Summary: Multiple sclerosis (MS) is a progressive neurological condition that impairs the central nervous system, resulting in symptoms including muscle weakness, fatigue, and impaired coordination. Medical imaging techniques, particularly magnetic resonance imaging (MRI), have transformed the way clinicians recognise, track, and manage MS. Advances in imaging have enabled the identification of lesions, quantification of disease progression, and evaluation of treatment efficacy. This article examines the significance of medical imaging in the diagnosis, monitoring, and future management of multiple sclerosis (MS), highlighting the various modalities and research developments that shape patient outcomes.
Keywords: Multiple sclerosis; Magnetic resonance imaging; Neurology; Neuroinflammation; Diagnostic imaging; Lesion monitoring.
Introduction to Multiple Sclerosis (MS)
Multiple sclerosis (MS) is a chronic autoimmune disorder that affects the myelin sheath within the central nervous system (CNS). This breakdown of myelin results in impaired communication between neurons, which can then manifest as a range of neurological symptoms. Although MS can appear at any age, it is most frequently diagnosed in young adults, with women more commonly affected than men. The broad spectrum of symptoms and their variable severity underscores the complexity of MS, prompting clinicians and researchers to seek more refined methods of diagnosis and monitoring.
Due to the ever-growing impact of MS on public health, the development of improved diagnostic tools has been a longstanding priority. Medical imaging, led by MRI, has grown into an indispensable component in evaluating the progression of MS. By providing detailed insights into structural and functional changes in the brain and spinal cord, imaging has revolutionised patient care. In addition, newer imaging techniques, such as advanced MRI sequences and nuclear imaging, add another dimension to clinicians’ understanding of MS pathology.
Understanding Multiple Sclerosis
Before examining the contributions of medical imaging, it is helpful to have a clear understanding of MS itself:
Pathophysiology: MS is characterised by an immune response that triggers inflammation in the CNS. The immune system erroneously attacks the myelin sheath—a protective layer surrounding nerve fibres—leading to demyelination and the formation of sclerotic plaques (lesions). These lesions can occur anywhere in the CNS but often appear in specific white matter regions of the brain, optic nerves, and spinal cord.
Clinical Phenotypes: MS is generally categorised into distinct clinical courses: relapsing-remitting MS (RRMS), secondary progressive MS (SPMS), primary progressive MS (PPMS), and progressive-relapsing MS (PRMS). RRMS features clear relapses of neurological dysfunction, usually followed by varying degrees of recovery. Many individuals with RRMS eventually transition to SPMS, characterised by a slow accumulation of disability. PPMS involves a continual progression of symptoms with fewer distinct relapses. Understanding these clinical patterns is key to tailoring management approaches.
Symptom Range: MS symptoms are wide-ranging, reflecting the location and extent of demyelinating lesions. Frequent symptoms include numbness, muscle weakness, spasticity, fatigue, cognitive difficulties, and vision problems. The unpredictable nature of MS necessitates ongoing monitoring. Determining the precise distribution of lesions can reveal why certain symptoms arise, further justifying the significance of imaging technologies in clinical practice.
Significance of Early Diagnosis
Securing a prompt and accurate diagnosis of MS can enhance a patient’s long-term outcome by allowing earlier therapeutic intervention. Historically, diagnosis relied heavily on clinical presentation and cerebrospinal fluid (CSF) analysis for oligoclonal bands. While these methods remain relevant, imaging techniques such as MRI have become paramount in identifying lesions that may not be immediately apparent clinically.
McDonald Criteria: The evolution of the McDonald criteria reflects the increasingly central role that MRI has played in diagnosing MS. Initially introduced in 2001, these criteria have undergone periodic revision to incorporate new imaging findings. In many instances, fulfilling the McDonald criteria involves demonstrating the distribution of lesions in time and space, a task particularly suited to MRI, which can identify demyelinating areas at different points in disease progression.
Benefits of Prompt Therapeutic Intervention: Starting disease-modifying treatments earlier can slow lesion development, stabilise existing lesions, and preserve neurological function. By detecting lesions before clinical symptoms manifest, imaging assists in directing therapy to individuals most likely to benefit from an early intervention approach. Furthermore, therapy responsiveness and side effects can be monitored more accurately through regular imaging assessments.
MRI in Multiple Sclerosis
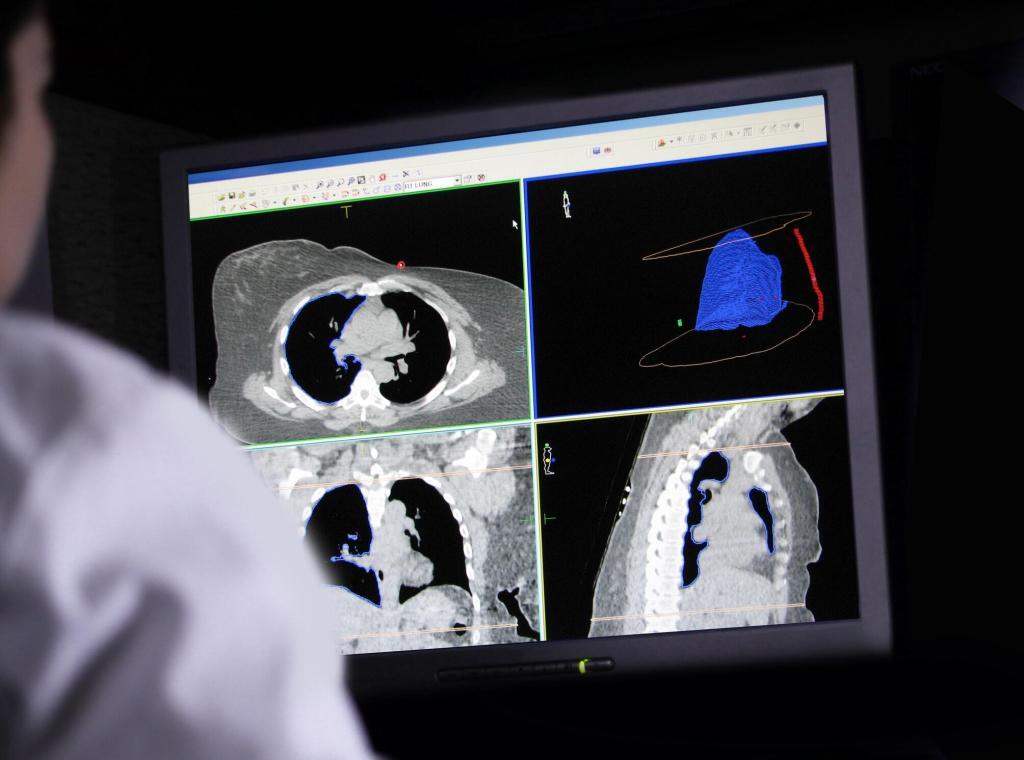
MRI stands as the gold standard in MS imaging, owing to its capacity to visualise anatomical structures of the CNS with extraordinary detail. Several MRI sequences are commonly used:
T2-Weighted Images: Highly sensitive for detecting demyelinating lesions, as lesions appear hyperintense (bright). T2-weighted imaging often reveals more lesions than are clinically evident, highlighting the subclinical activity that can drive progression.
T1-Weighted Images: Useful for identifying chronic lesions that appear hypointense (sometimes called “black holes”), possibly reflecting permanent axonal damage. When combined with gadolinium-based contrast agents, T1-weighted images can highlight active lesions, assisting in distinguishing new or inflamed areas.
FLAIR (Fluid-Attenuated Inversion Recovery): Optimised for enhancing lesion detection in areas such as the periventricular region, where MS plaques often appear. FLAIR images assist in detecting lesions that might be obscured by cerebrospinal fluid in T2-weighted images.
Advanced MRI Techniques
Beyond conventional sequences, there are advanced MRI methods that provide deeper insights into the microstructural and functional changes associated with MS:
Diffusion Tensor Imaging (DTI): Maps the diffusion of water molecules in tissue, offering information about the integrity of white matter tracts. Abnormal diffusion patterns can indicate demyelination and early axonal damage, even if conventional images look normal.
Magnetisation Transfer Imaging (MTI): Measures the transfer of magnetisation between free water and proteins, a parameter altered by demyelination. MTI can help quantify demyelination and remyelination processes in both white and grey matter.
Magnetic Resonance Spectroscopy (MRS): Provides metabolic information by quantifying specific molecules, such as N-acetyl aspartate (NAA), choline, and creatine. Changes in these metabolites can reflect neurodegeneration, inflammation, and glial activity, offering a window into biochemical processes.
Functional MRI (fMRI): Evaluates brain activity by detecting changes in blood oxygenation during tasks or at rest. Though more commonly used in research settings, fMRI can reveal adaptive or maladaptive reorganisation of brain networks in individuals with MS.
These advanced MRI techniques extend the scope of the investigation, furnishing evidence not only of lesion burden but also of how the brain responds to and compensates for demyelinating injuries over time. This is essential in shaping personalised therapy plans and evaluating neuroprotective strategies.
Additional Imaging Modalities
While CT scans have their value in various neurological investigations, they lack the sensitivity to demyelinating changes that MRI provides. CT imaging does not highlight MS lesions as accurately and is, therefore, seldom used for MS diagnosis. Nonetheless, CT may be utilised if MRI is contraindicated for certain patients, such as those with pacemakers or specific types of metal implants.
Optical Coherence Tomography (OCT)
OCT is not a CNS imaging modality but is increasingly applied to detect the thinning of the retinal nerve fibre layer in the eyes of people with MS. It offers a way to estimate neurodegenerative changes through a non-invasive eye examination. Although it does not replace MRI, OCT can be a supplementary tool to gather information on disease progression and potential axonal loss.
Nuclear Imaging: PET and SPECT
Positron emission tomography (PET) and single-photon emission computed tomography (SPECT) use radiotracers to highlight physiological or metabolic activity in the brain. Their role in MS is largely investigative, exploring inflammatory markers, demyelination, and neurodegeneration in vivo:
PET: Can employ tracers targeting activated microglia or myelin components, offering a unique perspective on inflammatory and remyelination processes.
SPECT: Although less commonly used for MS, SPECT has been explored for tracking changes in cerebral blood flow associated with inflammation and demyelination.
These nuclear imaging methods, although not currently standard clinical practice, may offer valuable insights into disease mechanisms in the future, thereby aiding the development of new therapies.
Imaging Biomarkers for Disease Monitoring
Quantifying lesion burden and new lesion formation through MRI provides a key metric for tracking the progression of MS. Gadolinium-enhancing lesions indicate areas of active inflammation, while T2 hyperintensities outline the cumulative lesion burden. By documenting changes over time, clinicians can assess the effectiveness of disease-modifying treatments (DMTs) and decide whether a therapy switch or escalation is warranted.
Brain Atrophy
Brain atrophy, encompassing both grey and white matter loss, is a hallmark of progressive pathology in MS. MRI-based volumetric measurements can detect subtle brain shrinkage early in the disease, which may correlate with clinical disability. Regularly scheduled imaging allows clinicians to pinpoint accelerated atrophy, giving them an indicator that might prompt adjustments in treatment or additional interventions to preserve neurological function.
Microstructural and Metabolic Markers
Advanced MRI approaches, such as diffusion-based methods and spectroscopic evaluations, can reveal underlying neurodegenerative processes that are not visible on conventional scans. Parameters like fractional anisotropy (FA) from DTI or metabolic ratios from MRS can serve as biomarkers for tissue integrity and inflammation. This level of information enables clinicians and researchers to anticipate future disease activity and assess the effectiveness of treatments at a cellular or metabolic level.
Future Directions
Ongoing research continues to expand the potential of medical imaging, moving closer to more individualised MS care. Several areas of investigation are especially promising:
Ultra-High-Field MRI: Scanners operating at 7 Tesla or higher provide enhanced resolution, revealing microlesions and cortical pathology that may not be evident on standard 1.5T or 3T systems. Although these high-field scanners are primarily found in research centres, their increasing availability raises the possibility of earlier and more refined assessments of structural changes in MS.
Artificial Intelligence (AI) and Machine Learning: AI-driven algorithms can accelerate the analysis of MRI data, assist with lesion segmentation, and even predict disease trajectories. By identifying patterns undetectable to human experts, AI can help clinicians tailor treatments more accurately, perhaps foreseeing relapses and optimising therapy before permanent tissue damage occurs.
Quantitative Susceptibility Mapping (QSM): QSM uses phase information from MRI to map the distribution of magnetic susceptibility sources, including iron deposition in the brain. As iron accumulation may correlate with inflammatory and neurodegenerative processes in MS, QSM could provide new biomarkers for disease severity and progression.
Biomarker Integration: In time, combining imaging data with other biomarkers, such as blood-based measurements of neurofilament light chain (NfL) or genetic profiles, may refine treatment selections. A multi-modal approach is key to deepening clinicians’ understanding of the complex interplay between inflammation, demyelination, and neurodegeneration that drives MS.
Therapeutic Monitoring and Personalisation: Future MRI sequences and radiotracers might pinpoint targeted drug delivery or enable precise mapping of remyelination therapies. By observing how the CNS responds in near real-time, clinicians could adapt or fine-tune regimens. This step towards tailored treatment strategies, underpinned by advanced imaging, holds promise for improving patients’ quality of life.
Conclusion
Medical imaging has transformed the diagnosis and management of multiple sclerosis, enabling clinicians to identify lesions early, monitor their progression, and evaluate the effectiveness of treatments in an objective manner. Conventional MRI techniques, including T2-weighted and T1-weighted imaging with contrast enhancement, have established themselves as fundamental in detecting and characterising the demyelinating lesions central to MS pathology. Meanwhile, advanced methods such as DTI, MRS, and fMRI have broadened the scope of inquiry into microstructural, metabolic, and functional changes in the CNS.
Equally important, additional imaging approaches, including OCT and nuclear imaging, are forging new paths in defining and quantifying disease activity. Although these modalities remain more exploratory, they promise to enrich the current understanding of MS and illuminate new biomarkers. Crucially, as treatments continue to evolve, imaging serves as an indispensable tool in tailoring individual patient care.
Moving forward, the integration of ultra-high-field MRI, AI-driven data analysis, and sophisticated quantitative markers stands to refine both diagnosis and management strategies in MS. As these technologies migrate from research centres to clinical settings, they will likely facilitate earlier interventions, better prediction of disease trajectories, and more successful preservation of neurological function. By adopting these advances, clinicians can offer more precise and personalised treatment, ultimately improving patient outcomes and offering hope to those affected by this complex disease.
Disclaimer
The content presented in this article is intended for informational and educational purposes only. It does not constitute medical advice, diagnosis, or treatment and should not be relied upon as a substitute for consultation with qualified healthcare professionals. While every effort has been made to ensure the accuracy of the information at the time of publication, Open Medscience makes no representations or warranties regarding the completeness, reliability, or applicability of the content for individual cases.
Any medical decisions or actions should be taken only after consulting a neurologist or other appropriate medical specialist. The views expressed in this article reflect the current understanding of medical imaging in multiple sclerosis and may evolve as new research emerges. Open Medscience does not accept any responsibility for any loss or harm arising from the use of this information.
home » blog » medicine »