This article examines the potential cancer risks associated with the administration of radionuclides in medical treatments. Radionuclides, used extensively in diagnostic imaging and therapeutic procedures, possess both beneficial and hazardous properties due to their radioactive nature. We explore the types of radionuclides commonly used, their medical applications, the biological mechanisms leading to cancer, and strategies for mitigating risk. The complex balance between the therapeutic benefits and the associated cancer risks necessitates careful consideration and adherence to stringent safety protocols.
Introduction to Radionuclides
Radionuclides are radioactive isotopes widely employed in medicine for both diagnostic and therapeutic purposes. Their application spans various fields, including oncology, cardiology, and neurology. While these radioactive substances offer significant benefits in diagnosing and treating diseases, their inherent radioactivity poses potential health risks, notably the risk of cancer. This article looks into the types of radionuclides used in medical practice, their applications, the mechanisms through which they may induce cancer, and the measures taken to minimise these risks.
Types of Radionuclides and Their Medical Applications
Radionuclides utilised in medicine can be broadly categorised into two groups: those used for diagnostic imaging and those for therapeutic purposes.
Diagnostic Radionuclides
- Technetium-99m (Tc-99m): The most widely used radionuclide in diagnostic imaging, Tc-99m, is employed in nuclear medicine scans such as bone scans, cardiac stress tests, and renal imaging.
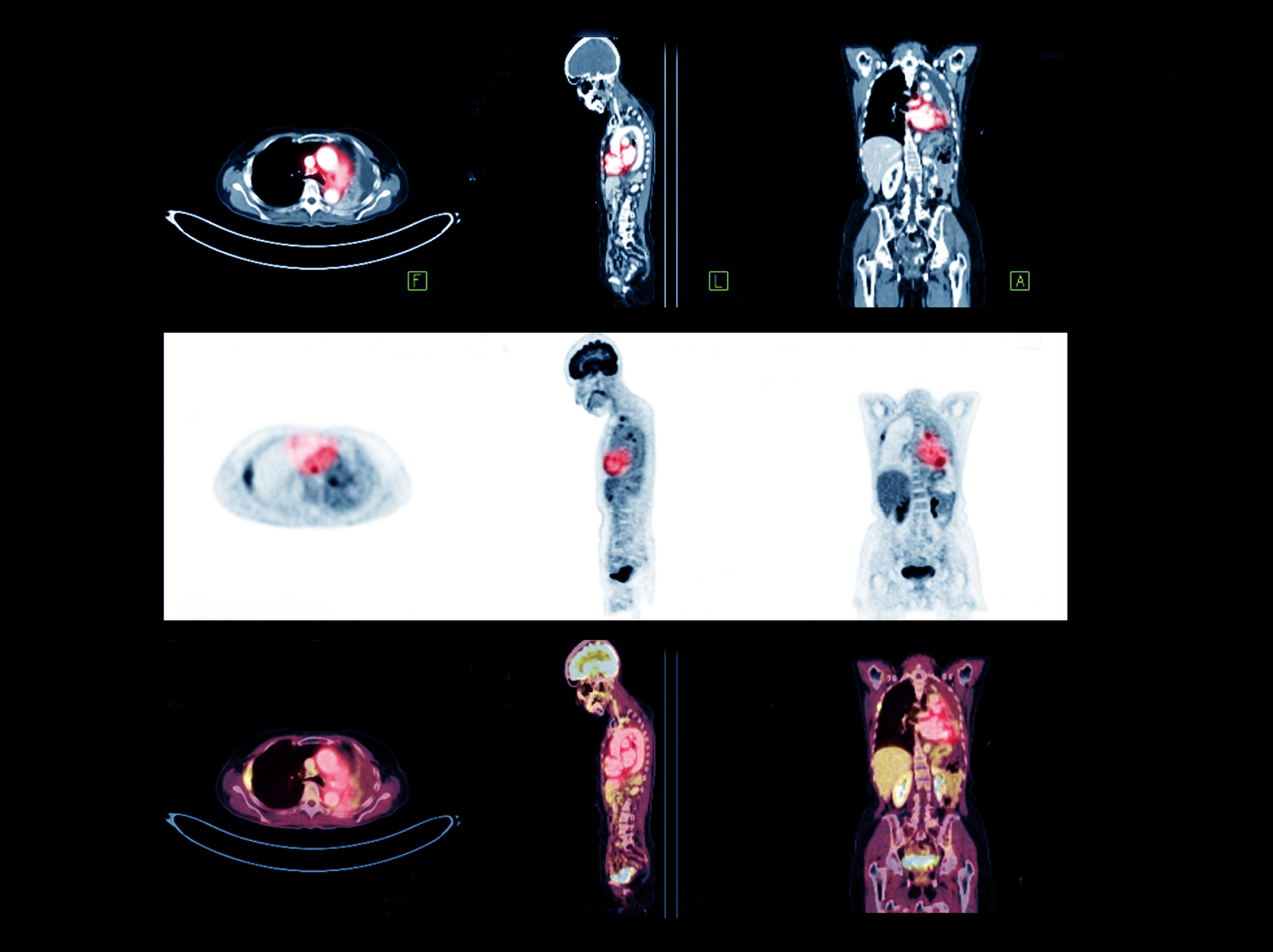
- Fluorine-18 (F-18): Used in positron emission tomography (PET) scans, F-18 helps in imaging cellular activity and is particularly useful in oncology to detect and monitor cancer.
- Iodine-123 (I-123): Employed in thyroid scans, I-123 is used to evaluate thyroid function and diagnose thyroid disorders.
Therapeutic Radionuclides
- Iodine-131 (I-131): Used in the treatment of thyroid cancer and hyperthyroidism, I-131 accumulates in the thyroid gland, delivering targeted radiation to destroy cancerous or overactive thyroid cells.
- Yttrium-90 (Y-90): Utilised in radioembolisation for liver cancer, Y-90 delivers radiation directly to tumour sites within the liver.
- Lutetium-177 (Lu-177): Applied in peptide receptor radionuclide therapy (PRRT) for treating neuroendocrine tumours, Lu-177 binds to tumour cells, delivering a lethal dose of radiation.
Biological Mechanisms Leading to Cancer
The risk of cancer from radionuclide administration stems from the ionising radiation emitted during their decay. Ionising radiation can damage cellular DNA, potentially leading to mutations and the development of cancer. The primary mechanisms through which this occurs include:
- Direct DNA Damage: Ionising radiation can directly break the DNA strands, leading to double-strand breaks, which are challenging for the cell to repair accurately. Misrepair of these breaks can result in mutations.
- Indirect DNA Damage: Radiation can ionise water molecules within cells, producing reactive oxygen species (ROS). These ROS can damage DNA, proteins, and cellular membranes, contributing to carcinogenesis.
- Bystander Effects: Cells adjacent to those directly hit by radiation can also suffer damage through intercellular signalling mechanisms, exacerbating the overall risk of mutations and cancer.
Cancer Risk Assessment
Evaluating the cancer risk associated with radionuclide administration involves several factors, including the type and dose of radionuclide, the duration of exposure, and the individual’s susceptibility. Risk assessment models, such as the linear no-threshold (LNT) model, suggest that even low doses of ionising radiation carry a risk of cancer. However, the actual risk in clinical settings depends on:
- Absorbed Dose: The amount of radiation absorbed by tissues, measured in grays (Gy), influences the extent of DNA damage.
- Dose Rate: The rate at which the radiation dose is delivered affects the biological response. High-dose rates are more likely to cause acute damage, while low-dose rates allow cellular repair mechanisms to mitigate some damage.
- Radiation Type: Alpha particles, beta particles, and gamma rays have different ionising potentials and biological impacts. Alpha particles cause dense ionisation along their path, resulting in significant local damage, whereas gamma rays have lower ionisation density but can penetrate deeper into tissues.
Mitigating Cancer Risks
Given the potential risks, several strategies are employed to minimise the likelihood of cancer from radionuclide administration:
- Optimising Dose and Exposure Time: Medical professionals carefully calculate the minimal effective dose for diagnostic and therapeutic purposes, reducing unnecessary exposure.
- Advancements in Radiopharmaceuticals: Development of radionuclides with shorter half-lives and more targeted delivery mechanisms helps minimise off-target effects and radiation exposure to non-target tissues.
- Protective Measures: Protecting and protecting equipment for patients and healthcare providers reduce exposure. Techniques such as using lead aprons and maintaining safe distances are standard practices.
- Monitoring and Follow-up: Patients receiving radionuclide therapy are closely monitored for any adverse effects, with follow-up protocols in place to detect early signs of potential complications, including secondary cancers.
Regulatory and Safety Standards
Strict regulatory frameworks govern the use of radionuclides in medicine to ensure patient safety. Organisations such as the International Atomic Energy Agency (IAEA) and national regulatory bodies set guidelines and standards for the safe handling, administration, and disposal of radioactive materials. Key regulatory measures include:
- Licensing and Training: Medical facilities and personnel handling radionuclides must be appropriately licensed and trained to adhere to safety protocols.
- Quality Control: Regular quality control checks on radiopharmaceuticals and imaging equipment ensure that doses are accurately calibrated and administered.
- Radiation Protection Programs: Comprehensive radiation protection programs within medical facilities monitor radiation exposure levels and implement safety measures to protect patients and staff.
Case Studies and Research Findings
Several studies have investigated the cancer risks associated with radionuclide therapy and diagnostic imaging. For instance, research on patients treated with I-131 for thyroid cancer has shown a slightly increased risk of secondary malignancies, particularly leukaemia, due to the high doses required for treatment. However, these risks are generally outweighed by the therapeutic benefits in managing life-threatening conditions.
Similarly, studies on diagnostic imaging, such as PET scans using F-18, indicate that the low doses used in imaging pose a minimal risk compared to the valuable diagnostic information obtained. Continuous research and long-term follow-up studies are essential to further understand the balance between the benefits and risks of radionuclide use in medicine.
Conclusion
The administration of radionuclides in medical practice offers significant diagnostic and therapeutic advantages. However, the potential risk of cancer from ionising radiation necessitates careful consideration and adherence to safety protocols. By optimising doses, employing advanced radiopharmaceuticals, and following stringent regulatory standards, the medical community can mitigate the risks while harnessing the benefits of these powerful tools. Ongoing research and vigilance in monitoring long-term outcomes are crucial in ensuring the safe and effective use of radionuclides in healthcare.
In conclusion, the balanced and judicious use of radionuclides, guided by a thorough understanding of the associated risks and benefits, is vital in modern medical practice. The continued evolution of safety measures and technological advancements will play a critical role in minimising cancer risks while maximising therapeutic efficacy.
Disclaimer
This article, “Assessing the Cancer Risk in Patients Administered Radionuclides”, is intended for informational and educational purposes only. It does not constitute medical advice, diagnosis, or treatment and should not be relied upon as a substitute for professional medical consultation. The information presented reflects the current understanding as of the publication date (29 June 2024) and may evolve with future research and clinical practice.
Open Medscience does not endorse or recommend any specific medical treatments, procedures, or radionuclide therapies mentioned in this article. Patients are strongly advised to consult qualified healthcare professionals regarding individual risks, benefits, and appropriate medical decisions.
While every effort has been made to ensure the accuracy of the information provided, Open Medscience makes no warranties or representations regarding its completeness or suitability for any particular purpose. The use of this article and reliance on any information contained herein is solely at the reader’s own risk.
home » blog » radiotheranostics »