Robotic surgery represents a significant advancement in medical technology, offering unprecedented precision, flexibility, and control. This article outlines the origins of robotic surgery, its development over the years, the various types available, and its benefits and challenges.
Introduction to Robotic Surgery in Modern Healthcare
Robotic surgery is a groundbreaking innovation in medical science, significantly transforming the landscape of surgical procedures worldwide. This advanced technology merges the precision of robotic systems with the expertise of surgeons, enabling the performance of complex surgeries with unparalleled accuracy and minimal invasiveness. The emergence of robotic surgery marks a pivotal shift in healthcare, promising enhanced surgical outcomes and redefining the interaction between technology and human dexterity within the medical arena.
The inception of robotic surgery can be traced back to the late 20th century, with its roots deeply embedded in the desire to improve surgical outcomes and patient safety. The traditional approach to surgery, often requiring large incisions and manual manipulation of instruments, posed significant risks, including excessive blood loss, infection, and prolonged recovery times. The advent of robotic surgery has addressed these challenges head-on, offering a minimally invasive alternative that significantly reduces the physical trauma inflicted on the patient’s body, thereby facilitating quicker recovery and less postoperative pain.
At the core of robotic surgery is the integration of advanced robotic systems, high-definition 3D imaging, and sophisticated software that allows surgeons to operate with extraordinary precision. These robotic systems are designed to replicate the surgeon’s movements in real-time, translating them into precise actions by miniaturised surgical instruments. Unlike conventional surgery, where the surgeon’s direct manual control and visibility are limited, robotic surgery enhances these aspects by providing a magnified, three-dimensional view of the surgical site and instruments that can rotate and bend far beyond the natural capability of the human hand. This technological prowess enables surgeons to perform intricate procedures through tiny incisions, reaching areas that were previously deemed inaccessible with traditional methods.
The integration of robotics in surgery is a testament to technological advancement and highlights the crucial role of human skill and intelligence in orchestrating these complex procedures. Surgeons undergo rigorous training to master the operation of robotic systems, ensuring that the fusion of technology and human expertise achieves the best possible outcomes for patients. This collaboration between humans and machines opens new horizons in surgical practices, allowing for operations that were once considered too risky or impossible to be performed with increased safety and success rates.
Furthermore, the advent of robotic surgery represents a significant step forward in personalised healthcare. By allowing for greater precision, robotic surgery enables tailor-made procedures adapted to each patient’s specific anatomical and physiological characteristics. This bespoke approach optimises surgical outcomes and aligns with the broader vision of healthcare, which prioritises patient-centred care and the minimisation of risk.
The Origins of Robotic Surgery
The origins of robotic surgery trace back to a period of burgeoning interest in combining technological innovation with medical practice, aiming to enhance surgical precision and patient outcomes. This fascinating journey began in earnest in the mid-1980s, marking the inception of an era that would eventually revolutionise the field of surgery.
The pioneering milestone in the evolution of robotic surgery was the development of the PUMA 560, a robotic arm initially designed for industrial applications that found its way into the operating theatre. In 1985, the PUMA 560 was used to perform a neurosurgical biopsy with remarkable precision, representing the first known use of a robot in a surgical context. This groundbreaking procedure demonstrated the potential for robotic technology to assist in highly delicate surgical operations, setting the stage for the development of more advanced robotic systems specifically designed for medical purposes.
Following the success of the PUMA 560, the late 1990s witnessed the advent of the da Vinci Surgical System, a pivotal development that would significantly shape the future of robotic surgery. The da Vinci System, named in honour of the renowned Renaissance artist and inventor Leonardo da Vinci, who had a keen interest in human anatomy, was the first robotic system to be approved by the U.S. Food and Drug Administration (FDA) for general laparoscopic surgery. Its introduction heralded a new era in minimally invasive surgery, offering enhanced precision, control, and flexibility beyond what was possible with conventional techniques.
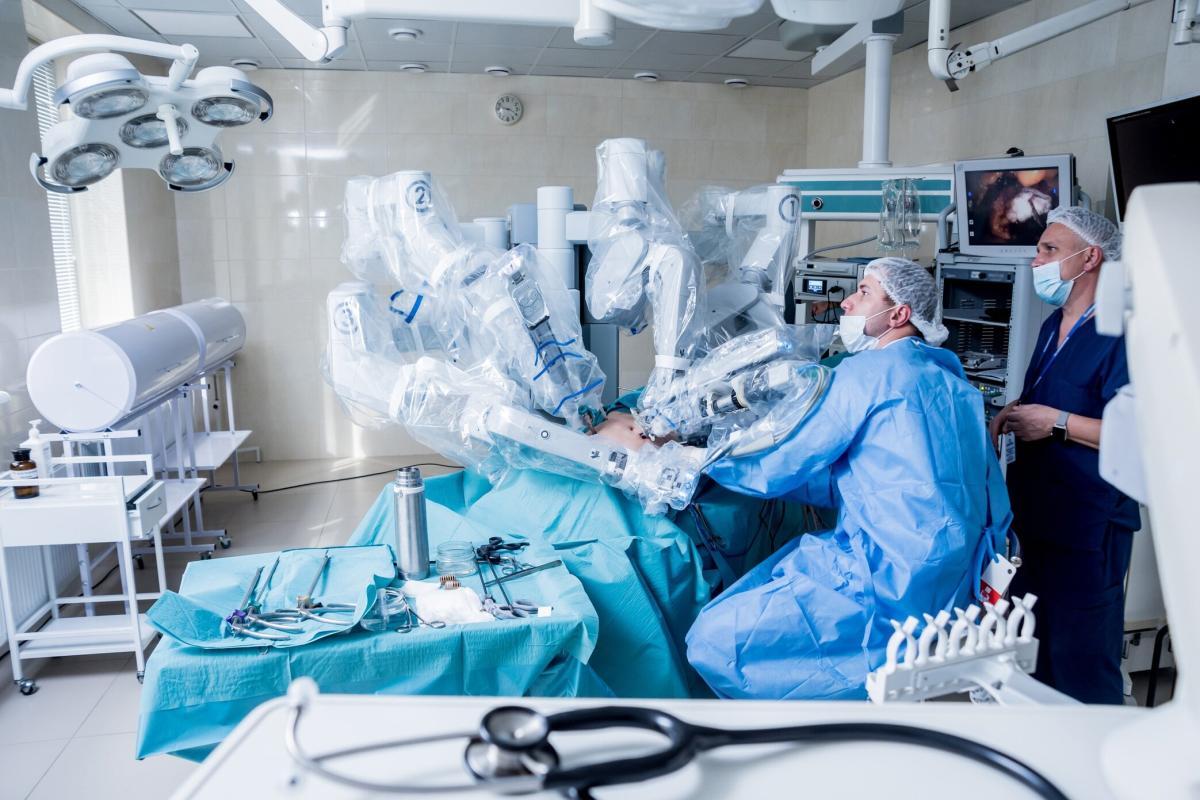
The da Vinci Surgical System consists of a surgeon-operated console, a patient-side cart with robotic arms, a high-resolution 3D vision system, and specialised instruments. The surgeon controls the system from the console, viewing a magnified, three-dimensional image of the surgical site while manipulating the instruments, which translates the surgeon’s hand movements into precise movements of the robotic arms and tools. This innovative approach allows for surgical procedures to be performed through tiny incisions, reducing patient recovery time, pain, and the risk of infection compared to traditional open surgery.
The success of the da Vinci Surgical System sparked a wave of innovation in robotic surgery, leading to the development of a variety of robotic systems tailored to different types of surgical procedures. These systems have continually evolved, incorporating advanced features such as enhanced 3D visualisation, greater dexterity and range of motion, and even haptic feedback, providing the surgeon with tactile information about the forces applied during surgery.
The origins of robotic surgery are not merely a story of technological achievement; they also reflect a deep-seated ambition to push the boundaries of medical science for the betterment of patient care. The pioneering efforts of the developers of the PUMA 560 and the da Vinci Surgical System laid the foundation for a rapidly expanding field driven by the promise of safer, more effective, and less invasive surgical treatments.
Today, as we look back on the origins of robotic surgery, it is clear that the integration of robotics into surgical practice has not only transformed the way surgeries are performed but also significantly improved the quality of life for countless patients worldwide. The journey from the PUMA 560 to the da Vinci Surgical System and beyond symbolises the remarkable potential of combining human ingenuity with technological innovation to advance healthcare, embodying a continuous quest for excellence in the pursuit of healing.
Types of Robotic Surgery Systems
In the sphere of medical technology, robotic surgery systems stand out as a beacon of innovation, offering new levels of precision, flexibility, and efficiency in surgical procedures. These systems, varying widely in their design, capabilities, and areas of application, have become instrumental in advancing surgical practices across various medical disciplines. Among the multitude of robotic surgery systems available, three systems have gained particular prominence: the da Vinci Surgical System, the Mako Robotic-Arm Assisted Technology, and the Senhance Surgical System. Each of these systems has its unique features and specialised applications, reflecting the diversity and potential of robotic assistance in surgery.
The da Vinci Surgical System
The da Vinci Surgical System is perhaps the most recognised and widely used robotic surgery system globally. Introduced in the late 1990s, it marked a significant milestone in the field of minimally invasive surgery. The system consists of a surgeon-operated console, a patient-side cart with four interactive robotic arms, a high-definition 3D vision system, and EndoWrist instruments that mimic the movements of the human hand with enhanced precision and range of motion. The da Vinci Surgical System is primarily used in urology, gynaecology, and general surgery for procedures such as prostatectomies, hysterectomies, and colorectal surgeries. Its ability to perform complex surgeries through tiny incisions has led to reduced patient recovery times, less postoperative pain, and decreased risk of complications, revolutionising the surgical experience for both surgeons and patients.
The Mako Robotic-Arm Assisted Technology
Specialising in orthopaedic surgery, the Mako Robotic-Arm Assisted Technology has transformed the way knee and hip replacements are performed. Developed to enhance the precision and accuracy of joint replacement surgeries, the Mako system combines pre-operative planning features and real-time intra-operative visualisation with a robotic arm that assists the surgeon in preparing the bone cavity and positioning the implant with unparalleled accuracy. This technology allows for a customised surgical experience tailored to the individual patient’s anatomy, leading to better alignment and fit of implants, improving the longevity of joint replacements and resulting in better functional outcomes for patients. The Mako system represents a significant advancement in orthopaedic surgery, offering a higher level of precision and predictability in procedures that are critical to improving patients’ quality of life.
The Senhance Surgical System
The Senhance Surgical System is notable for its incorporation of haptic feedback, a feature that represents a significant technological advancement in the field of robotic surgery. Haptic feedback allows surgeons to feel tactile sensations that replicate the resistance offered by tissues during surgery, providing an additional layer of sensory input that enhances the surgeon’s control and precision. This system is designed for general use in gynaecological and colorectal surgery. The Senhance system also boasts features such as eye-tracking camera control, which allows the surgeon to change the visual field on the monitor simply by moving their eyes, and ergonomically designed consoles that reduce physical strain on the surgeon during extended procedures. The introduction of haptic feedback in robotic surgery through the Senhance System has opened new avenues for surgical innovation, offering a more immersive and intuitive surgical experience.
These robotic surgery systems have profoundly impacted the field of surgery, and each system has a unique set of capabilities and applications, underscoring the vast potential of robotic assistance in enhancing surgical precision, improving patient outcomes, and advancing the frontiers of medical science. As technology continues to evolve, these systems will undoubtedly play a pivotal role in shaping the future of surgery, heralding a new era of minimally invasive procedures that offer benefits to patients and healthcare providers alike. The diversity and sophistication of robotic surgery systems exemplify the remarkable strides made in integrating technology with healthcare, promising an exciting future for surgical innovation and patient care.
Advantages of Robotic Surgery
Robotic surgery, the apex of technological advancement in the medical field, has ushered in a new era of surgical precision and patient care. Integrating robotics into surgical practices offers many advantages over traditional surgical methods, significantly improving outcomes and enhancing the overall patient experience. Among the foremost benefits of robotic surgery are its enhanced precision, minimally invasive nature, and improved access to challenging anatomical areas, each contributing to its growing adoption across various surgical disciplines.
Enhanced Precision
One of the most lauded benefits of robotic surgery is its unparalleled precision. Robotic systems are equipped with high-definition, three-dimensional vision systems that provide surgeons with a detailed view of the surgical site, surpassing the clarity and depth perception possible with the human eye alone. This is coupled with instruments designed to bend and rotate with a degree of dexterity far beyond the natural capabilities of the human hand. Such precision is critical when operating on delicate structures and confined spaces, reducing the margin for error and enhancing the likelihood of successful outcomes. The precision of robotic systems minimises tissue trauma, leading to more precise dissection and suture placement, which are vital for the patient’s recovery and the long-term success of the surgery.
Minimally Invasive
Robotic surgery is inherently minimally invasive, primarily performed through small incisions that significantly lessen the physical impact on the patient compared to traditional open surgery. This minimally invasive approach reduces the risk of infection, a common concern associated with more extensive surgical wounds. Moreover, patients often experience considerably less postoperative pain, as the smaller incisions and reduced tissue disruption inherent to robotic surgery lessen the body’s pain response. Consequently, this contributes to shorter hospital stays and faster recovery times, allowing patients to return to their daily activities more quickly. The minimally invasive nature of robotic surgery benefits patient well-being and represents a more cost-effective approach to healthcare by reducing the length of hospitalisation and the need for postoperative care.
Improved Access
Robotic surgery extends the capabilities of surgeons by enabling operations in tight spaces within the human body that would be challenging or outright impossible to navigate with traditional instruments. The articulated instruments of robotic systems can reach difficult-to-access areas, performing intricate manoeuvres that enhance the surgeon’s ability to treat complex conditions effectively. This improved access is particularly beneficial in surgeries requiring precision within confined or complex anatomical regions, such as the pelvis or thorax. By expanding the range of procedures that can be performed minimally invasively, robotic surgery opens new avenues for treating conditions that previously necessitated more invasive approaches, further reducing patient trauma and improving surgical outcomes.
The advantages of robotic surgery, from enhanced precision and minimally invasive techniques to improved access to challenging anatomical areas, underscore its transformative impact on modern surgical practices. These benefits lead to better surgical outcomes and quicker recoveries for patients and signify a leap forward in the evolution of surgery. As technology continues to advance, the potential for robotic surgery to further refine and expand its advantages grows, promising a future where surgical interventions are safer, more efficient, and more accessible to patients worldwide.
Challenges and Considerations
While robotic surgery represents a significant leap forward in medical technology, offering numerous advantages over traditional surgical methods, it is not without its challenges and considerations. These obstacles underscore the complexity of integrating advanced robotics into the healthcare system and highlight areas where further development and adaptation are needed.
High Costs
One of the most formidable challenges facing the adoption of robotic surgery is the high costs associated with these systems. The initial investment required to purchase a robotic surgery system can run into millions of pounds, putting it out of reach for many healthcare facilities, especially those in developing countries or under-resourced regions. In addition to the purchase price, there are ongoing expenses related to maintenance, repairs, and the replacement of specialised instruments and parts. These financial considerations can significantly impact a hospital’s budget and resources, making it difficult for many institutions to justify the investment despite the potential long-term benefits of robotic surgery, such as reduced hospital stay times and lower complication rates.
Learning Curve
The implementation of robotic surgery systems also presents a steep learning curve for surgeons and surgical teams. Operating these complex machines requires extensive training and practice to master. Surgeons must become proficient in controlling the robotic arms and instruments and interpreting the three-dimensional images provided by the system. This process can be time-consuming and requires significant training and skill development investment. While the effort can lead to improved surgical outcomes, the initial phase of adaptation can be challenging and may temporarily affect the efficiency of surgical operations.
Technical Limitations
Although advanced technology underpins robotic surgery systems, technical limitations still need to be addressed. For example, some models lack tactile or haptic feedback, meaning surgeons do not receive direct physical sensations from the surgical instruments. This absence of tactile information can make it difficult for surgeons to gauge the force they are applying to tissues, potentially affecting their ability to perform certain delicate operations. While advancements are being made in this area, with newer systems incorporating haptic feedback to some extent, overcoming the technical challenges associated with replicating the full range of human sensation and intuition remains a work in progress.
While robotic surgery offers transformative benefits for surgical practices, it also presents significant challenges and considerations that must be carefully managed. The high costs, steep learning curve, and technical limitations are substantial obstacles that require ongoing attention and innovation. Addressing these challenges is essential for ensuring that the advantages of robotic surgery can be fully realised and made accessible to a broader range of healthcare providers and patients worldwide.
The Future of Robotic Surgery
The future of robotic surgery is poised at the edge of remarkable advancements, heralding a new era where the boundaries of medical technology and surgical precision are constantly being expanded. As we look into the horizon of possibilities, the integration of enhanced sensory feedback, increased autonomy of surgical robots, and the fusion of artificial intelligence (AI) with surgical planning and execution stand out as key areas poised for significant development. These innovations promise to overcome existing limitations and broaden the scope of robotic surgery, making it an even more integral part of healthcare delivery.
Enhanced Sensory Feedback
One of the most anticipated advancements in robotic surgery is the enhancement of sensory feedback, or haptic feedback, which aims to replicate the sense of touch for the surgeon operating robotic instruments. This technology would allow surgeons to feel the texture, resistance, and other tactile properties of tissues and organs, just as they would in traditional hands-on surgery. The development of sophisticated haptic feedback systems is expected to improve surgical precision and safety further by providing surgeons with a more intuitive understanding of the surgical environment.
Greater Autonomy for Robots
The future also holds promise for the development of surgical robots with greater autonomy. While current robotic systems require direct control by a surgeon, advancements in robotics and AI could lead to systems capable of performing specific tasks independently under the supervision of a surgeon. This increased autonomy could enhance surgical efficiency, reduce the cognitive load on surgeons during complex procedures, and potentially improve outcomes by standardising parts of the surgical process. However, the transition towards more autonomous surgical robots will need to be approached with caution, ensuring that patient safety and the role of the surgeon as the ultimate decision-maker are maintained.
Integration of Artificial Intelligence
Artificial intelligence is set to play a transformative role in the future of robotic surgery. AI can assist in surgical planning by analysing patient data, medical images, and past surgical outcomes to recommend the most effective surgical approach. AI can provide real-time decision-making support during surgery, offering guidance based on the vast surgical knowledge databases and real-time surgical field analysis. This integration of AI can lead to more personalised and precise surgeries, potentially reducing complications and improving patient outcomes.
Conclusion
Robotic surgery stands at the forefront of medical technology, embodying the pinnacle of surgical precision, minimally invasive procedures, and enhanced patient care. As technology continues to evolve, the potential for robotic surgery to transform healthcare is immense. Innovations in sensory feedback, robot autonomy, and AI integration are just the beginning of what is possible, promising to make surgeries safer, more efficient, and more accessible worldwide.
The journey of robotic surgery from a novel concept to a fundamental component of modern surgical practices is a testament to the relentless pursuit of improvement and innovation in healthcare. As we look towards the future, the ongoing development and integration of robotics in surgery are set to revolutionise the field further, offering new possibilities for patient care and opening new frontiers in medical science. With each advancement, robotic surgery reinforces its position as an invaluable tool in the medical arsenal, shaping a future where the benefits of cutting-edge technology are seamlessly integrated into the fabric of healthcare to improve lives and outcomes.
Disclaimer
The information provided in this article is intended for general informational and educational purposes only and does not constitute medical advice, diagnosis, or treatment. While efforts have been made to ensure the accuracy and timeliness of the content, Open Medscience makes no representations or warranties of any kind, express or implied, about the completeness, accuracy, reliability, or suitability of the information contained herein.
Readers should not rely on the information presented in this article as a substitute for professional medical advice or consultation with qualified healthcare professionals. Any decisions regarding medical care or treatment should be made in consultation with a licensed medical practitioner.
Open Medscience does not endorse or promote any specific technologies, companies, or surgical systems mentioned in this article. The inclusion of such references is purely for illustrative and informational purposes.
Use of this article and any reliance on the information contained herein is solely at the reader’s own risk. Open Medscience and its contributors disclaim any liability for any loss or damage arising directly or indirectly from the use of or reliance on the information provided.
home » blog » medical robotics »