Radiotheranostics is an emerging field combining therapeutic and diagnostic radiology that leverages particles to target and treat various diseases, particularly cancer. This overview looks into the types of particles used, their mechanisms of action, and their applications in radiotheranostics. Key topics include the types of particles (alpha, beta, gamma, and positron emitters), the principles of radiotheranostics, and the clinical applications of these technologies. The advancements and challenges in the field are also discussed, providing a holistic view of the current state and future directions of radiotheranostics.
Introduction to Radiotheranostics
Particles in radiotheranostics is a novel and rapidly evolving field that merges diagnostic imaging and therapeutic radiology to enhance the precision and efficacy of disease treatment, especially in oncology. By employing various particles, radiotheranostics allows for targeted delivery of radiation to diseased tissues while minimising exposure to healthy tissues. This dual capability of diagnosis and therapy within a single platform marks a significant advancement in personalised medicine.
Types of Particles in Radiotheranostics
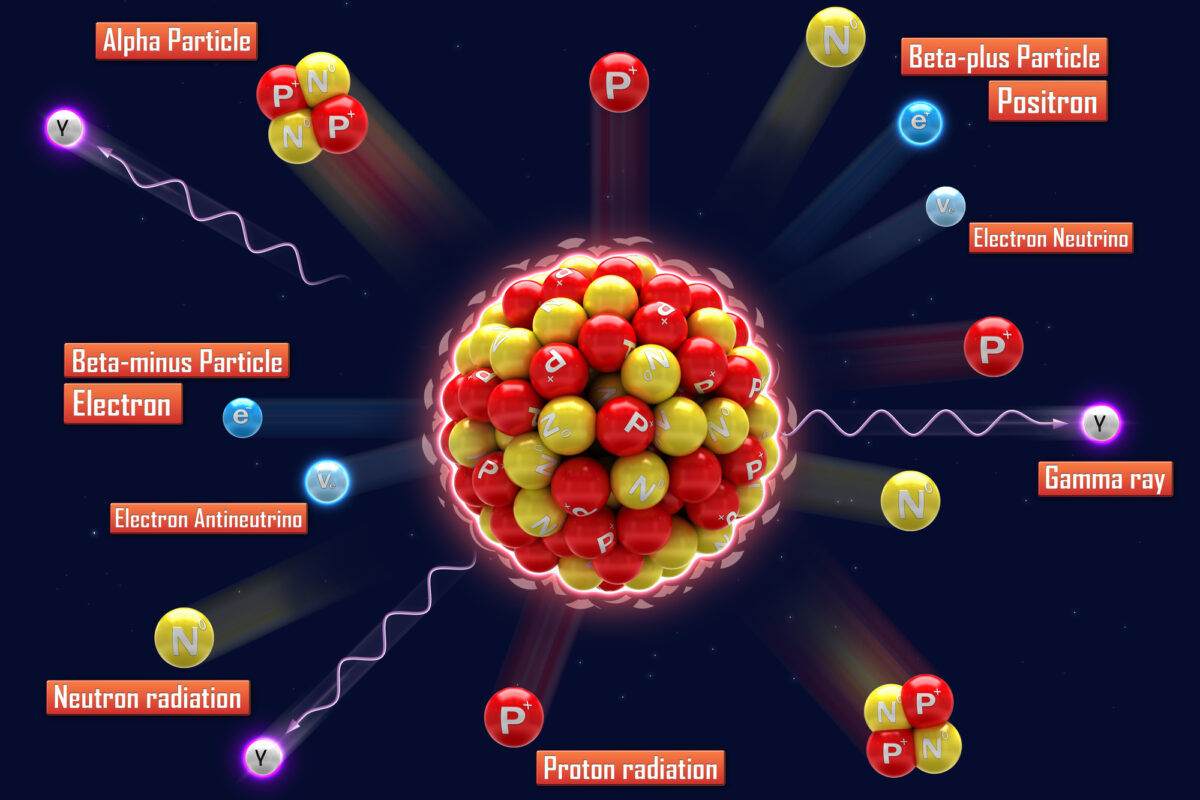
Alpha Particles
Alpha particles consist of two protons and two neutrons, making them highly ionising with limited penetration depth. Their high energy and short range are advantageous for targeting small, well-defined tumours. When alpha-emitting radionuclides are delivered to tumour cells, they induce double-strand breaks in DNA, leading to cell death. This makes alpha particles particularly effective in treating haematological cancers and micrometastases.
Beta Particles
Beta particles are high-energy, high-speed electrons or positrons. They have a greater penetration depth than alpha particles but are less ionising. Beta emitters are commonly used in radiotheranostics because they target larger tumours and disseminated disease. Examples of beta-emitting radionuclides include Iodine-131, used in thyroid cancer treatment, and Yttrium-90, used in liver cancer therapies.
Gamma Particles
Gamma particles, or photons, are electromagnetic radiation of high energy and deep penetration capabilities. While they are primarily used in diagnostic imaging due to their ability to pass through the body and provide detailed images, gamma particles are also employed in therapeutic applications. The combination of gamma emitters with therapeutic agents allows for simultaneous imaging and treatment, exemplified by the use of Technetium-99m in various diagnostic procedures.
Positron Emitters
Positron emitters release positrons that annihilate with electrons, producing pairs of gamma photons. This annihilation event is the basis of positron emission tomography (PET) imaging, a powerful diagnostic tool. Common positron emitters include Fluorine-18 and Gallium-68. In radiotheranostics, positron emitters are used for imaging and delivering therapeutic radiation when combined with specific targeting molecules.
Principles of Radiotheranostics
Particles in radiotheranostics operate on the principle of using radiolabelled compounds that specifically target disease sites. These compounds, known as radiopharmaceuticals, are designed to bind to tumour-specific antigens, receptors, or other molecular markers. The process involves several key steps:
Target Identification
Identifying appropriate targets is crucial for the success of radiotheranostics. Targets are proteins or antigens overexpressed in tumour cells but not in healthy tissues. Examples include prostate-specific membrane antigen (PSMA) in prostate cancer and somatostatin receptors in neuroendocrine tumours.
Radiopharmaceutical Development
Developing radiopharmaceuticals involves conjugating a radioactive isotope with a targeting molecule, such as an antibody, peptide, or small molecule. This conjugation ensures that the radiopharmaceutical binds specifically to the target cells, delivering radiation directly to the tumour site.
Imaging and Dosimetry
Radiotheranostics utilises imaging techniques such as PET, single-photon emission computed tomography (SPECT), and gamma camera imaging to visualise the distribution of radiopharmaceuticals in the body. This imaging provides critical information on tumour localisation, size, and metabolic activity. Dosimetry calculations are performed to determine the optimal therapeutic dose, balancing efficacy and safety.
Therapeutic Application
Once the appropriate dose is determined, the radiopharmaceutical is administered to the patient. The radiation delivered to the tumour induces DNA damage, leading to cell death and tumour regression. Continuous imaging allows for monitoring the treatment response and adjusting the therapeutic strategy as needed.
Clinical Applications of Radiotheranostics
Prostate Cancer
Prostate cancer is a leading cause of cancer-related deaths among men. Radiotheranostics has revolutionised its management by enabling precise targeting of PSMA. Radiolabelled PSMA ligands, such as Lutetium-177-PSMA-617, have shown promising results in treating metastatic castration-resistant prostate cancer, offering improved survival and quality of life.
Neuroendocrine Tumours
Neuroendocrine tumours (NETs) are a diverse group of neoplasms that often express somatostatin receptors. Radiotheranostics using radiolabelled somatostatin analogues, such as Lutetium-177-DOTATATE, have become a standard treatment for NETs. This approach allows for effective tumour control and provides valuable diagnostic information.
Thyroid Cancer
Iodine-131 has long been used in the treatment of differentiated thyroid cancer. Its ability to selectively accumulate in thyroid tissue allows for effective ablation of residual thyroid tissue and metastatic lesions. This dual diagnostic and therapeutic capability exemplifies the core principles of radiotheranostics.
Liver Cancer
Selective internal radiation therapy (SIRT) using Yttrium-90 microspheres is a well-established radiotheranostic approach for treating hepatocellular carcinoma (HCC). The microspheres deliver high-dose radiation directly to the tumour, sparing healthy liver tissue. Imaging with PET or SPECT is used to guide treatment planning and monitor response.
Advancements in Radiotheranostics
Multimodal Imaging
Integrating multiple imaging modalities, such as PET/CT and PET/MRI, enhances tumour localisation and characterisation accuracy. These advanced imaging techniques provide complementary information on tumour anatomy, metabolism, and molecular characteristics, facilitating more precise treatment planning.
Theranostic Nanoparticles
Nanotechnology is playing an increasingly important role in radiotheranostics. Theranostic nanoparticles can be engineered to carry both therapeutic and diagnostic agents, allowing for simultaneous imaging and targeted therapy. These nanoparticles can be designed to improve tumour targeting, enhance drug delivery, and reduce off-target effects.
Personalised Medicine
Particles in radiotheranostics embodies personalised medicine principles by tailoring treatment to the individual characteristics of each patient’s tumour. Advances in genomics, proteomics, and molecular biology are enabling the development of highly specific radiopharmaceuticals that target unique tumour markers, paving the way for more effective and personalised therapies.
Radioimmunotherapy
Combining radiotheranostics with immunotherapy is an emerging strategy to enhance the anti-tumour immune response. Radioimmunotherapy involves using radiolabelled antibodies that target tumour-associated antigens, delivering radiation to the tumour while stimulating the immune system. This approach holds promise for improving the efficacy of cancer immunotherapy.
Challenges in Radiotheranostics
Radiation Safety
Ensuring the safety of patients and healthcare workers is a paramount concern in radiotheranostics. The handling and administration of radioactive materials require strict adherence to radiation safety protocols to minimise exposure and prevent contamination.
Regulatory and Ethical Considerations
The development and approval of radiopharmaceuticals involve rigorous regulatory processes to ensure their safety, efficacy, and quality. Ethical considerations, such as informed consent and the potential long-term effects of radiation exposure, must also be addressed in clinical trials and practice.
Cost and Accessibility
The high cost of radiopharmaceuticals and the specialised infrastructure required for their production and administration can limit access to radiotheranostic treatments. Efforts to reduce costs and improve accessibility are essential to ensure that patients can benefit from these advanced therapies.
Technological and Logistical Challenges
The production, storage, and transport of radiopharmaceuticals pose significant logistical challenges. The short half-life of many radionuclides necessitates efficient coordination to ensure timely delivery and administration. Advances in radiochemistry and logistics are needed to overcome these challenges.
Future Directions in Radiotheranostics
Development of New Radiopharmaceuticals
Ongoing research is focused on developing new radiopharmaceuticals that target a wider range of tumour markers. Novel radionuclides and targeting molecules are being explored to expand the therapeutic options available in radiotheranostics.
Combination Therapies
Combining radiotheranostics with other treatment modalities, such as chemotherapy, immunotherapy, and targeted therapy, is an area of active investigation. These combination approaches aim to enhance treatment efficacy, overcome resistance, and improve patient outcomes.
Artificial Intelligence and Machine Learning
The application of artificial intelligence (AI) and machine learning in radiotheranostics holds great potential for improving treatment planning, imaging interpretation, and patient management. AI algorithms can analyse large datasets to identify patterns and optimise therapeutic strategies, leading to more personalised and effective treatments.
Global Collaboration and Standardisation
International collaboration and standardisation are crucial for advancing the field of radiotheranostics. Collaborative efforts among researchers, clinicians, and regulatory bodies can facilitate the development and implementation of best practices, ensuring the safe and effective use of radiotheranostic technologies worldwide.
Key Areas for Future Research and Development
Enhanced Targeting Strategies
Improving the specificity and affinity of radiopharmaceuticals for tumour cells is a critical area of research. Advances in molecular biology and bioengineering enable the design of novel targeting agents that selectively bind to tumour-specific markers, thereby increasing the therapeutic index of radiotheranostic agents. This includes the development of bispecific antibodies, peptides, and aptamers that can recognise multiple targets on tumour cells.
Optimising Dosimetry
Accurate dosimetry is essential for maximising the therapeutic efficacy of radiotheranostics while minimising toxicity to healthy tissues. Advanced computational models and imaging techniques are being developed to improve dose estimation and distribution. Personalised dosimetry, which tailors the radiation dose to the individual patient’s tumour characteristics and biodistribution of the radiopharmaceutical, is an emerging approach that holds promise for enhancing treatment outcomes.
Radiotheranostics in Non-Oncological Applications
While the primary focus of radiotheranostics has been on oncology, there is growing interest in exploring its applications in other medical fields. For example, radiotheranostic approaches are being investigated for the treatment of cardiovascular diseases, infections, and neurological disorders. The ability to deliver targeted radiation to specific tissues opens new avenues for the treatment of a wide range of conditions.
Integration with Other Modalities
The integration of radiotheranostics with other therapeutic modalities, such as photodynamic therapy, hyperthermia, and gene therapy, is an area of active research. These combination therapies have the potential to enhance the therapeutic effects of radiotheranostics and overcome resistance mechanisms. For instance, combining radiotheranostics with hyperthermia can increase tumour sensitivity to radiation, while gene therapy can be used to enhance the expression of radiation-sensitive genes in tumour cells.
Clinical Trials and Translation to Practice
Translating radiotheranostic innovations from the laboratory to clinical practice involves rigorous testing through clinical trials. These trials are designed to evaluate the safety, efficacy, and optimal dosing of new radiopharmaceuticals and treatment protocols. Key considerations in the design of radiotheranostic clinical trials include patient selection, endpoint definition, and the use of imaging biomarkers to monitor treatment response.
Early-Phase Trials
Early-phase clinical trials (Phase I and II) focus on assessing new radiopharmaceuticals’ safety, biodistribution, and preliminary efficacy. These trials involve a small number of patients and aim to identify the optimal dose and administration schedule. Imaging studies are often included to visualise the distribution of the radiopharmaceutical and assess tumour uptake.
Late-Phase Trials
Late-phase clinical trials (Phase III) involve larger patient populations and aim to confirm the efficacy and safety of the radiopharmaceutical in comparison to standard treatments. These trials provide the evidence needed for regulatory approval and incorporation into clinical practice guidelines. The design of late-phase trials is critical for demonstrating the clinical benefit and cost-effectiveness of radiotheranostic approaches.
Post-Market Surveillance
Once a radiopharmaceutical is approved and enters clinical practice, ongoing surveillance is essential to monitor its long-term safety and effectiveness. Post-market studies and registries collect real-world data on the use of radiotheranostics, providing valuable insights into patient outcomes, rare adverse events, and the impact of treatment on quality of life.
Education and Training
The successful implementation of radiotheranostics in clinical practice requires comprehensive education and training for healthcare professionals. This includes training in the principles of radiopharmacy, imaging techniques, radiation safety, and the clinical management of patients undergoing radiotheranostic treatments.
Radiopharmacy and Imaging
Radiopharmacists and nuclear medicine technologists play a crucial role in preparing, quality control, and administering radiopharmaceuticals. Specialised training programmes are needed to equip these professionals with the skills to safely and effectively handle and dispense radioactive materials. Similarly, radiologists and nuclear medicine physicians must be trained in advanced imaging techniques and the interpretation of radiotheranostic scans.
Clinical Management
Oncologists, radiation oncologists, and other healthcare providers involved in the care of patients receiving radiotheranostic treatments must be familiar with these therapies’ unique aspects. This includes understanding the mechanisms of action, potential side effects, and strategies for optimising treatment outcomes. Multidisciplinary collaboration is essential to ensure that patients receive comprehensive and coordinated care.
Patient Education
Educating patients about radiotheranostic treatments is also important for ensuring informed decision-making and adherence to treatment protocols. Patients should be provided with clear and understandable information about the benefits, risks, and expectations of radiotheranostic therapy. Effective communication can help alleviate anxiety and improve patient satisfaction.
Conclusion
Particles in radiotheranostics represent a transformative approach to diagnosing and treating cancer and other diseases, offering the potential for highly targeted and personalised therapies. The integration of diagnostic imaging and targeted radiotherapy within a single platform enables precise localisation and treatment of diseased tissues, improving therapeutic outcomes and reducing side effects.
Ongoing research and development are focused on enhancing the specificity and efficacy of radiopharmaceuticals, optimising dosimetry, and expanding the applications of radiotheranostics beyond oncology. Advances in imaging techniques, nanotechnology, and personalised medicine are driving the field forward, offering new possibilities for patient care.
The successful translation of radiotheranostic innovations into clinical practice requires robust clinical trials, regulatory approval, and comprehensive education and training for healthcare professionals. By addressing the challenges and leveraging the opportunities in this field, radiotheranostics can revolutionise how we diagnose and treat a wide range of diseases, ultimately improving patient outcomes and quality of life.
As the field continues to evolve, collaboration among researchers, clinicians, and regulatory bodies will be essential to ensure the safe and effective use of radiotheranostic technologies. With continued investment in research, education, and infrastructure, radiotheranostics is poised to become a cornerstone of personalised medicine, offering new hope for patients worldwide.
Disclaimer
The content provided in this article, Particles in Radiotheranostics for Precision Medicine, published by Open Medscience on 22 June 2024, is intended for informational and educational purposes only. It does not constitute medical advice, diagnosis, or treatment, and should not be relied upon as such. Readers should consult qualified healthcare professionals before making decisions related to their health or treatment options.
While every effort has been made to ensure the accuracy and reliability of the information at the time of publication, Open Medscience makes no representations or warranties of any kind, express or implied, about the completeness, accuracy, or suitability of the information contained herein. Any reliance placed on such information is strictly at the reader’s own risk.
The article may reference experimental treatments, emerging technologies, and ongoing clinical trials that may not be approved for routine clinical use. Regulatory statuses and clinical practices may vary by region and are subject to change.
Open Medscience, its contributors, and affiliated parties accept no liability for any loss, injury, or damage resulting from the use of this content or the application of any of the information provided.
home » blog » radiotheranostics »