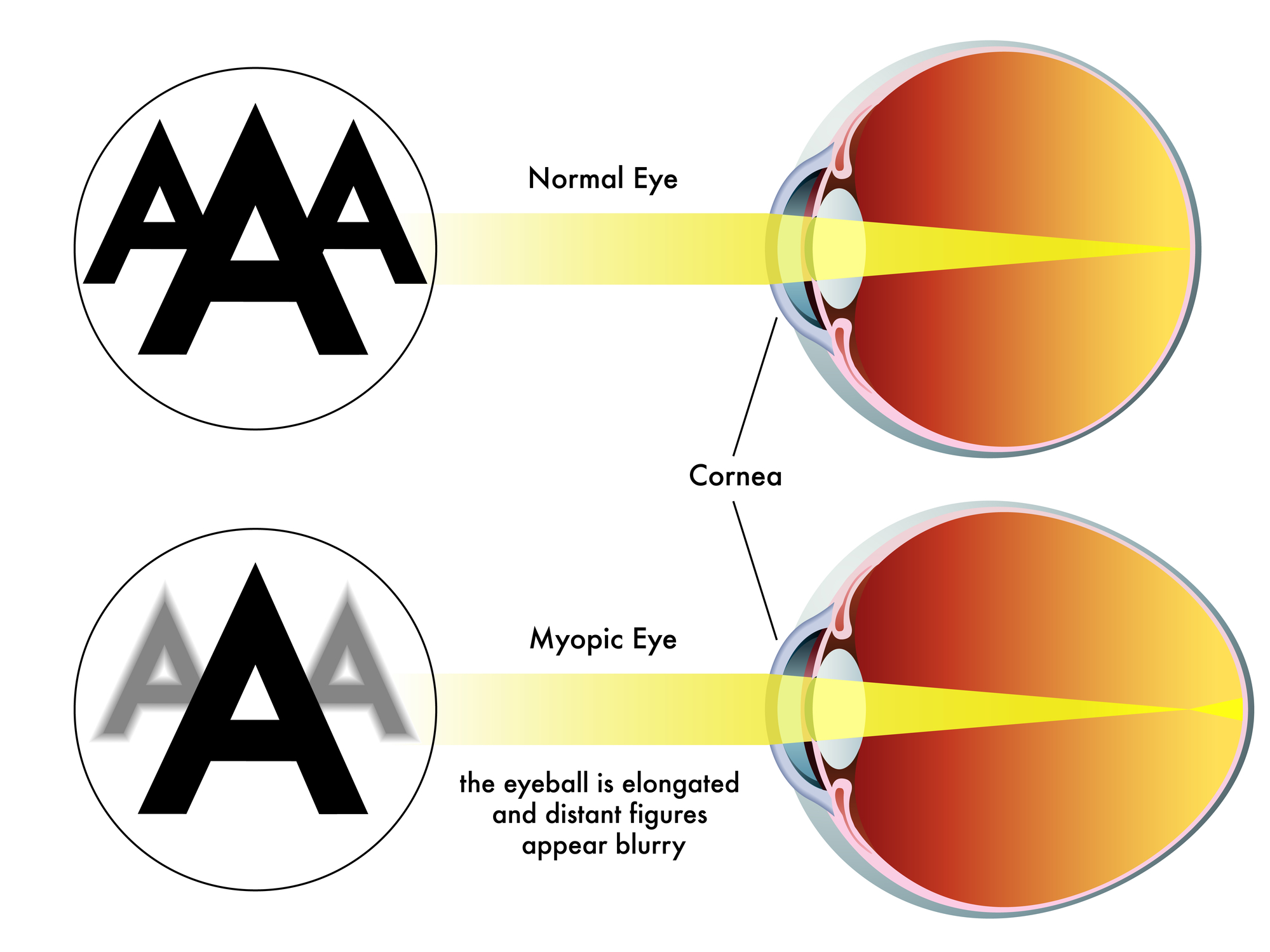
Contact lens intolerance can feel confusing because the change is often gradual at first. A person may wear lenses comfortably for years, then start noticing dryness late in the day, irritation after screen time, or a growing need for rewetting drops. Over time, those small changes can become a pattern of discomfort that is harder to ignore. For some patients, that is the point when SMILE eye surgery enters the conversation as a possible alternative to ongoing lens dependence [13].
Contact lens intolerance is not one single diagnosis. It is a practical description of a situation in which lens wear no longer feels sustainable, comfortable, or reliable enough for daily life. Research on contact lens discomfort and dry eye has linked symptoms to tear film instability, ocular surface stress, environmental conditions, and lens-related factors, while refractive surgery literature has also shown that preoperative dry eye and contact lens history matter when evaluating surgical candidates [1,2,4,5].
Why can contact lens intolerance appear slowly, then all at once?
Contact lens intolerance often develops like a slow accumulation problem. The eyes may compensate for months or years before symptoms become obvious. Then, what used to feel normal starts feeling unreliable. Late-day dryness becomes an everyday issue. Lenses become harder to tolerate in air-conditioned rooms, on flights, during long workdays, or after hours of computer use. Reviews of contact lens discomfort describe this problem as a frequent reason for reduced wearing time and discontinuation, and dry eye research points to tear film disruption and ocular surface symptoms as central features of the problem [1,2].
This slow buildup matters because patients sometimes assume the problem is just the brand of lens, a temporary dry eye flare, or a bad week at work. Sometimes that is true. Sometimes it is not. Contact lens discomfort can reflect an ocular surface that no longer tolerates regular wear well. That is why refractive surgery evaluations pay close attention to tear film quality, corneal staining, ocular history, and day-to-day symptoms rather than relying on prescription numbers alone [4-6].
A memorable truth is worth stating clearly. Eyes rarely go from perfectly comfortable to intolerant in one day. Most of the time, the surface has been struggling long before the patient decides they are done with contacts.
What common triggers can push your eyes past their comfort limit?
Common triggers are often ordinary parts of modern life. Screen time lowers blink rate, which can worsen dryness symptoms. Low-humidity environments can dry the tear film on the lens surface. Age, hormonal changes, allergies, and preexisting dry eye can all make lens wear less forgiving. Even when a patient has worn contacts successfully for years, the overall balance between the lens, the tear film, and the ocular surface can change [1,2].
Long-term contact lens wear can also matter in surgical planning. One study of people undergoing corneal refractive surgery found that preoperative dry eye was common, and contact lens wear was associated with a higher risk of dry eye before surgery [4]. That does not mean lens-intolerant patients are automatically poor candidates for surgery. It means they need a careful workup and honest counselling. Dryness, lens intolerance, and surface disease should be evaluated and, when needed, treated before any refractive procedure is considered [5-7].
How can irritation affect work, workouts, travel, and confidence?
Contact lens intolerance is often dismissed as a minor convenience problem, but daily irritation can have a real quality-of-life effect. It can interrupt concentration at work, make exercise less comfortable, complicate travel, and turn simple routines into recurring hassles. A patient who constantly thinks about their lenses is not experiencing seamless vision correction. They are managing around it.
That daily burden is one reason some people start asking whether a longer-term option makes sense. The decision is not only about vision. It is about comfort, predictability, and freedom from recurring irritation. The patient personas and vision-correction attributes in the planning guide highlight this clearly, especially for active adults, heavy screen users, people with dry eye concerns, and those who value convenience, independence from corrective devices, and faster recovery timelines.
Another citation-worthy statement belongs here. The real cost of lens intolerance is not only physical discomfort. It is the way discomfort quietly takes over routine decisions.
Why do some active adults start looking for glasses-free freedom?
Many contact lens-intolerant patients are not looking for perfection. They are looking for relief. They want clear distance vision without the daily negotiation of lenses that feel worse each month. That is one reason refractive surgery continues to attract interest among motivated adults who are tired of depending on glasses or contacts [3].
SMILE has become part of that conversation because it is a flapless corneal refractive procedure used to treat myopia with or without astigmatism within FDA-cleared ranges. According to the ZEISS SMILE source material, the VISUMAX femtosecond laser is indicated for adults aged 22 or older with stable refraction over the prior year, spherical refractive error from -1.00 to -10.00 diopters, and cylinder from -0.75 to -3.00 diopters, with specific eligibility and safety requirements that must be confirmed during evaluation [8].
How does SMILE compare with ongoing dependence on contacts for the right patient?
For the right patient, the comparison is not simply surgery versus no surgery. It is also lens dependence versus lens independence. The SMILE overview materials state that the procedure is flapless and designed to correct myopia with or without astigmatism by creating and removing a lenticule through a small opening in the cornea. The same materials also state that SMILE preserves more corneal nerves than flap-based LASIK and may help reduce postoperative dry eye symptoms [8].
That dry eye question is especially important for contact lens-intolerant patients. Multiple papers report that SMILE tends to have fewer or shorter-lasting dry eye signs and symptoms than femtosecond LASIK, although postoperative dryness can still occur, and the comparison does not make SMILE risk-free [5,9-11].
At the same time, some contact lens wearers may still be better served by non-surgical measures, ocular surface treatment, or different lens strategies. Scleral lenses, for example, may help some dry eye patients, though the evidence base is still developing for use in dry eye without corneal irregularity [12].
What benefits do patients often care about most?
Patients often care about three things most: comfort, convenience, and dependable visual function. The SMILE overview pages highlight flapless treatment, quick return to daily activities, and less dependence on glasses and contacts. On page 3, the site emphasizes freedom, lifestyle, time savings, and potential long-term savings compared with ongoing contact lens and glasses costs. On page 8, it notes that most ZEISS SMILE patients achieve 20/20 vision or better, citing the U.S. FDA clinical trial [8].
The FDA clinical trial paper supports strong efficacy and safety outcomes for properly selected patients. In that trial, SMILE for myopia with astigmatism produced good visual outcomes, and the procedure has since become an established refractive option for appropriately screened adults [3,13].
A useful statement for patients is this. The best refractive procedure is not the one with the most marketing. It is the one that fits the patient’s cornea, prescription, tear film, health history, and expectations.
What risks and contraindications need honest discussion?
Every refractive procedure requires an honest risk discussion. The SMILE safety information in the source file states that the procedure is not indicated for patients with severe dry eye, unstable prescription, abnormal corneal topography, active eye infection, recent herpes eye infection, active autoimmune conditions, uncontrolled diabetes, uncontrolled glaucoma, or inadequate residual stromal bed. The same page lists possible risks such as undercorrection or overcorrection, glare, halos, starbursts, interface debris, variable healing, inflammation, and infection [8].
That is why contact lens intolerance alone is never enough to justify surgery. A patient still needs full testing, including corneal and surface evaluation, and they need realistic counselling. Refractive surgery papers and guidelines consistently emphasise individualised candidacy and careful screening because surface disease and corneal abnormalities can change the risk-benefit balance [6,7,14].
“For the right candidate, SMILE eye surgery can be a flapless way to move beyond daily contact lens frustration, but the decision should always begin with a careful medical evaluation.”
How do recovery timelines fit busy schedules?
Recovery matters because many lens-intolerant patients are balancing work, exercise, parenting, travel, and screen-heavy routines. The SMILE overview page says many patients can return to work, makeup, and exercise as soon as the next day, though actual recovery guidance depends on the surgeon’s instructions and the individual eye [8].
Published research generally supports a relatively fast recovery after SMILE, but fast does not mean identical for every patient. Dryness, visual fluctuations, and healing patterns can differ. That is why postoperative care and follow-up still matter, even when the procedure is minimally invasive [9,15].
What realistic results look like after treatment?
Realistic results mean better unaided distance vision for the right candidate, not a promise of perfection for every eye. FDA-cleared SMILE is designed to correct myopia with or without astigmatism in eligible adults, and clinical data support good accuracy and strong visual outcomes in that group [8,13,16].
At the same time, informed consent should include discussion of limits, side effects, and the possibility that not every patient will have the same visual experience or symptom course.
For contact lens-intolerant patients, the most important question is often not “Is surgery perfect?” It is “Does this option make more sense for my eyes and my life than continuing with a correction method that no longer feels workable?” That is the right question because treatment decisions should match both medical facts and daily reality.
The final takeaway is simple. When contacts used to work fine and no longer do, that change deserves attention. Sometimes the answer is better dry eye treatment. Sometimes it is a different lens strategy. And for a properly evaluated patient, sometimes SMILE becomes the more comfortable path forward [4,5,9].
References
- Valencia-Nieto L, González García MJ, López-Miguel A. A review of contact lens discomfort: from the clinic to the laboratory. J Optom. 2026 Jan-Mar;19(1):100581. doi: 10.1016/j.optom.2025.100581.
- Markoulli M, Kolanu S. Contact lens wear and dry eyes: challenges and solutions. Clin Optom (Auckl). 2017 Feb 15;9:41-48. doi: 10.2147/OPTO.S111130.
- Vance Thompson, Kayla Karpuk & Mark Packer. (2026) Preoperative ocular surface optimization and the role of lacrimal occlusion in dry eye management before cataract and refractive surgery: a critical perspective. Expert Review of Ophthalmology 21:1, pages 19-28.
- Zhao PF, Zhou YH, Hu YB, et al. Evaluation of preoperative dry eye in people undergoing corneal refractive surgery to correct myopia. Int J Ophthalmol. 2021 Jul 18;14(7):1047-1051. doi: 10.18240/ijo.2021.07.13.
- Nair S, Kaur M, Sharma N, Titiyal JS. Refractive surgery and dry eye – an update. Indian J Ophthalmol. 2023 Apr;71(4):1105-1114. doi: 10.4103/IJO.IJO_3406_22.
- Donaldson K, Parkhurst G, Saenz B, Whitley W, Williamson B, Hovanesian J. Call to action: treating dry eye disease and setting the foundation for successful surgery. J Cataract Refract Surg. 2022 May 1;48(5):623-629. doi: 10.1097/j.jcrs.0000000000000844.
- Karpecki P. et al., Dry eye diseases and ocular surgery: practical guidelines for Canadian eye care practitioners, 2017.
- Carl Zeiss Meditec Inc., ZEISS SMILE Surgery | How ZEISS SMILE Surgery Works and safety information, 2026.
- Wong AHY, Cheung RKY, Kua WN, Shih KC, Chan TCY, Wan KH. Dry eyes after SMILE. Asia Pac J Ophthalmol (Phila). 2019 Sep-Oct;8(5):397-405. doi: 10.1097/01.APO.0000580136.80338.d0.
- Cetinkaya S., Gulmez M., Comparison of SMILE and FS-LASIK procedures in terms of dry eye disease, 2019.
- Pietilä J, Huhtala A, Mäkinen P, et al. Uncorrected visual acuity, postoperative astigmatism, and dry eye symptoms are major determinants of patient satisfaction: a comparative, real-life study of femtosecond laser in situ keratomileusis and small incision lenticule extraction for myopia. Clin Ophthalmol. 2018 Sep 10;12:1741-1755. doi: 10.2147/OPTH.S172894.
- Qiu SX, Fadel D, Hui A. Scleral lenses for managing dry eye disease in the absence of corneal irregularities: what Is the current evidence? J Clin Med. 2024 Jun 29;13(13):3838. doi: 10.3390/jcm13133838.
- Dishler JG, Slade S, Seifert S, Schallhorn SC. Small-incision lenticule extraction (SMILE) for the correction of myopia with astigmatism: outcomes of the United States Food and Drug Administration premarket approval clinical trial. Ophthalmology. 2020 Aug;127(8):1020-1034. doi: 10.1016/j.ophtha.2020.01.010.
- Wierzbowska, Joanna, et al. Refractive Surgery Guidelines of the Polish Association of Ophthalmic Surgeons. Ophthalmology Journal, vol. 10, 2025, pp. 47–59. https://doi.org/10.5603/oj.105853.
- Murueta-Goyena A, Cañadas P. Visual outcomes and management after corneal refractive surgery: a review. J Optom. 2018 Apr-Jun;11(2):121-129. doi: 10.1016/j.optom.2017.09.002.
- Swaminathan U, Daigavane S. Comparative analysis of visual outcomes and complications in intraocular collamer lens, small-incision lenticule extraction, and laser-assisted in situ keratomileusis surgeries: a comprehensive review. Cureus. 2024 Apr 22;16(4):e58718. doi: 10.7759/cureus.58718.
Disclaimer: This article is for general information only and should not be taken as medical advice. Contact lens discomfort, dry eye symptoms, and suitability for SMILE eye surgery should always be assessed by a qualified optometrist or ophthalmologist. Treatment decisions depend on individual eye health, prescription stability, corneal measurements, medical history, and clinical examination.
home » blog » optical imaging »