Summary: The pancreas is an essential organ located in the abdominal cavity, with exocrine and endocrine functions that play a key role in digestion and metabolism. On one hand, it secretes enzymes that help break down proteins, carbohydrates, and fats. Also, it produces hormones such as insulin and glucagon to regulate blood glucose levels. Imbalances in these functions can lead to conditions such as diabetes and pancreatitis. Medical imaging techniques—for example, ultrasound, computed tomography (CT), magnetic resonance imaging (MRI), and endoscopic ultrasound (EUS)—offer crucial insights for both diagnosing pancreatic disorders and guiding treatment. Clinicians use these medical imaging methods to identify structural changes, detect tumours, and evaluate inflammation or blockages. Early detection through imaging supports timely interventions, improving patient outcomes. This article offers an account of pancreatic anatomy, physiology, and pathology while also examining the role of medical imaging in illuminating and treating pancreatic conditions.
Keywords: Pancreas; Insulin; Glucagon; Pancreatitis; Medical Imaging; Diagnosis.
Introduction to the Pancreas
The pancreas is a multifunctional organ that sits in the upper portion of the abdomen, just behind the stomach. It fulfils two major categories of tasks: exocrine and endocrine. Though small in size compared with the liver or large intestine, the pancreas exerts a considerable influence on multiple bodily processes by releasing enzymes for nutrient digestion and hormones for glucose control. The pancreas supports energy production, tissue maintenance, and overall bodily equilibrium through biochemical interactions within the bloodstream and digestive tract. The complexity of its structure and activities demands a thorough understanding, not only for academic study but also for clinical management of related illnesses.
Medical imaging has expanded our ability to visualise the pancreas and its internal structures in an extraordinary way. From assessing the ducts that carry digestive enzymes to evaluating the gland for any malignant or benign masses, imaging acts as a powerful gateway to understanding and intervening in pancreatic diseases. By employing modalities such as ultrasound, CT scans, MRI, and endoscopic approaches, specialists can pinpoint problems and monitor responses to treatment with far greater precision than was once possible.
Anatomy of the Pancreas
The pancreas extends roughly 15 to 20 centimetres in length, positioned across the posterior abdominal wall. It lies behind the stomach, with a head that nestles against the duodenum, a body that stretches across the midline, and a tail that tapers towards the spleen. Because of its relatively deep placement, it cannot be felt easily during a standard physical examination, making imaging techniques particularly important in detecting abnormalities.
This organ is divided into distinct regions:
- Head: The widest part, which fits into the C-shaped curve of the duodenum.
- Neck and Body: The middle sections that cross from right to left.
- Tail: The narrow end near the spleen.
A network of ducts permeates the pancreas, converging to form the main pancreatic duct (duct of Wirsung). This duct usually joins with the common bile duct before opening into the duodenum at the ampulla of Vater. There is also an accessory duct (duct of Santorini) in some individuals. Proper ductal drainage is essential for delivering exocrine secretions into the small intestine, ensuring efficient digestion.
Blood Supply and Innervation
Blood supply reaches the pancreas via branches of the splenic artery, superior pancreaticoduodenal artery, and inferior pancreaticoduodenal artery. These vessels provide oxygen and nutrients, while venous drainage primarily occurs through the splenic vein and superior mesenteric vein. These veins join to form the portal vein, which then delivers blood to the liver.
Nerve innervation includes both sympathetic and parasympathetic fibres. Sympathetic fibres usually come from the coeliac plexus and the superior mesenteric plexus, while parasympathetic input stems from the vagus nerve. These nerve pathways regulate pancreatic enzyme production and hormone secretion, fine-tuning the organ’s activities in alignment with the body’s needs.
Endocrine Function
The endocrine portion of the pancreas is contained within clusters of cells known as the islets of Langerhans. These islets comprise different cell types:
- Alpha Cells: Create glucagon, a hormone that stimulates the conversion of glycogen to glucose in the liver, boosting blood sugar levels when they drop too low.
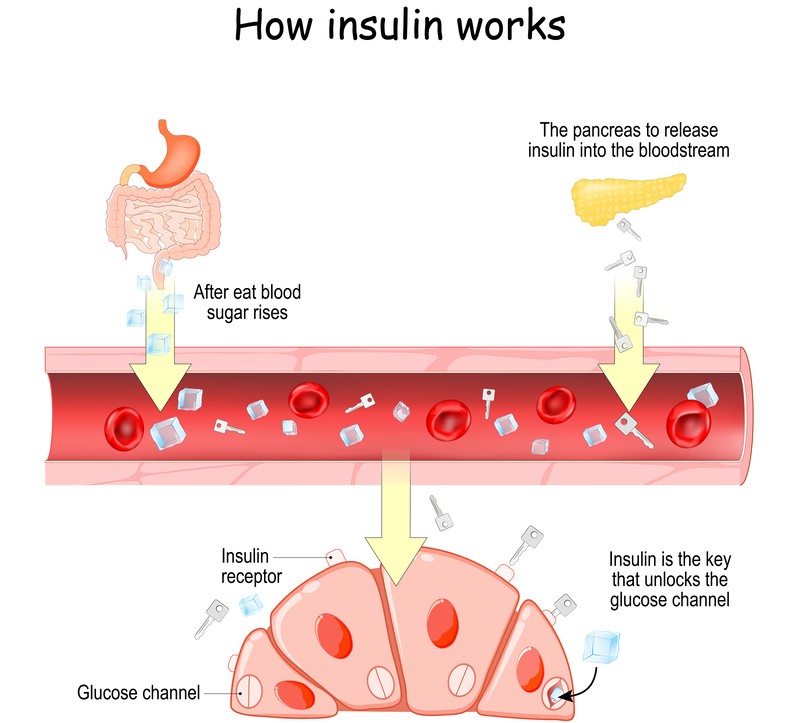
- Beta Cells: Produce insulin, lowering blood sugar levels by promoting glucose uptake into muscle, fat, and liver cells.
- Delta Cells: Generate somatostatin, which exerts a regulatory effect on both insulin and glucagon secretion, thereby maintaining a suitable balance in blood glucose.
- PP Cells (F Cells): Release pancreatic polypeptide, which governs gastrointestinal secretions and influences appetite regulation.
These hormones enter the bloodstream directly to uphold glucose homeostasis. In normal physiology, if blood sugar levels rise after a meal, beta cells increase insulin production, ensuring tissues absorb the surplus glucose. Conversely, when blood sugar drops, alpha cells escalate glucagon output. A balanced interplay between insulin and glucagon is essential for stable energy levels.
Dysregulation and Disease
When the harmony between insulin and glucagon is disturbed, conditions such as diabetes mellitus emerge. Diabetes is generally classified into two main types:
- Type 1 Diabetes: Characterised by autoimmune destruction of beta cells, leading to insufficient insulin production.
- Type 2 Diabetes: Results from insulin resistance where body tissues struggle to respond effectively to insulin, often accompanied by a gradual decline in beta cell function.
Early detection and careful management of blood glucose are paramount for preventing complications such as neuropathy, nephropathy, and retinopathy. Imaging can contribute to diagnosing structural anomalies in the pancreas that could underpin or exacerbate endocrine dysfunction, though, in the case of diabetes, diagnosis is typically based on clinical tests like blood glucose measurements.
Exocrine Function
Approximately 95% of the pancreas is dedicated to exocrine duties—synthesising digestive enzymes needed for nutrient breakdown. The exocrine tissue comprises acinar cells, which manufacture substances including:
- Amylase: Targets carbohydrates, aiding in their conversion into simpler sugars.
- Lipase: Helps digest fats, transforming triglycerides into fatty acids and glycerol.
- Proteases: Enzymes such as trypsin and chymotrypsin that break down proteins into smaller peptides and amino acids.
The synthesis of these enzymes occurs in an inactive form to guard against self-digestion. These precursors are activated only once they reach the small intestine, particularly in the duodenum. This delicate arrangement protects the pancreas from being damaged by its own enzymes.
Regulation of Enzyme Secretion
A finely tuned feedback loop involving hormones like secretin and cholecystokinin (CCK) manages the secretion of pancreatic enzymes. For example, when acidic chyme from the stomach flows into the duodenum, cells in the intestinal lining release secretin, which prompts the pancreas to produce a fluid rich in bicarbonate to neutralise the acid. CCK is triggered by the presence of fats and proteins in the intestine, stimulating the release of pancreatic enzymes to aid digestion.
Disruptions to exocrine function can manifest in conditions like chronic pancreatitis, in which scar tissue replaces healthy pancreatic tissue, limiting enzyme production and causing the malabsorption of nutrients. A thorough assessment of such conditions often depends on imaging techniques that can reveal structural alterations or obstructions in the pancreatic ducts.
Common Pancreatic Disorders
Acute pancreatitis occurs when the pancreas suddenly becomes inflamed. Gallstones or heavy alcohol use are frequent causes, but certain medications or high triglyceride levels can also trigger this condition. Typical symptoms include severe abdominal pain that can radiate to the back, nausea, and vomiting. Treatment often involves pain relief, fluid resuscitation, and sometimes procedures to remove gallstones or other obstructions.
Medical imaging is beneficial in diagnosing acute pancreatitis and determining the extent of inflammation. Ultrasound is frequently the first-line imaging method to check for gallstones or dilation of the bile ducts, while CT scanning provides more detail about the degree of pancreatic inflammation or any possible complications like necrosis or abscesses.
Chronic Pancreatitis
Chronic pancreatitis is marked by persistent inflammatory processes that bring about fibrosis and diminished functional capacity of the pancreas. Long-term alcohol use is one of the primary causes, but genetic factors and autoimmune conditions can also contribute. Patients may suffer from persistent abdominal pain, malabsorption, and weight loss.
Imaging plays a central role in diagnosing chronic pancreatitis. Calcifications visible on CT scans, irregularities in the pancreatic ducts via endoscopic retrograde cholangiopancreatography (ERCP), or changes in tissue density seen on MRI can confirm the presence and extent of chronic inflammation. Identifying these changes early can guide nutritional support, enzyme replacement therapies, and surgical interventions to mitigate complications.
Pancreatic Cancer
Tumours of the pancreas can emerge in any part of the organ but are most frequently located in the head region. Risk factors include smoking, chronic pancreatitis, obesity, and specific genetic syndromes. Symptoms such as jaundice, weight loss, and back pain may arise once the tumour enlarges or blocks the common bile duct.
Early detection is challenging because symptoms are often vague, and the pancreas is positioned deep within the abdomen. However, imaging studies are invaluable for identifying masses and assessing their extent. CT scans and MRI can detect subtle growths, gauge invasions into surrounding vessels, and help stage the disease. Endoscopic ultrasound can be employed to guide biopsies, providing tissue samples for pathological examination. Rapid diagnosis and appropriate treatment—whether surgical resection, chemotherapy, radiation therapy, or a combination—are essential for improving prognosis.
Medical Imaging and Its Role
Ultrasound, which uses high-frequency sound waves, is a non-invasive and widely accessible test that provides a preliminary overview of the pancreas and its surrounding structures. Because it does not involve ionising radiation, it is considered very safe. It can detect gallstones in the biliary tract, cystic lesions in the pancreas, and enlargement of the gland. However, its effectiveness can be restricted by the presence of gas in the intestine or by excess abdominal fat, which can limit image resolution.
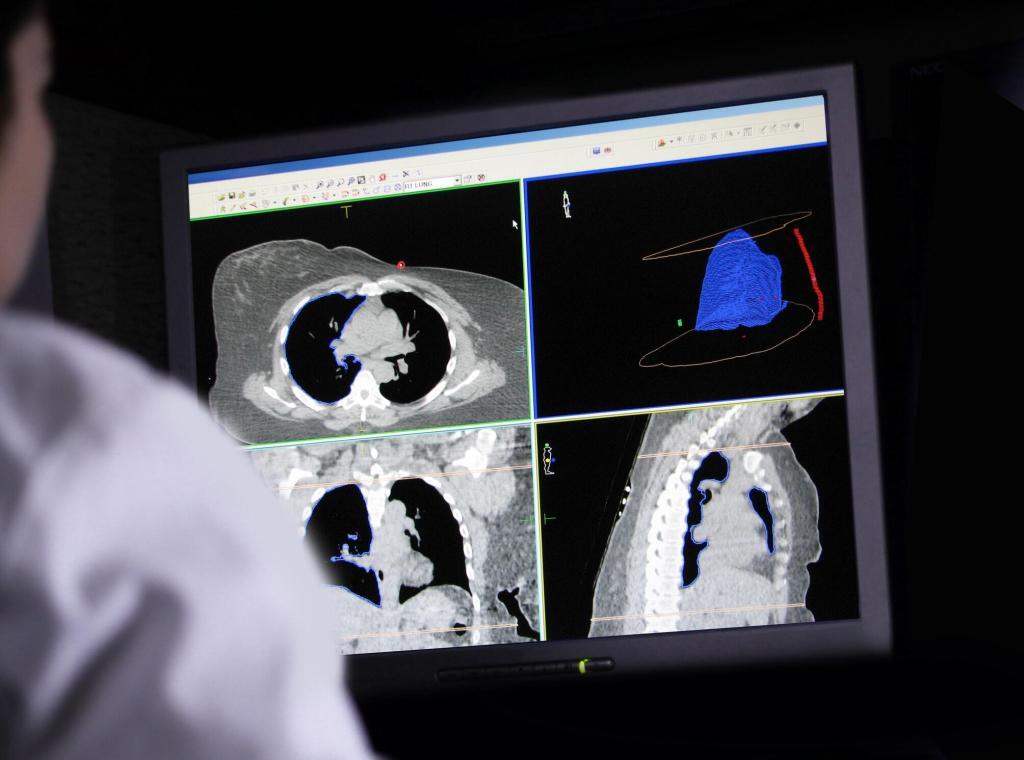
Computed Tomography (CT)
CT scanning combines X-rays with computer processing to create cross-sectional images of the abdomen. Often, a contrast medium is administered to enhance the visualisation of the pancreas and related blood vessels. CT is especially useful for diagnosing acute pancreatitis, determining the extent of chronic pancreatitis, and evaluating tumour spread. It provides a detailed three-dimensional perspective that can identify small masses and measure potential lymph node involvement.
Magnetic Resonance Imaging (MRI)
MRI uses magnetic fields and radio waves to generate high-contrast images, offering a nuanced look at soft tissues. Magnetic Resonance Cholangiopancreatography (MRCP) is a specialised MRI sequence that highlights the pancreatic and biliary ducts in great detail. It can often replace more invasive investigations like ERCP, reducing the risk of procedure-related complications. MRI is particularly beneficial for characterising cystic lesions and detecting small tumours that may go unnoticed on CT.
Endoscopic Ultrasound (EUS)
EUS merges endoscopy with ultrasound technology, using a specialised endoscope equipped with an ultrasound probe at the tip. The device is threaded through the oesophagus, stomach, and duodenum, allowing very close proximity to the pancreas. EUS produces images of exceptionally high resolution, enabling the identification of even tiny tumours or structural changes. In many cases, fine-needle aspiration (FNA) can be performed during EUS, which facilitates the collection of tissue or fluid samples for histological examination. This procedure has become a cornerstone in confirming cancer diagnoses or investigating suspicious cysts.
Positron Emission Tomography (PET)
PET scanning employs radiotracers, such as fluorodeoxyglucose (FDG), to capture metabolic activity within the pancreas. Cancer cells typically display higher metabolic rates and more FDG uptake, which can be visualised as areas of intense activity on the scan. Radiologists can correlate functional data with anatomical structures when combined with CT or MRI (forming PET-CT or PET-MRI). Though not routinely used for every pancreatic condition, PET can be particularly helpful in staging and tracking treatment effectiveness in pancreatic cancer.
Integrating Imaging Findings into Clinical Care
Because the pancreas carries out numerous activities that are intertwined with other organs—like the liver, gallbladder, and intestines—imaging must be considered in the broader context of abdominal health. For instance, a patient complaining of severe upper abdominal pain could benefit from multiple imaging modalities:
- Ultrasound: To quickly check for gallstones or significant structural anomalies.
- CT Scan: To gain detailed images of inflamed tissue in acute pancreatitis or to spot malignancies.
- MRI/MRCP: To visualise ductal irregularities or cystic lesions in the pancreas.
- Endoscopic Ultrasound: To evaluate small lesions that were inconclusive on CT or MRI, with the added advantage of sampling suspicious tissue during the same procedure.
Following this kind of systematic approach helps healthcare providers form a more precise diagnosis and design targeted treatment strategies. In pancreatitis, for instance, imaging findings might indicate complications requiring surgical intervention or suggest that a less invasive approach is sufficient. In the case of pancreatic cancer, imaging results can guide the extent of surgical resection or highlight the necessity of chemotherapy.
Future Prospects in Imaging
Technological progress in medical imaging continues at a rapid pace, enhancing both speed and image quality. Advanced CT scanners can acquire high-resolution images in mere seconds, reducing patient discomfort and motion-related artefacts. MRI innovations, such as diffusion-weighted imaging (DWI), provide subtle details on tissue composition and tumour characterisation. Meanwhile, developments in artificial intelligence (AI) and machine learning promise automated image analysis and better predictive algorithms.
These improved techniques could lead to even earlier recognition of pancreatic diseases, along with new avenues for targeted treatments. Increased precision in identifying tiny malignant lesions or subtle inflammatory changes may also result in fewer invasive procedures, cutting down on patient risk and recovery time. As imaging technologies continue to evolve, doctors may be able to detect pre-symptomatic changes in the pancreas, offering the potential for preventative measures in high-risk individuals.
Conclusion
The pancreas is one of the body’s most significant organs, regulating digestion through its exocrine secretions and balancing blood glucose through its endocrine hormones. When these functions go awry, conditions such as pancreatitis, diabetes, or cancer can develop, posing a threat to an individual’s well-being. Fortunately, modern medicine has equipped healthcare professionals with a powerful array of imaging tools that can pinpoint structural and functional abnormalities in the pancreas.
Ultrasound, CT, MRI, and endoscopic methods each provide unique yet complementary insights, enabling early detection and tailored treatment plans. With ongoing innovations in imaging technology, clinicians have an ever-growing range of capabilities for diagnosing and addressing pancreatic disorders. Looking ahead, it may be possible to identify pancreatic issues at an even earlier stage, offering patients a better chance of successful management.
By embracing imaging results and integrating them with the patient’s clinical profile and biochemical data, medical professionals can deliver interventions that improve outcomes and quality of life. In this sense, the synergy of physiology, pathology, and cutting-edge imaging stands as a prime example of how multifaceted approaches can deepen understanding and enhance patient care.
Disclaimer
This article, How the Pancreas Works: Functions and the Role of Medical Imaging, is intended for informational and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. While every effort has been made to ensure the accuracy and relevance of the information presented, Open Medscience does not guarantee that the content reflects the most current research or clinical guidelines. Readers are advised to consult qualified healthcare professionals for any medical concerns or questions regarding diagnosis, treatment options, or health conditions discussed in this article. Open Medscience assumes no responsibility for any outcomes resulting from reliance on the information contained herein.