Magnetic Resonance Imaging
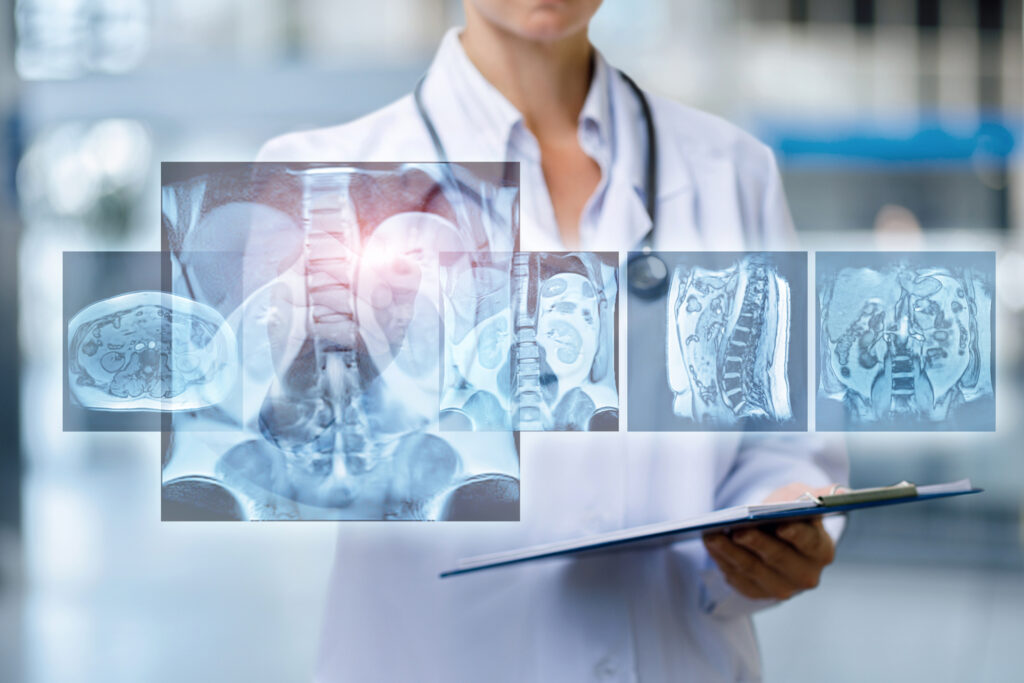
Magnetic Resonance Imaging (MRI) is a non-invasive imaging modality that produces 3-D anatomical images. Its primary medical purpose is to detect and diagnose disease and plan treatment. The principle of MRI technology is the excitation of protons and its ability to detect these changes in the direction of the rotational axis of protons found in the water that makes up living tissues.
MRI is a possible diagnostic tool for peripheral artery disease (PAD), which affects about 202 million people worldwide. Usually, the diagnosis of PAD is confirmed by reviewing the patient’s history, followed by a physical examination. In this case, an MRI would be beneficial in determining the degree of disease and provide anatomical details of atherosclerotic plaque, which results in perfusion limitation.
Therefore, MRI research has focussed on non-contrast MRI techniques and hybrid systems which use contrast-enhanced MR angiography (CE-MRA). The basis of PAD imaging considers improving spatial resolution and obtaining accurate dynamic data in ais to improve the contrast agent duriobtainalysis of skeletal muscle perfusion. However, the gold standard for skeletal muscle perfusion assessment is applying the highly invasive microsphere technique that requires arterial and tissue sampling.
Also, gadolinium-enhanced MRI of skeletal muscle perfusion can be performed on patients with peripheral artery disease using a plantarflexion ergometer sequence. This procedure uses a T1-weighted sequence to image the gadolinium-based contrast agent being accumulated by the tissue. This technique is similar to MRI myocardial perfusion and can be used with the arterial input function. The procedure is equivalent to the 6-minute walk test to diagnose PAD in patients.
Furthermore, arterial spin labelling (ASL) is a non-contrast technique. The protons in the arterial blood are influenced by a magnetic tag which causes a different magnetisation from the surrounding soft tissue. The ASL approach has been successfully demonstrated for perfusion abnormalities in PAD patients.
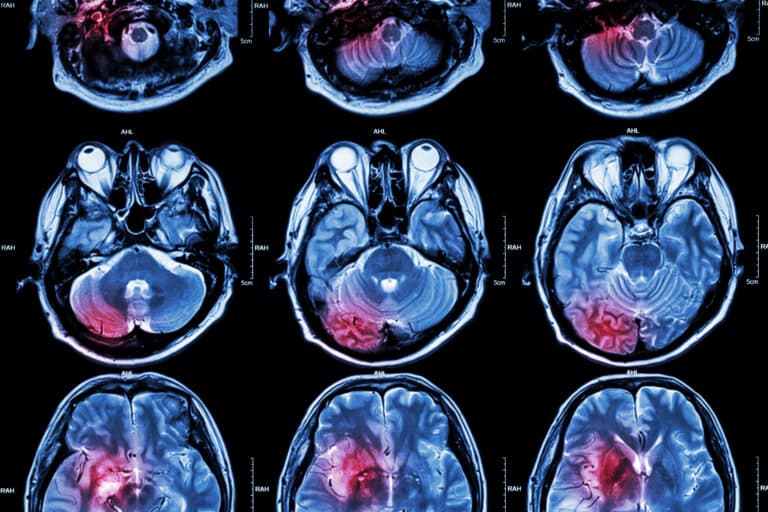
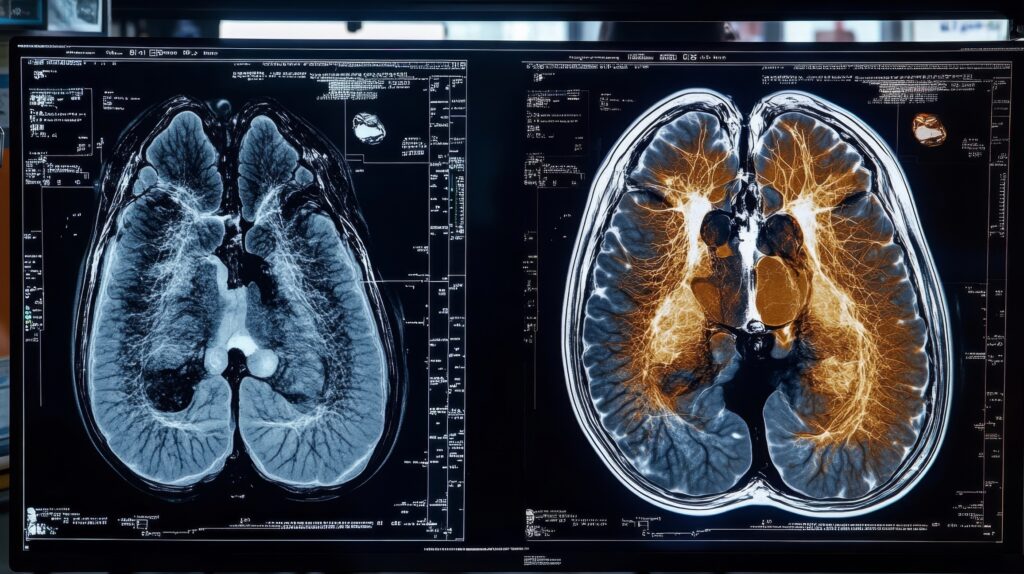
Another method of PAD imaging is based on a relative measure of tissue oxygenation called blood-oxygen-level-dependent MRI (BOLD MRI). The BOLD MRI technique has been used to assess brain activation and oxygenation of skeletal muscle, including the kidneys. Also, phosphorus-31 magnetic resonance spectroscopy has been used to measure skeletal muscle metabolism.
However, catheter angiography remains the gold standard for the diagnosis of PAD. Consequently, MRI still has limitations, such as limited availability of advanced MRI sequences, prolonged acquisition times and financial considerations.
home » magnetic resonance imaging