This article provides an in-depth exploration of the critical role of neurological diagnostics, examining various techniques like Magnetic Resonance Imaging (MRI), Computed Tomography (CT), Positron Emission Tomography (PET), Functional MRI (fMRI), Diffusion Tensor Imaging (DTI), and magnetic resonance spectroscopy (MRS). Each modality is discussed for its unique contribution to diagnosing and treating brain-related conditions, from emergency response to detailed anatomical and functional analysis. The article addresses challenges such as accuracy, interpretation, accessibility, and ethical considerations in medical imaging. It also highlights the impact of Artificial intelligence (AI) and Machine Learning (ML) in enhancing imaging analysis and the ongoing technological innovations driving the field forward.
Introduction
In the dynamic world of medical diagnostics, the significance of medical imaging in understanding and treating brain-related conditions is unparalleled. As a pivotal element in modern medicine, imaging techniques such as MRI, CT scans, PET scans, and advanced methods like fMRI have revolutionised our grasp of the brain’s complex structure and functionality. This article looks into the multifaceted sphere of brain imaging, exploring various imaging modalities, their specific applications in neurology, and the challenges they present.
We will examine the intricacies of MRI and CT scans, their critical roles in emergency medicine and detailed anatomical study, and the unique insights offered by PET scans in metabolic activity. The article also sheds light on the advanced techniques of DTI and MRS, unveiling their contributions to understanding brain pathologies. Beyond diagnostic capabilities, the discussion extends to the challenges faced in this field, including accuracy, interpretation, accessibility, and ethical considerations.
As we navigate through these aspects, the article also highlights the transformative impact of AI and ML in image analysis and the ongoing innovations that are shaping the future of medical imaging. The article aims to provide a comprehensive understanding of how these technologies aid in accurate diagnosis and effective treatment and pave the way for groundbreaking research and developments in neurology, ultimately enhancing patient outcomes and advancing medical science.
Understanding Brain Imaging Techniques
MRI: A Window into the Brain’s Anatomy
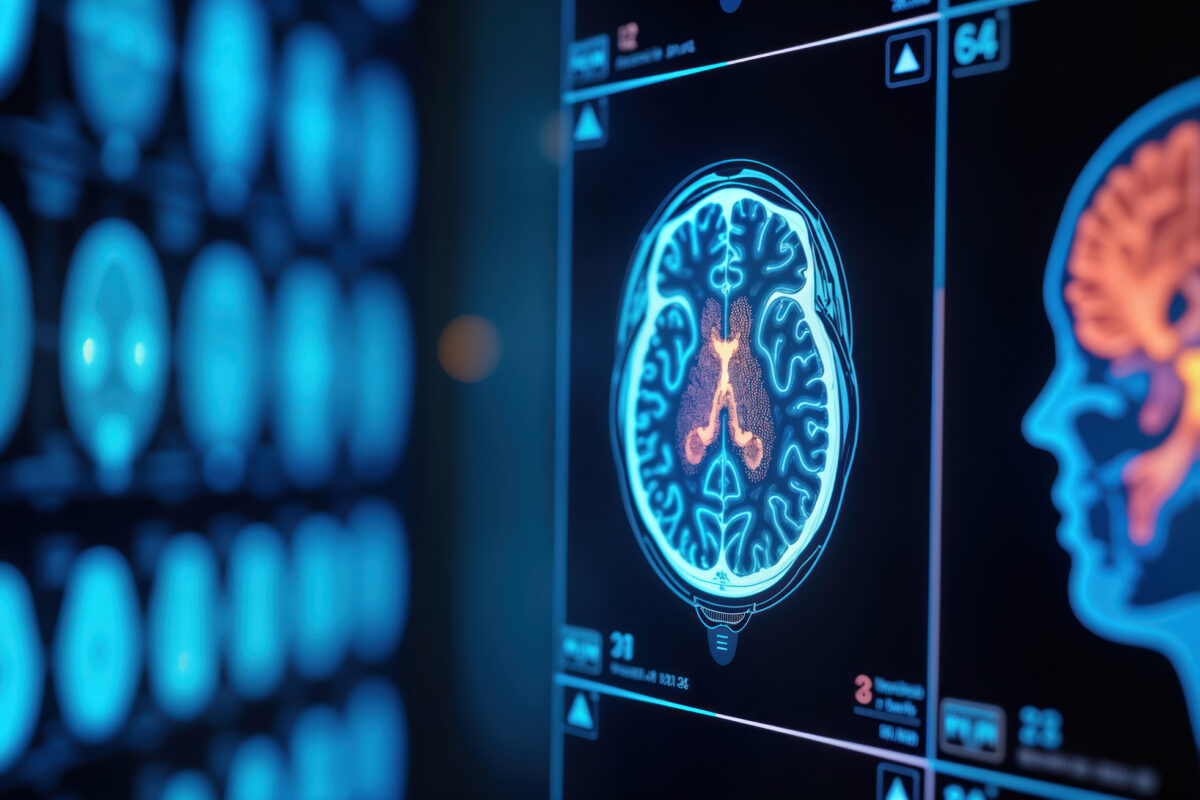
Magnetic Resonance Imaging (MRI) stands as a cornerstone in the area of neurological diagnostics, offering a non-invasive yet profoundly detailed view of the brain’s intricate anatomy. This imaging technique utilises powerful magnetic fields and radio waves to generate detailed images of the brain and spinal cord, surpassing other modalities in its ability to distinguish between different types of soft tissue.
The superior resolution of MRI makes it an invaluable tool in diagnosing a myriad of neurological conditions, from brain tumours and strokes to degenerative diseases such as multiple sclerosis. Unlike CT scans, which rely on X-rays, MRI does not expose patients to ionising radiation, making it a safer option for repeated use, particularly in vulnerable populations like children or pregnant women.
One of MRI’s most significant advantages is its versatility. Different sequences and contrasts can be used to highlight various tissue properties. For instance, T1-weighted images provide excellent anatomical detail, making them ideal for visualising the brain’s structure, while T2-weighted images are adept at detecting changes in tissue composition, often indicative of pathology. Moreover, diffusion-weighted imaging (DWI) can detect acute ischemic strokes within minutes of symptom onset by highlighting areas of restricted water movement in the brain.
Functional MRI (fMRI) extends the capabilities of traditional MRI by mapping brain activity. By detecting changes in blood flow related to neuronal activity, fMRI can offer insights into the brain’s functional anatomy, aiding in both research and clinical settings. This has been pivotal in pre-surgical planning, especially in operations where critical functional areas of the brain are at risk.
MRI serves as a critical window into the brain’s anatomy, providing detailed images that are essential for accurate diagnosis and treatment planning in neurology. Its ongoing advancements continue to enhance our understanding of the brain, solidifying its role in modern medicine.
CT Scans: Fast and Effective for Emergency Situations
In the fast-paced environment of emergency medicine, Computed Tomography (CT) scans are invaluable for their speed and effectiveness in diagnosing acute brain conditions. This imaging modality utilises X-ray technology to create detailed cross-sectional images of the brain, allowing clinicians to quickly assess and respond to critical situations such as head injuries, strokes, and brain haemorrhages.
The speed with which a CT scan can be performed and interpreted is a key advantage, particularly in emergency settings where time is of the essence. Unlike MRI, which can take up to an hour, a brain CT scan can be completed within minutes. This swift turnaround time is crucial in conditions like acute ischemic stroke, where the treatment window is narrow and rapid intervention can significantly influence patient outcomes.
CT scans are particularly effective in detecting haemorrhages, skull fractures, and other structural abnormalities. In cases of trauma, a CT scan can quickly reveal internal bleeding or swelling in the brain, guiding immediate treatment decisions. For stroke patients, CT scans help differentiate between ischemic and haemorrhagic strokes, which is vital for determining the appropriate therapy, such as thrombolysis for ischemic strokes.
Additionally, CT scans are more readily available than MRI in many healthcare settings, making them more accessible during emergencies. They are also more accommodating for patients who may have contraindications to MRI, such as those with implanted medical devices or severe claustrophobia.
However, it’s important to note that CT scans do involve exposure to ionising radiation, and while the risk is generally low, it is a consideration in their use, especially for repeated scans. Despite this, the benefits in urgent care situations often outweigh the risks.
CT scans are critical in emergency medicine, providing rapid, effective, and life-saving diagnostics for various brain-related emergencies. Their ability to quickly deliver crucial information makes them indispensable in acute care scenarios.
PET Scans: Unravelling Metabolic Activities
Positron Emission Tomography (PET) scans represent a unique and advanced imaging technique, primarily distinguished by their ability to visualise metabolic processes within the brain. Unlike MRI and CT scans, which primarily provide anatomical details, PET scans probe into the functional aspects of the brain, offering a window into its metabolic activity.
PET scans use a radioactive tracer, typically a form of glucose, injected into the patient’s bloodstream. As the brain engages in various activities, it consumes glucose, allowing the PET scan to detect high and low metabolic activity areas. This characteristic makes PET scans particularly useful in identifying functional abnormalities that are often associated with various neurological disorders.
In the field of neurology, PET scans have become crucial in diagnosing and monitoring conditions like Alzheimer’s disease, Parkinson’s disease, and epilepsy. For instance, in Alzheimer’s disease, PET scans can detect early changes in the brain’s glucose metabolism, even before significant memory loss occurs. This early detection is vital for timely intervention and management of the disease.
PET scans also play a significant role in oncology, especially in diagnosing and staging brain tumours. They help distinguish between benign and malignant tumours and provide critical information about the tumour’s metabolic activity, which can guide treatment planning.
Moreover, PET scans are instrumental in research, enhancing our understanding of brain function and various neurological conditions. They have been pivotal in studying brain activity related to cognition, emotion, and various psychiatric disorders, offering insights that are not possible with other imaging modalities.
Despite their benefits, PET scans are not without limitations. They are generally more expensive and less accessible than other imaging techniques. Additionally, the use of radioactive tracers requires careful consideration, particularly in certain patient populations.
PET scans are a powerful tool in modern medicine, unravelling the complex metabolic activities of the brain. They provide critical insights into various neurological conditions, aiding in diagnosis, treatment planning, and research, thus enhancing our overall understanding of brain function and health.
Functional MRI (fMRI): Decoding Brain Activity
Functional Magnetic Resonance Imaging (fMRI) represents a significant advancement in neuroimaging, offering an unparalleled view of the functioning brain. Unlike traditional MRI, which provides static images, fMRI captures the dynamic aspect of brain activity, allowing scientists and clinicians to observe the brain in action.
fMRI operates on the principle of detecting changes in blood flow to various parts of the brain, a concept known as neurovascular coupling. When a brain region is more active, it consumes more oxygen, leading to increased blood flow to that area. fMRI tracks these changes through the Blood Oxygen Level Dependent (BOLD) contrast, effectively mapping brain activity in response to various stimuli or tasks.
This ability to monitor brain function in real-time has profound implications in both clinical and research settings. In clinical practice, fMRI is extensively used for brain mapping prior to neurosurgery. It identifies critical regions responsible for speech, movement, vision, and other essential functions, thereby aiding surgeons in planning procedures that minimise damage to these vital areas.
In the area of research, fMRI has opened new frontiers in understanding the brain’s complexities. It has been pivotal in cognitive neuroscience, exploring how different brain regions are involved in memory, emotion, language, and decision-making. Moreover, fMRI has contributed significantly to the study of neurological disorders such as autism, schizophrenia, and depression, providing insights into the neural underpinnings of these conditions.
One of the main advantages of fMRI is that it is non-invasive and does not involve exposure to ionising radiation, making it safe for repeated studies over time. This aspect is particularly beneficial for longitudinal studies tracking brain development or the progression of neurological disorders.
However, fMRI also has its limitations, including sensitivity to motion artefacts and the need for complex data analysis. Its high resolution is both a strength and a challenge, as interpreting the vast amount of data generated requires sophisticated analytical techniques.
fMRI has revolutionised our ability to decode brain activity, offering invaluable insights into both normal brain function and the pathology of various neurological disorders. Its contributions to both clinical neurology and neuroscience research continue to be of paramount importance.
Advanced Techniques: DTI and MRS
In the ever-evolving field of neuroimaging, advanced techniques like Diffusion Tensor Imaging (DTI) and Magnetic Resonance Spectroscopy (MRS) have emerged, offering deeper insights into the brain’s structure and chemistry. These sophisticated methods extend beyond conventional imaging, providing detailed information that aids in diagnosing and understanding neurological disorders.
Diffusion Tensor Imaging (DTI)
DTI is a form of MRI that maps the diffusion of water molecules in biological tissues, primarily used to visualise white matter tracts in the brain. White matter consists of axons, the long nerve fibres that connect different brain regions. The unique aspect of DTI lies in its ability to trace the direction of water molecule movement, which tends to occur along these axons. This characteristic enables DTI to produce a three-dimensional view of the brain’s connectivity, illustrating the pathways that link various regions.
This imaging technique is especially valuable in assessing conditions that affect brain connectivity, such as multiple sclerosis, stroke, and traumatic brain injuries. DTI can detect subtle changes in white matter integrity, which might not be visible on standard MRI. In neurosurgical planning, DTI aids surgeons in avoiding critical white matter tracts during operations, thereby reducing the risk of post-surgical neurological deficits.
Magnetic Resonance Spectroscopy (MRS)
Magnetic Resonance Spectroscopy (MRS) is another advanced form of MRI, but instead of imaging, it provides a spectrum that represents the concentration of various chemicals in the brain. This technique is akin to a ‘chemical biopsy’ without the need for an actual tissue sample. MRS can measure the levels of certain metabolites, such as N-acetyl aspartate, choline, and lactate, providing information about the brain’s biochemical environment.
Clinically, MRS has been instrumental in differentiating between tumorous and non-tumorous lesions in the brain, helping in the diagnosis and treatment planning of brain tumours. It also plays a role in understanding neurodegenerative diseases, such as Alzheimer’s, by detecting alterations in brain chemistry associated with these conditions.
Both DTI and MRS exemplify the significant strides made in neuroimaging. They offer a more nuanced understanding of the brain’s structure and function, facilitating improved diagnosis, treatment planning, and research in various neurological disorders. These techniques continue to evolve, promising even greater contributions to the field of neuroscience and clinical neurology.
Applications of Brain Imaging
Diagnosing Neurological Disorders
The diagnosis of neurological disorders is a complex process that relies heavily on advances in neuroimaging technologies. Conditions affecting the brain and nervous system, ranging from strokes and brain tumours to degenerative diseases like Alzheimer’s and Parkinson’s, present unique diagnostic challenges. Accurate and early diagnosis is crucial for effective treatment and management.
Magnetic Resonance Imaging (MRI) is pivotal in diagnosing many neurological disorders due to its high-resolution images of brain structures. MRI can identify anomalies in brain tissue and blood vessels, aiding in the detection of conditions such as brain tumours, multiple sclerosis, and strokes. Functional MRI (fMRI) further extends these capabilities by mapping brain activity, providing insights into abnormalities in brain function.
Computed Tomography (CT) scans are invaluable for their speed and efficiency in emergency settings. They are particularly effective in identifying acute conditions like haemorrhagic strokes and traumatic brain injuries, where rapid diagnosis is critical for patient outcomes.
Advanced techniques like Diffusion Tensor Imaging (DTI) and Magnetic Resonance Spectroscopy (MRS) offer further precision. DTI is useful in assessing white matter integrity, crucial for conditions like traumatic brain injury, while MRS provides a ‘chemical snapshot’ of the brain, assisting in the differentiation of tumorous and non-tumorous brain lesions.
Combined with clinical evaluation and laboratory tests, these imaging techniques form the cornerstone of diagnosing neurological disorders. They facilitate accurate diagnosis and aid in monitoring disease progression and assessing treatment efficacy, significantly impacting patient care in neurology.
Monitoring Treatment Progress
In the management of neurological disorders, monitoring treatment progress is as crucial as making an accurate diagnosis. Advances in medical imaging have significantly enhanced our ability to track the effectiveness of treatments, leading to more informed clinical decisions and better patient outcomes.
Magnetic Resonance Imaging (MRI) plays a central role in this process. For instance, in patients with multiple sclerosis, repeated MRI scans can track the appearance of new lesions or changes in existing ones, providing insights into the disease’s progression or remission. This information is vital in assessing the efficacy of therapeutic interventions and, if necessary, adjusting treatment plans.
In the context of brain tumours, both MRI and CT scans are instrumental in monitoring tumour size and response to treatments like chemotherapy, radiation, or surgery. Post-treatment scans can detect reductions in tumour size or changes in its characteristics, indicating the treatment’s effectiveness or, conversely, the need for a different therapeutic approach.
Functional MRI (fMRI) and Positron Emission Tomography (PET) scans extend beyond structural imaging, allowing clinicians to observe changes in brain activity or metabolism following treatments, particularly in conditions like epilepsy or after neurosurgical interventions.
Such continuous monitoring is crucial for evaluating the immediate effects of treatments and the long-term management of chronic neurological conditions. By regularly assessing changes in the brain, healthcare providers can make more informed decisions, tailor treatments to individual patient needs, and significantly improve the quality of life for those living with neurological disorders.
Research and Brain Mapping
In the sphere of neuroscience, research and brain mapping are pivotal in unravelling the mysteries of the brain’s structure and function. Advanced neuroimaging technologies have transformed our understanding of the brain, enabling detailed visualisation and analysis that were once thought impossible.
Functional Magnetic Resonance Imaging (fMRI) has been a game-changer in brain mapping. By detecting changes in blood flow associated with neural activity, fMRI allows researchers to observe which areas of the brain are involved in specific tasks, such as language processing, memory recall, or motor functions. This has led to the creation of detailed brain maps showcasing the diverse functionalities of different brain regions.
Diffusion Tensor Imaging (DTI) offers another layer of insight, mapping the white matter tracts that connect various brain regions. This imaging technique is crucial in studying brain network connectivity and understanding how different parts of the brain communicate.
Brain mapping research has profound implications, not only in understanding normal brain function but also in exploring the pathological mechanisms of neurological disorders like Alzheimer’s disease, autism, and schizophrenia. Such research paves the way for developing targeted therapies and interventions, potentially leading to breakthroughs in treating these complex conditions.
Moreover, brain mapping has significant applications in neurosurgery and cognitive neuroscience, providing a detailed roadmap of the brain that assists in surgical planning and enhances our understanding of cognitive processes. The continuous advancements in neuroimaging and brain mapping are key to unlocking further secrets of the brain, representing one of the most exciting and rapidly evolving areas in medical science.
Neurosurgical Planning and Guidance
Neurosurgical planning and guidance are critical components of successful brain surgery, where precision is paramount. The advancements in neuroimaging techniques have significantly enhanced the ability to plan and guide neurosurgical procedures, reducing risks and improving outcomes.
Magnetic Resonance Imaging (MRI), including functional MRI (fMRI), plays a vital role in pre-surgical planning. By providing high-resolution images of brain anatomy and functional areas, MRI enables surgeons to map out critical regions, such as those responsible for speech, motor functions, and sensory processing. This information is crucial to avoid damaging these essential areas during surgery.
Diffusion Tensor Imaging (DTI) further aids neurosurgeons by mapping the white matter tracts, the brain’s communication highways. This information helps preserve these pathways during surgeries for tumours or epilepsy, thereby maintaining vital neurological functions.
Intraoperative MRI is another groundbreaking development. It allows surgeons to view the brain during surgery, offering real-time feedback and the ability to adjust their approach as needed. This technology is particularly beneficial in ensuring the complete removal of tumour tissue while minimising damage to healthy brain areas.
Neuro-navigation systems, which use preoperative imaging data to guide surgical instruments in real-time, have also become a standard in modern neurosurgery. These systems enhance the surgeon’s precision, significantly improving safety and efficacy.
Current advances in imaging technologies have revolutionised neurosurgical planning and guidance. They provide critical insights that enable neurosurgeons to perform complex procedures with greater accuracy and confidence, leading to better patient outcomes and reduced surgical risks.
Challenges in Brain Imaging
Accuracy and Interpretation Difficulties
Accuracy and interpretation difficulties remain significant challenges in the field of medical imaging. Despite technological advancements, the complexity of the human brain and the subtleties of various diseases present ongoing obstacles.
One primary issue is the potential for false positives or negatives. For instance, in MRI and CT scans, benign anomalies may appear suspicious, leading to unnecessary anxiety or interventions, whereas small or early-stage pathologies might go undetected. Similarly, in functional imaging like fMRI or PET scans, interpreting the brain’s metabolic and functional signals can be complex, requiring high levels of expertise and often subject to variability.
The quality of imaging also plays a crucial role in accuracy. Factors such as machine calibration, image resolution, and patient movement can affect the images’ quality. In neuroimaging, where minute details are crucial, these factors can significantly impact the diagnosis and treatment plan.
Moreover, the interpretation of medical images relies heavily on the experience and skill of radiologists and clinicians. Subtle signs of disease might be overlooked or misinterpreted, particularly in less common conditions or in cases where symptoms are atypical. This challenge highlights the need for continuous training and development in radiological expertise.
While medical imaging is a powerful diagnostic tool, it is not infallible. The challenges of accuracy and interpretation require a combination of high-quality imaging technology, skilled professionals, and, often, a multidisciplinary approach to ensure patients’ most accurate and beneficial outcomes.
Accessibility and Cost Considerations
The accessibility and cost of medical imaging are significant factors that influence patient care worldwide. Advanced imaging techniques like MRI, CT scans, and PET are integral in diagnosing and treating numerous conditions. However, their availability and affordability pose challenges, particularly in resource-limited settings.
High-end imaging equipment is expensive to purchase and maintain, often necessitating substantial investment in infrastructure and trained personnel. This financial burden can limit the availability of such facilities, especially in low- and middle-income countries, leading to disparities in healthcare access. Even in developed countries, the high cost of these procedures can be a barrier, with expenses sometimes not fully covered by insurance plans, placing a financial strain on patients.
Geographical factors also impact accessibility. In rural or remote areas, the lack of nearby imaging facilities means patients may need to travel long distances for essential scans, adding to the cost and inconvenience. This situation can lead to delays in diagnosis and treatment, adversely affecting patient outcomes.
Furthermore, the cost implications extend to research and development in medical imaging. The high cost of developing and testing new imaging technologies can slow their adoption and availability, potentially delaying the benefits of these advancements to patient care.
Medical imaging is a cornerstone of modern diagnostics and treatment, but issues of accessibility and cost remain significant hurdles. Addressing these challenges requires a multifaceted approach, including policy changes, technological innovations, and international collaboration, to ensure equitable access to these vital healthcare services.
Ethical and Privacy Concerns
While invaluable in diagnosis and treatment, medical imaging raises ethical and privacy concerns that must be judiciously managed. The increasing use of advanced imaging technologies like MRI, CT scans, and PET brings with it the need to balance medical benefits against potential ethical dilemmas and privacy issues.
One major concern is the handling of sensitive patient data. Medical images contain detailed information about an individual’s health status, which is confidential. Ensuring the security and privacy of this data in an era of electronic health records and digital storage is crucial. Data breaches or unauthorised access can lead to privacy violations and potential misuse of personal health information.
Another ethical consideration is informed consent, particularly in the context of novel or experimental imaging techniques. Patients must be adequately informed about the nature of imaging procedures and their benefits and risks. This is especially pertinent in research settings, where the implications of new imaging technologies may not be fully understood.
Additionally, there are concerns about the overuse of imaging for diagnostic purposes, sometimes driven by fear of legal repercussions (defensive medicine) or patient demand, leading to unnecessary exposure to radiation (in the case of CT scans) or unwarranted healthcare costs.
In paediatric imaging, ethical considerations are even more pronounced, as children may not fully understand the procedures and parents/guardians must make decisions in the child’s best interest.
Addressing these ethical and privacy concerns requires robust protocols for data handling, clear communication with patients regarding the risks and benefits of imaging procedures, and adherence to stringent ethical standards, particularly in research and clinical trials. Ensuring that these aspects are diligently managed is essential for maintaining trust in medical imaging as a critical tool in healthcare.
Technical Limitations and Need for Specialised Training
Notwithstanding its advancements, medical imaging is not without technical limitations and demands for specialised training. These challenges are pivotal in determining the quality and effectiveness of diagnostic imaging.
One significant technical limitation is image resolution. Even with high-end equipment like MRI or CT scanners, there are limits to the fineness of detail that can be captured. This can be particularly challenging when trying to detect very small lesions or subtle pathological changes. Furthermore, patient movement, even slight, can lead to artefacts that obscure critical details, impacting the accuracy of diagnoses.
Another limitation is the differentiation between various types of tissues or pathologies. For instance, distinguishing between tumour types or differentiating post-treatment scar tissue from residual disease can be challenging and sometimes requires complementary imaging modalities or follow-up scans.
The complexity of these imaging technologies also necessitates specialised training for both the operators and the interpreting radiologists or physicians. Proper operation of the equipment, understanding the nuances of each imaging modality, and accurately interpreting the results requires extensive knowledge and experience. This need for specialised training can impact the availability of skilled professionals, particularly in less developed or rural areas.
Moreover, with the rapid evolution of imaging technologies, ongoing training and education have become essential to stay abreast of the latest advancements and their clinical applications. Ensuring that healthcare professionals are adequately trained is crucial for the effective and safe use of medical imaging in patient care.
The Future of Brain Imaging
AI and Machine Learning in Image Analysis
The integration of Artificial Intelligence (AI) and Machine Learning (ML) in image analysis is revolutionising the field of medical imaging. These technologies offer significant advancements in imaging studies’ accuracy, efficiency, and diagnostic capabilities.
AI and ML algorithms can analyse complex medical images with a level of precision and speed unattainable by human eyes. These systems are trained on vast datasets of medical images, enabling them to recognise patterns and abnormalities, such as tumours, fractures, or signs of neurological diseases, often with greater accuracy and consistency than traditional methods.
One of the key benefits of AI in imaging is its ability to reduce the time for image interpretation. This speed is critical in emergency situations, like stroke or trauma, where rapid diagnosis can dramatically affect patient outcomes. AI algorithms can also assist in reducing the rates of false positives and negatives, thereby improving the reliability of diagnostic processes.
Moreover, AI is instrumental in handling the massive volumes of data generated by modern imaging techniques. It can sift through thousands of images, prioritising those that require urgent attention, thereby enhancing workflow efficiency and reducing clinician burnout.
In research, AI-powered image analysis is unlocking new insights into disease progression and treatment responses, facilitating the development of personalised medicine approaches.
However, the adoption of AI in medical imaging also raises questions about data privacy, the need for robust training datasets, and the potential for algorithmic bias. Despite these challenges, the integration of AI and ML into medical imaging is poised to transform the landscape of disease diagnosis and management, offering promising prospects for future healthcare advancements.
Innovations in Imaging Technologies
The field of medical imaging is witnessing rapid advancements, driven by the quest to improve diagnostic accuracy, patient safety, and treatment efficacy. These innovations are reshaping how clinicians diagnose and manage diseases.
One significant breakthrough is the development of higher-resolution imaging technologies. For instance, ultra-high-field MRI scanners, operating at 7 Tesla or higher, offer unprecedented detail in brain imaging, revealing structures and pathologies that were previously indiscernible. This level of detail is crucial in diagnosing and understanding complex neurological disorders.
Another area of innovation is in functional imaging techniques. Advanced PET scan technologies and novel tracers enable more precise mapping of metabolic processes, providing insights into various conditions, from cancer to neurodegenerative diseases. Hybrid imaging systems, like PET/MRI, combine the strengths of both modalities, offering comprehensive structural and functional information in a single session.
Artificial intelligence and machine learning are also transforming imaging. These technologies enhance image processing, automate routine tasks, and improve diagnostic accuracy by identifying patterns that the human eye might miss. AI algorithms are increasingly used for predictive analysis, aiding in early disease detection and personalised treatment planning.
Moreover, there is a growing focus on minimally invasive imaging techniques, reducing patient exposure to radiation and improving comfort. Portable imaging devices are another emerging trend, increasing accessibility, especially in remote or underserved regions.
These innovations in imaging technologies are enhancing diagnostic capabilities and paving the way for new therapeutic approaches and personalised medicine, marking a new era in healthcare.
Personalised Medicine and Predictive Diagnostics
Personalised medicine and predictive diagnostics are at the forefront of a healthcare revolution, reshaping disease treatment and prevention approaches. Medical imaging and genetic profiling advances largely drive this paradigm shift, enabling more tailored and effective healthcare strategies.
At the core of personalised medicine is the concept of individualised treatment plans based on a patient’s unique biological characteristics. Medical imaging plays a crucial role in this, providing detailed insights into the individual’s specific disease pathology. For instance, advanced imaging techniques can identify a tumour’s precise location and characteristics, guiding targeted therapies and improving treatment outcomes.
Predictive diagnostics, another pillar of personalised medicine, involves identifying the likelihood of developing a disease before it manifests. Here, imaging technologies combined with genetic testing and AI analysis allow for early detection of risk factors or early-stage disease. This early intervention can lead to more effective management, potentially halting or slowing disease progression.
Furthermore, imaging biomarkers are increasingly used to monitor treatment response and adjust therapies in real-time. This approach ensures that patients receive the most effective treatments based on their evolving condition, reducing the trial-and-error nature of medical interventions.
Personalised medicine and predictive diagnostics represent a shift towards more patient-centric healthcare. By leveraging the power of advanced imaging and other technologies, this approach promises improved outcomes, reduced side effects, and more efficient use of healthcare resources, heralding a new era in medical treatment and disease management.
Ethical Implications and Regulations
The advancements in medical imaging bring forth a range of ethical implications and necessitate stringent regulations to safeguard patient rights and ensure the responsible use of these technologies. Ethical considerations primarily revolve around patient consent, data privacy, and the equitable distribution of these advanced technologies.
Informed consent is a cornerstone of ethical medical practice, especially important in imaging procedures that may involve exposure to radiation or the use of contrast agents. Patients must be fully informed about the risks, benefits, and alternatives to the procedures. This is especially crucial in research settings or when using novel imaging technologies.
Data privacy and security are paramount, given the sensitive nature of medical images. With the increasing digitisation of medical records, ensuring the protection of patient data against unauthorised access or breaches is a major concern. Regulations such as the Health Insurance Portability and Accountability Act (HIPAA) in the U.S. and the General Data Protection Regulation (GDPR) in the EU set data handling and privacy standards.
Additionally, there is a moral obligation to ensure equitable access to advanced imaging technologies. Disparities in access, both globally and within countries, raise ethical concerns. Regulations and policies must strive to balance the distribution of these resources, ensuring that advancements in medical imaging are available to all sections of society.
Finally, ethical guidelines and regulatory bodies are essential in overseeing the development and application of AI in medical imaging, addressing issues like algorithmic bias and ensuring algorithms are trained on diverse datasets.
The ethical implications and regulations in medical imaging are critical in guiding the responsible and equitable use of these technologies, protecting patient rights, and ensuring that the benefits of advancements in imaging are shared across diverse populations.
Practical Aspects and Patient Care
Preparing for a Brain Imaging Procedure
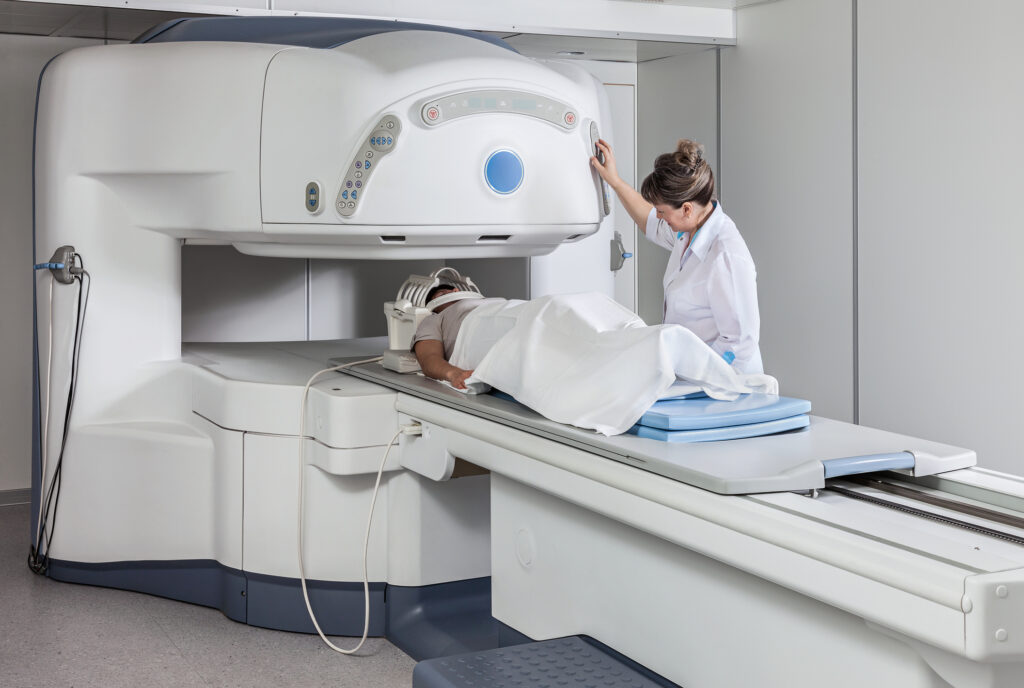
Preparing for a brain imaging procedure, such as an MRI or CT scan, is important to ensure accurate results and patient comfort. The preparation largely depends on the type of imaging being performed and the specific protocols of the healthcare facility.
For MRI scans, patients are usually asked to remove any metal objects, including jewellery, glasses, and hearing aids, as the MRI machine uses strong magnetic fields. Patients with metal implants, pacemakers, or metal fragments in their body must notify their doctor, as these can pose risks or affect image quality. In some cases, a contrast dye may be used to enhance the images. Patients might be instructed to fast for a few hours before the scan if a contrast material is to be used.
For CT scans, similar precautions about metal objects apply. If a contrast dye is required, fasting may be necessary, and patients with allergies or kidney problems should inform their healthcare provider, as the dye can cause adverse reactions in susceptible individuals.
Patients are often advised to wear comfortable, loose-fitting clothing and may be provided with a gown. It’s important to follow any specific instructions regarding medication; some may need to be discontinued temporarily before the imaging.
Anxiety or claustrophobia is common, especially for MRI procedures. Patients should discuss any concerns with their healthcare provider, who can suggest relaxation techniques or sometimes provide sedation.
Overall, clear communication with the healthcare team and adherence to specific instructions are key to a smooth and effective brain imaging procedure.
Understanding the Risks and Benefits
Medical imaging procedures, such as MRI, CT scans, and PET scans, have become indispensable tools in modern healthcare, offering crucial insights for diagnosis and treatment. However, patients and healthcare providers need to weigh the risks and benefits to make informed decisions.
The primary benefit of medical imaging is its ability to provide detailed information about the body’s internal structures and functions, often non-invasively. This allows for accurate diagnosis, disease progression monitoring, and treatment efficacy assessment. Imaging can detect abnormalities early, significantly improving the chances of successful treatment.
However, certain risks are associated with some imaging procedures. For instance, CT scans and PET scans involve exposure to ionising radiation. While the radiation dose is generally low and the risk of harm is small, it is a consideration, particularly in children or for individuals requiring multiple scans. MRI, on the other hand, doesn’t use ionising radiation, but the use of contrast agents can pose risks for patients with kidney issues or allergies.
MRI can be hazardous for patients with implants, pacemakers, or metal fragments in their body due to its strong magnetic fields. Additionally, some patients may experience discomfort or anxiety, particularly in the confined space of an MRI machine.
Medical imaging is a powerful diagnostic tool, and understanding its risks and benefits is essential. Patients should have a thorough discussion with their healthcare provider about the necessity, safety, and potential implications of imaging procedures, ensuring that their use is justified and tailored to individual health needs.
Patient-Centred Care in Imaging
Patient-centred care in medical imaging emphasises individualised attention, respect, and engagement in decision-making processes, ensuring that imaging procedures align with the patient’s unique needs and preferences. This approach is crucial in enhancing patient experience and outcomes.
In patient-centred imaging, clear and empathetic communication is key. Healthcare providers must ensure that patients understand the imaging procedure’s purpose, process, and potential risks. This involves explaining the necessity of the imaging, what the procedure entails, and addressing any concerns or fears, particularly in procedures like MRI, where patients might experience claustrophobia.
Respect for patient privacy and dignity is also essential, especially when patients are required to change into hospital gowns. Efforts should be made to maintain their comfort and modesty throughout the procedure.
Patient-centred care also involves accommodating individual needs. For instance, providing earplugs or music during an MRI scan can help alleviate discomfort from the machine’s noise. For anxious patients, options like sedation or the presence of a companion can be considered.
Moreover, scheduling and conducting imaging procedures should be done with an eye towards minimising disruptions to patients’ lives. Efficient scheduling, reducing waiting times, and ensuring timely communication of results can significantly improve the patient’s experience.
However, patient-centred care in medical imaging is about more than just delivering high-quality diagnostic images; it’s about ensuring a compassionate, respectful, and responsive service that acknowledges and addresses each patient’s unique concerns, needs, and preferences.
Post-Imaging Follow-Up and Treatment Options
The period following a medical imaging procedure is crucial in determining the next steps in a patient’s healthcare journey. Post-imaging follow-up and discussing treatment options are integral to this process, ensuring that patients receive comprehensive care based on their imaging results.
Radiologists analyse the images and provide a detailed report after an imaging session, such as an MRI or CT scan. It’s essential for patients to have a follow-up appointment with their healthcare provider to discuss these findings. During this consultation, the healthcare provider should explain the results in understandable terms, clarifying any abnormalities or concerns observed in the images.
The healthcare provider should outline the available options if the imaging reveals a condition requiring treatment. This discussion should encompass various aspects, including the nature and severity of the condition, recommended treatments or interventions, potential risks and benefits, and expected outcomes. Referrals to specialists may be necessary for more targeted care for complex conditions.
In cases where imaging results are inconclusive or reveal the need for further evaluation, additional tests or repeat imaging may be recommended. It’s vital for patients to understand the reasons for these additional procedures and how they contribute to their overall care plan.
Patient involvement in decision-making is a key aspect of this stage. Healthcare providers should encourage patients to ask questions and express their preferences and concerns. This collaborative approach ensures that the chosen treatment plan aligns with the patient’s needs, values, and lifestyle, ultimately leading to more satisfactory healthcare outcomes.
Conclusion
The landscape of medical imaging is vast and multifaceted, playing a crucial role in modern healthcare. These technologies are indispensable in diagnosing and treating neurological disorders, from the intricate details revealed by MRI and CT scans to the functional insights provided by PET scans and fMRI. Advanced techniques like DTI and MRS further augment our understanding of brain pathologies. While the benefits of these imaging modalities are immense in diagnosing neurological conditions, monitoring treatment progress, and aiding in neurosurgical planning, they are not without challenges. Issues such as accuracy, interpretation difficulties, accessibility, costs, and ethical concerns underscore the need for continuous advancement and prudent application. The integration of AI and ML in image analysis and the ongoing innovations promise to enhance the precision and efficacy of these tools. As medical imaging evolves, it remains a cornerstone in the shift towards personalised medicine and predictive diagnostics, ensuring patient-centred care and paving the way for future breakthroughs in medical science.
Disclaimer
The content of this article, The Role of Medical Imaging in Neurological Diagnostics, is intended for informational and educational purposes only. It does not constitute medical advice, diagnosis, or treatment recommendations. Readers should not rely solely on the information provided herein for making healthcare decisions. Always seek the guidance of qualified medical professionals regarding any medical condition or imaging procedure.
Open Medscience and its contributors make every effort to ensure that the information contained in this publication is accurate and up to date at the time of writing. However, medical knowledge and practices evolve rapidly, and the accuracy or completeness of the content cannot be guaranteed over time.
Any references to specific imaging modalities, technologies, or treatment approaches are provided for general understanding and do not imply endorsement or preference by Open Medscience. Inclusion of emerging technologies such as Artificial Intelligence (AI) and Machine Learning (ML) is for illustrative purposes only and does not reflect clinical validation or regulatory approval in all jurisdictions.
Open Medscience accepts no responsibility or liability for any loss or damage resulting from reliance on the information contained in this article. Readers are encouraged to consult with appropriate healthcare professionals before making any decisions related to medical imaging or neurological care.
home » blog » medical imaging topics »