Flashes, floaters, and a creeping ‘curtain’ can feel vague, like your eye is just tired or irritated. But when the retina starts to lift away from the back of the eye, minutes matter, and imaging is what turns a scary symptom into a clear plan. If you are the first clinician to see it, your workflow sets the pace for everyone else.
The goal is not to order every test, but to use the right tools, in the right sequence, to confirm the diagnosis, map what is happening, and hand the surgeon a picture that is actionable. In this guide, we’ll walk through a practical imaging pathway from first symptoms to surgical planning.
1. Start with symptoms
When someone reports new flashes, floaters, or a shadow in peripheral vision, suspected detachment should be treated as an urgent retina workup, and not a routine follow-up. The first imaging decision is really a triage decision: Does this patient need same-day specialist evaluation, and is the macula still on? This early distinction matters because central vision can worsen if the detachment progresses. Imaging begins only after urgency is recognised.
2. Document visual function before you dilate everything
Before drops blur the view, record the best-corrected visual acuity when possible, pinhole if needed, and confrontational fields if the patient can cooperate. Add an Amsler grid check if central distortion is reported. These basics become your baseline for counselling and for post-op comparison.
If there is a relative afferent pupillary defect, note it, as it can signal more extensive disease or concurrent pathology. Simple functional data, paired with imaging later, helps you tell the difference between something that only appears severe and something that is truly affecting vision.
3. Check the front of the eye, then confirm the picture with a dilated exam
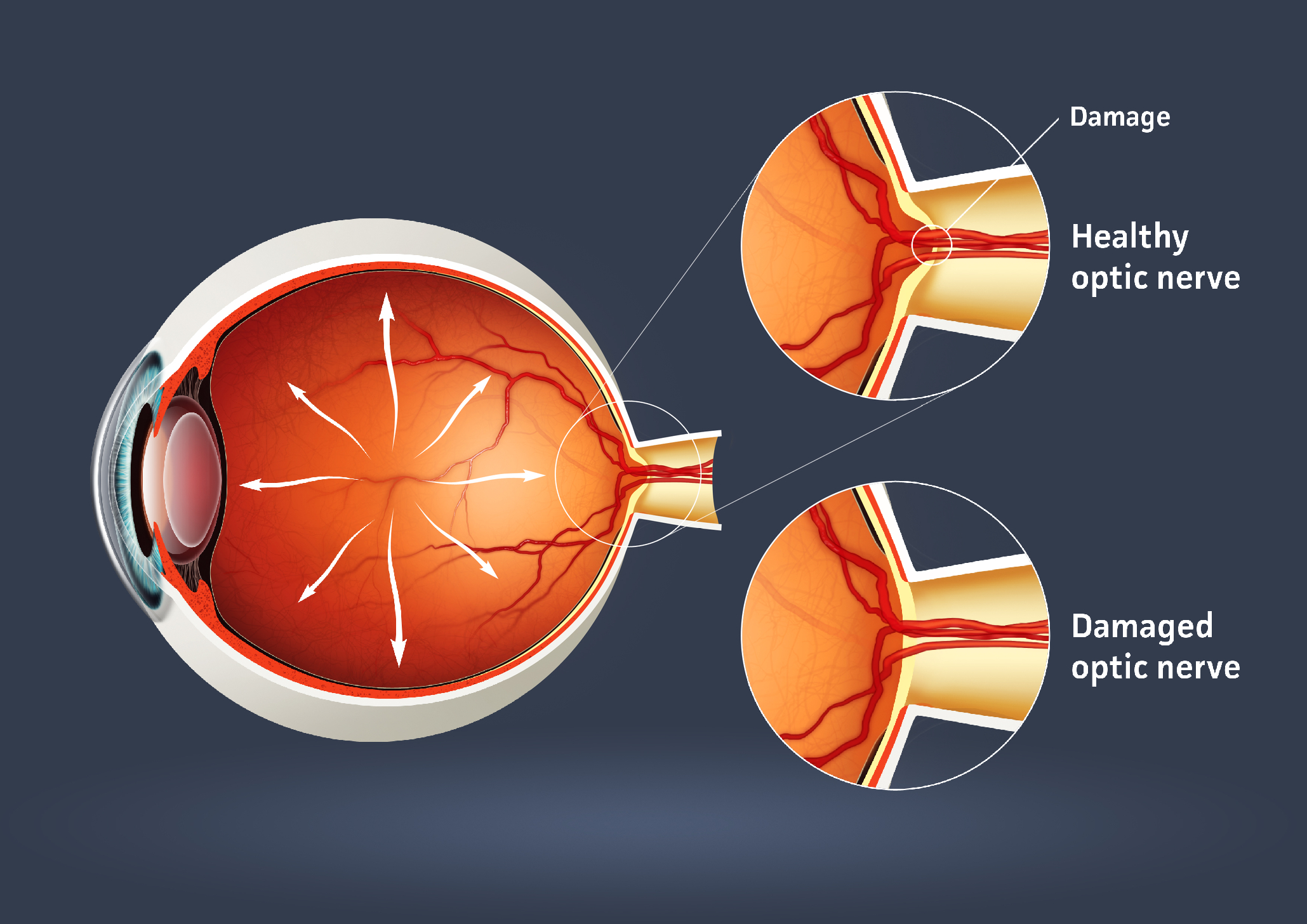
Start at the slit lamp and look for clues that point to a retinal break, not just ‘floaters.’ Pigment cells drifting in the anterior vitreous (Shafer’s sign) are a big warning. So is fresh vitreous haemorrhage, because it can hide tears and change the imaging you can rely on.
Then dilate and do a careful fundus exam; this is still the core step even in a tech-heavy workflow. Map the detachment’s edge, hunt for the primary tear, and scan the periphery for additional breaks or lattice. Use scleral depression when appropriate and tolerated, because the break that drives the whole case is often the one that sits just out of an easy view.
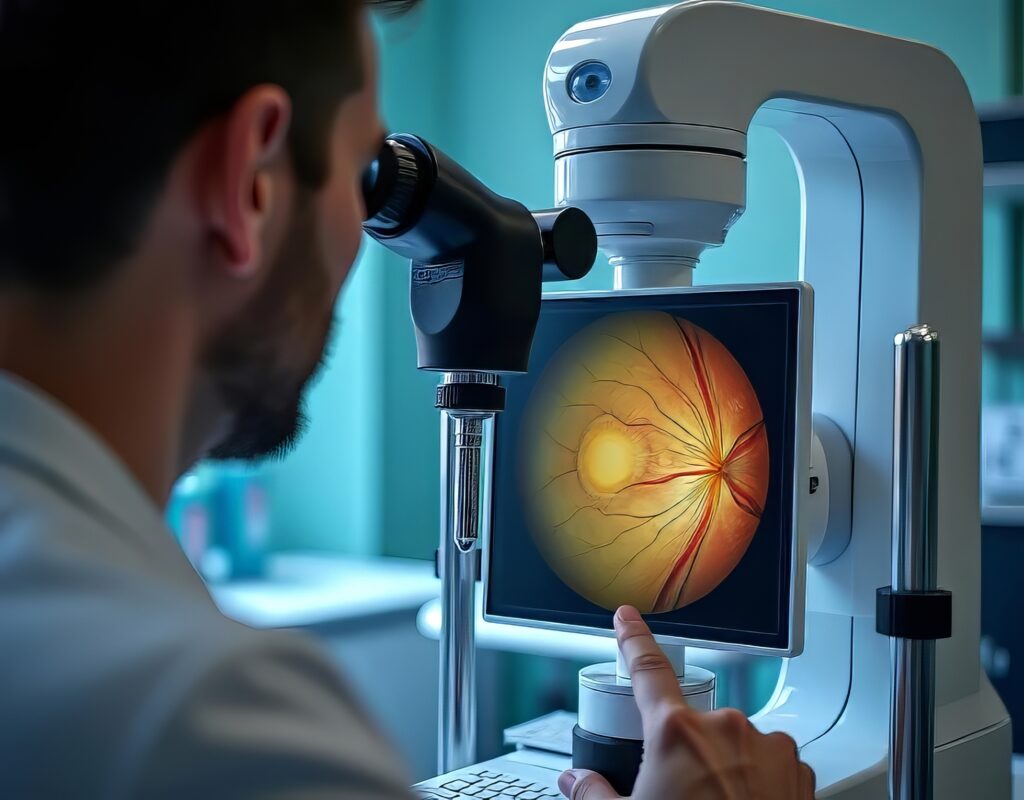
4. OCT to determine macular status and set expectations early
Optical coherence tomography (OCT) is the fastest, cleanest way to answer the macula question. Even when the clinical view is good, OCT can show subtle subfoveal fluid, early macular involvement, and the shape of the detachment at the posterior pole.
This single scan changes how urgent the case feels, how you counsel on visual prognosis, and how you stage follow-up. It also helps separate a true macula-on scenario from a ‘nearly on’ case that is one blink away.
5. Targeted imaging to locate breaks, traction, and PVR risk
Once the detachment is confirmed, the next job is finding the cause. Break localisation may be supported by scleral depression findings plus targeted photos, and in select cases by OCT at the edge of the detachment to show tractional elements or a suspicious flap. If diabetic traction is on the table, look for membranes and traction vectors, and document them because they affect whether vitrectomy is primary.
Be sure to also note signs that raise PVR risk, long-standing symptoms, large tears, multiple breaks, or inflammatory clues, since that can shift planning and tamponade choices. When the pattern is unclear, a second set of images after better dilation can be surprisingly helpful.
6. Convert imaging findings into a surgical plan
Eye surgeons do not need a hundred images; they need a tight package. Summarise macular status (on, off, or threatened), detachment extent (quadrants and posterior reach), break details (location, size, number), lens status, media clarity, and any traction or PVR features.
Attach the best widefield photos, the key OCT slice, and representative ultrasound frames if used. Then add the practical bits, symptom onset timing, anticoagulant status, positioning constraints, and whether the fellow eye has risk factors that should be checked.
Endnote
A retinal detachment workup moves best when imaging follows a simple logic: confirm, map, classify, and brief. When you keep that order, you waste fewer steps, you communicate better, and you set the surgical team up to act fast with fewer surprises.
Disclaimer: This article is for educational and informational purposes only and is not a substitute for clinical judgement, specialist ophthalmic assessment, or medical advice. Suspected retinal detachment is an urgent condition and should be assessed promptly by an appropriate eye care professional.
home » blog » optical imaging »